51 patients were included (26 [51%] male and 25 [49%] female; mean age: 52.88 years ± 13.35; age range: 32–79 years).
The mean CD duration in our study cohort was 11.6 ± 6.2 years,
with a mean time interval between age of symptom onset and ileocolic resection of 7.2 ± 4.5 years.
Ileocolic anastomoses were as follows: 18 (35.3%) stapled side-to-side,
17 (33.3%) end-to-side (7 stapled and 10 hand-sewn),
and 16 (31.4%) end-to-end (6 stapled and 10 hand-sewn).
The clinical indication for the CTe-WE was suspected CD anastomotic recurrence with clinical symptoms in 45 patients,
and suspected CD anastomotic recurrence without clinical symptoms in the remaining 6 patients.
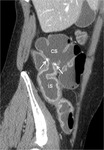
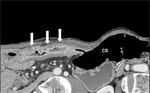
The degree of distension of the ileal side of the ileocolic anastomosis received a score ≥2 (on a qualitative 3-point scale) in 38/51 (74.5%) patients,
while the colonic side received a score ≥2 in 46/51 (90.2%) patients (Figure 1).
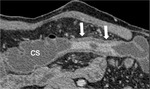
CTe-WE findings of CD anastomotic recurrence were detected by the two readers in 43 examinations,
which included, according to the reference standard,
41 true positive cases and 2 false positive cases (Figure 2).
The ileal side of the anastomoses was involved in all cases of anastomotic recurrence.
The remaining 8 CTe-WE examinations included 6 true negatives and 2 false negatives.
With regard to the true positive examinations,
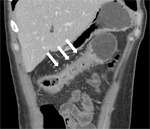
isolated anastomotic recurrence (without SILs) was found in the majority of cases (30/41 patients [73.2%]); anastomotic recurrence with a SIL in 11/41 patients (26.8%) (Figure 3).
There were no patients with multiple SILs.
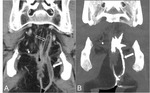
CTe-WE demonstrated a CD recurrence not involving the anastomotic site in only 2/51 patients (3.92%),
including one inflammatory ileal recurrence,
and one case of perianal fistulizing CD (Figure 4).
In both patients colonoscopy was negative for anastomotic recurrence,
but CRP values were increased.
These two cases were not classified as “SILs” due to the absence of a concomitant anastomotic recurrence.
The chi-square test did not demonstrate a significant association between the type of ileocolic anastomosis and the behavior of CD recurrence (p= 0,2725).
Nevertheless,
dividing the study cohort in two groups (group A including stapled side-to-side anastomoses and group B including both end-to-side and end-to-end ileocolic anastomoses),
the Fisher's exact test revealed a significant lower prevalence of stricturing recurrence in the group A (p= 0.032769) (Figure 5).
The prevalence of both inflammatory (p= 0.176130) and penetrating (p= 0.595635) recurrences was not significantly different between group A and group B.