SKULL BASE PATHOLOGY
Different entities which affect the skull base include congenital pathology,
traumas,
infections,
inflammation and tumours.
In the followings,
we present some examples of skull base pathology:
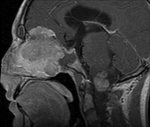
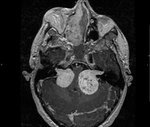
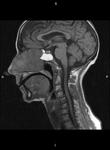
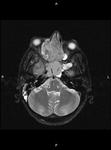
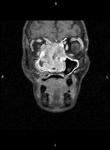
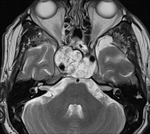
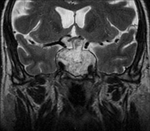
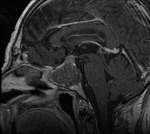
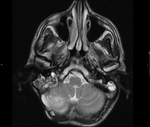
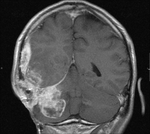
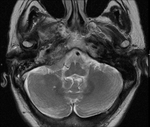
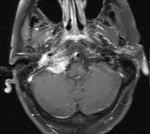
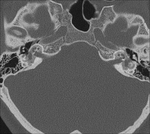
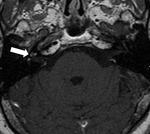
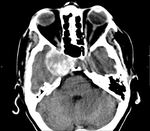
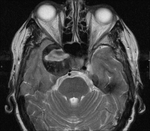
Clinical case – Meningioma of the olfactory sinus (Fig. 3 and Fig. 4), neurinomas in both internal auditory conducts (Fig. 4) and bulbar astrocytoma (Fig. 3) in a young woman with type II neurofibromatosis.
Meningioma – the most frequent intracranial extraaxial tumour,
predominantly supratentorial,
the peak age prevalence is between 35 and 65 years and it manifests a predilection for the feminine gender.
There are demonstrated correlations with type II neurofibromatosis and with basal cells nevus syndrome.
Usually it manifests by headache and seizures.
If it’s situated in the greater wings of the sphenoid,
they have a tendency of enclose the carotid artery and the middle cerebral and to compress the optic nerve and the chiasm.
CT – hyperostosis; calcifications; dural tail; erosions, mimicking schwannomas; contrast-enhancement.
MR – T1 sequences are not very sensible (relaxation time similar to the cerebral tissue); in T2 it is iso- or hyperintense; presents homogeneous contrast enhancement.
Neurinoma (schwannoma) – the most affected cranial nerve is the VIII; the main symptoms there are hearing loss and tinnitus; expansion and asymmetry of the auditory canal,
occupation of the pontocerebellar angle.
MR is the technique of choice,
they are hypointense in T1 and hyperintense in T2; they present contrast-enhancement,
they have well defined borders,
sometimes they show quistic parts,
necrosis,
and haemorrhage.
They are bilateral in neurofibromatosis.
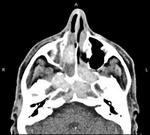
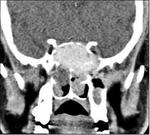
Clinical case – Infiltrative mass in nasopharynx (Fig. 5 and Fig. 6).
Nasopharyngeal carcinomas with skull base extensions usually have invasion of the clivus,
the sphenoid sinus,
the cavernous sinus,
the pterygopalatine fossa,
the pterygoid canal,
and the foramen rotundum.
They can manifest by persistent middle otitis secondary to the compromise of the Eustaquio tube.
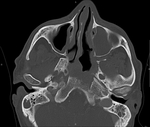
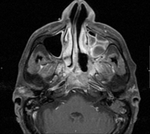
Clinical case – Squamous cell carcinoma of the ethmoid sinuses (Fig. 7, Fig. 8 and Fig. 9).
The carcinomas of the paranasal sinuses are not frequent processes.
The main histological type is the squamous one and when it affects the ethmoid sinus it can also invade the orbit and the anterior cranial fossa.
The sagittal and coronal sections are especially useful to appreciate the extension.
Clinical case – Clivus chordoma (Fig. 10, Fig. 11 and Fig. 12).
The skull base chordomas occurs at younger ages (medium 20-40 years) than in the sacrum (40-60 years,
the most frequent location).
Habitually in the clivus and the sphenooccipital synchondrosis,
they frequently present invasion of the nasopharynx,
the nasal cavities,
the maxillary sinuses and the petrous apex. CT – osseous destruction,
calcifications.
MR – isointense in T1,
hyperintense in T2.
Clinical case – Right occipital osteosarcoma (Fig. 13 and Fig. 14).
Generally,
the osteosarcoma is a osteolytic tumour which affects firstly the metaphysic parts of the extremities,
with two peak ages of prevalence: one in the 2nd - 3rd decades of life and the other in the 7th decade.
Rarely does it affect the skull base.
Clinical case – Jugular glomus (Fig. 15 and Fig. 16).
The paraganglioma (glomus,
quemodectoma) is a well vascularized tumour with a locally aggressive growth.
The jugular type originates in the internal jugular vein and affects the IX,
X,
XI cranial nerves (at the level of jugular foramen) and the VII nerve (by extension).
The tympanic type growths from the Jacobson nerve,
in the mesotympanum and manifests by tinnitus and hypoacusia.
CT – contrast enhancing mass with bone erosions.
MR – heterogeneous aspect with lineal or punctiform signal voids ("pepper").
Clinical case – Mycotic sinusitis (Fig. 17 and Fig. 18).
It is classified in invasive and noninvasive and in acute or chronic.
Mucormicosis and aspergillosis are particularly aggressive occurring usually in immunocompromised patients.
They are associated to bone lesions,
contrast enhancement and high tendency of intracranial spread.
Clinical case – Otosclerosis (Fig. 19).
The typical patient is a young woman with bilateral hypoacusia and tinnitus.
CT – otic bone resorption and,
in advanced cases,
osseous neoformation and sclerosis which alters the transmission of sound through the ossicular chain to the oval window.
Clinical Case – Labyrinthitis (Fig. 20).
Usually it is a viral infectious process.
It can be noted a decrease of the signal of the endolymph in T2 sequences and enhancement in T1.
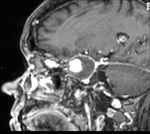
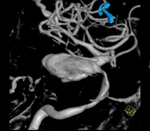
Clinical case – Internal carotid aneurysm (Fig. 21,
Fig. 22,
Fig. 23,
and Fig. 24).
The aneurysms of the intracranial segments of the ICA can manifest by headache,
compression of the closed structures or rupture and bleeding.
It can associate well defined bone resorption and curvilinear calcifications.