Currently ileocolonoscopy remains the gold standard technique to evaluate CD recurrence in patients who have undergone ileocolic resection.
Nevertheless,
endoscopy is an invasive method that frequently needs patient's sedation or anaesthesia.
In addition,
it may also be incomplete due to modified anatomy and luminal narrowing in correspondence to the anastomotic site,
preventing the progression of the endoscope in approximately one-third of cases [3,
9].
In such situations,
endoscopy allows for an evaluation limited to the colonic side of the anastomosis.
On the other hand,
the assessment of the neoterminal ileum is of great clinical value,
because CD recurrence mainly involves the ileal side of the ileocolic anastomosis [1],
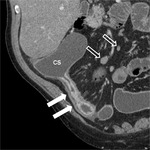
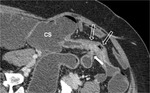
and imaging plays an important role in this concern (Figure 6).
Both CT-enterography and CT-enteroclysis have been used to evaluate CD patients with suspected anastomotic recurrence.
In a previous work [11],
Minordi et al.
have shown that both CT-enterography (performed after oral administration of a solution containing polyethylene glycol) and CT-enteroclysis can provide a complete distension (grade 3 on a 4-point qualitative scale) of the neoterminal ileum and ileocolic anastomosis in a high percentage of patients (92.3% and 80.9%,
respectively),
and no significant difference (p= 0,1502) has been demonstrated between these two CT techniques.
More recently,
Soyer et al.
used CT-enterocylsis to characterize the status of the ileocolic anastomosis in a cohort of 40 CD patients,
finding that it provides an adequate distension and visualization of the anastomotic site in all cases [10].
They demonstrated that severe anastomotic stenosis and anastomotic wall thickening >3 mm are the two most sensitive CT-enteroclysis findings for the diagnosis of abnormal anastomosis (including inflammatory recurrence and fibrostenosis),
with sensitivities of 97% and 93%,
respectively,
while stratification had a specificity of 100%.
In a previous work [13],
we retrospectively assessed the value of CTe-WE (i.e.
CT-enterography performed after the additional trans-rectal administration of a water enema) for a comprehensive phenotypical characterization (i.e.
CD location and behavior according to the Montreal classification [3]) of 221 CD patients.
In the CTe-WE technique the reflux of water from the cecum through the ileocecal valve into the terminal ileum combines with the orally ingested contrast material,
resulting in excellent luminal distension of both sides of the ileocecal area [16].
In the present study,
CTe-WE has shown the ability to provide a constantly adequate distension of the colonic side of the ileocolic anastomoses (90.2% of patients with a distension score ≥2),
while the lower percentage of patients with a distension score ≥2 of the preterminal ileum (74.5%) may be due to the high prevalence of stricturing recurrences (29.27%).
Another advantage of CTe-WE over the other CT techniques dedicated to the study of the bowel (i.e.
CT-enterography and -enteroclysis) is the simultaneous distension of both small and large intestine,
which can be precious to verify the presence of inflammatory lesions in CD patients throughout the whole gastrointestinal tract [13,
16].
In our study an unexpected high prevalence of SILs was demonstrated (11/41,
26.8%),
including 2 colonic SILs that might have been missed by standard CT-enterography.
In their study cohort of 34 CD patients Minordi et al.
found only one (2.94%) case of an isolated jejunal SIL (without concomitant anastomotic recurrence) and three patients (8.82%) with anastomotic recurrence associated to SILs in the proximal ileum.
Soyer et al.
[10] did not report the prevalence of SILs in their study group of 40 patients,
as they mainly focused on the CT-enterography findings that allow to differentiate between inflammatory CD recurrence and anastomotic fibrostenosis.
CT has the added value of enabling the examination of the entire bowel wall as well as extra-luminal involvement,
which are two well-known limitations of endoscopy [10-13].
In our study,
CTe-WE detected 4/41 (9.75%) penetrating anastomotic recurrences (Figure 7) and 3/11 (27.3%) penetrating SILs (excluding perianal disease),
that might have been missed by conventional endoscopic studies.
In the work of Minordi et al.
[11] CT-enterography and CT-enteroclysis have shown high values of sensitivity,
specificity and accuracy in the assessment of CD anastomotic recurrence (96.9%,
100% and 97%,
respectively),
with only one false-negative CT case and no false-positive cases,
using ileocolonoscopy as reference standard.
In our work we found two false-positive and two false negative cases,
which all had an endoscopic correlation.
The false-negative cases were both related to anastomotic recurrence manifesting with only small aphthous lesions (i.e.
less than 5,
Rutgeerts score = 1),
and it is known that CT-enterography may fail in the detection of these tiny mucosal ulcerations due to insufficient spatial resolution (i.e.
inferior to that of conventional barium studies [17]).
On the other hand false-positive cases were both determined by a slight mucosal hyper-enhancement,
which may reflect hyperemia and edema of the anastomotic site,
without mucosal ulcerations (Rutgeerts score = 0).
Recent studies have shown that recurrence rates are similar whether end-to-end anastomosis or side-to-side anastomosis is performed [5].
Nevertheless,
with regard to the behavior of CD recurrence,
we found that end-to-end and end-to-side ileocolic anastomoses are significantly more prone to stricture than wide-lumen stapled side-to-side ileocolic anastomoses (p= 0.032).
This result,
despite the low number of patients of our study cohort,
is supported by other Authors [6],
who suggest that the stapled side-to-side technique may reduce the risk of obstruction because of a wider anastomotic lumen.
The major drawback of our study relies on its retrospective design (i.e.
systematic search in our institutional radiology database),
which may have led to inclusion of patients only when anastomotic recurrence was clinically suspected.
This method of inclusion resulted in a relatively high prevalence of abnormal anastomoses (41/51 [80.4%]),
and it might have conditioned the overall diagnostic performance of CTe-WE in the detection of CD anastomotic recurrence.
A disadvantage of CTE is the radiation exposure,
particularly in the setting of a chronic and remitting disease such as Crohn’s,
which can lead to multiple CT examinations in young patients.
Despite the development of new techniques of dose reduction and optimization is overcoming this problem,
several authors advocate the use of MR-enterography/ -enteroclysis in particular in younger CD patients [18-20].
However,
a disadvantage of MRI in the assessment of ileocolic anastomoses is that surgical clips may impair the diagnostic capabilities of this imaging modality in about 10% of cases,
due to the presence of metal artifacts [10,
12].
On the other hand,
CT is not limited by the presence of surgical clips in correspondence to the anastomotic site,
is a less expensive and more available technique and requires shorter examination times.
In conclusion,
the value of CTe-WE in the assessment of CD patients who have undergone ileocolic resection relies on its ability to provide a good distension of both sides of the ileocolic anastomosis and to detect SILs throughout the remaining gastrointestinal tract including small bowel segments which are not accessible by conventional endoscopic techniques.