The abdominal aorta aneurysms (AAA) has a prevalence of 4-7% in the population between 65 and 80 years old.
A ruptured AAA,
is the cause of death of 15,000 people /year worldwide.
Many patients die before reaching the hospital and postoperative mortality after rupture is 50 to 60%.
An abdominal aorta aneurysm is defined as the dilation greater than 3cm in diameter,
although it poses no risk of rupture until it reaches 5.5 cm in men and 5 cm in women.
Screening and monitoring:
The latest recommendations from the American prevention department (USPSTF) support the evaluation with at least one screening ultrasound for diagnosis of AAA in men,
when they are between 65 and 75 years old,
when they have smoked more than 100 cigarettes in their lifetime.
In Europe there are no proven and established generalized recommendations.
The AAA is often diagnosed incidentally during an imaging study indicated for another reason.
It is important to know the risk associated with AAA in patients with aneurysms in other locations,
a 62% of patients with popliteal aneurysms and 85% of those with femoral aneurysms have an AAA,
and so abdominal aorta should be evaluated in these patients.
An ultrasound monitoring protocol,
for asymptomatic abdominal aorta aneurysms of less than 4.5 cm,
are shown in Table 1.
While imaging follow up is necessary,
the patient should be referred for evaluation by a physician with expertise in vascular disease,
as there are general recommendations and medical treatment (eg.
Beta-blockers,
smoking cessation,
etc.) that could reduce morbidity and mortality associated with this diagnosis.
Alarm signs:
Signs that involve increased risk can be divided into clinical and radiological:
The presence of abdominal pain,
without other explanation than pain associated with abdominal aneurysm,
increases mean patient morbidity from 5% to 26%.
At follow-up imaging,
there are some signs that indicate an increased risk of rupture that we should consider,
and may derive in an earlier or urgent specialist consultation,
even with diameters of less than the threshold of 5.5 cm or 5cm.
Signs that carries high risk of rupture:
1.
- Rapid growth,
an increase of 6-12 mm per year,
has been shown to pose a high risk of rupture.
2.
- Saccular or very eccentric morphology of the aneurysm,
being more risky the latter.
3.
- The absence of thrombus or thinning,
are also associated with increased likelihood of rupture.
4.
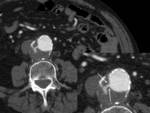
- The wall ulceration or new onset ulceration of a mural thrombus.
Fig. 1
5.
- The focal or diffuse thickening of the aortic wall,
fibrotic periaortic changes,
fat stranding or the existence of a focal saccular aneurysm should raise the suspiction of an mycotic (inflammatory) etiology,
which is an important factor when deciding on the type and urgency of treatment.
Signs that require urgent specialized Evaluation:
Because these signs,
have a low positive predictive value,
urgent specialized evaluation should be recommended,
as they may require early treatment.
1.
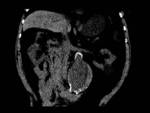
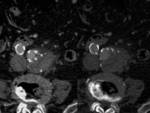
- Identification of a hyperdense crescent image in the aortic wall,
(homogeneous or layered) translates the existence of an acute wall hematoma.
It is most obvious in the baseline study without contrast and is the sign with greater specificity.
Fig. 2
2.
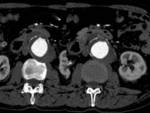
- The "draped aorta sign" which refers to the lining of a vertebral body by the dilated and deformed aortic wall,
in the appropriate clinical context; this may be the only evidence of rupture.
Fig. 3
3.
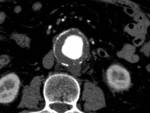
- Parietal calcium Discontinuity: can be identified in a obvious aortic rupture or could be present as the only high risk sign in an aneurysms showing no other apparent complications.
Fig. 4
4.
– Aortic wall blurring,
given by slight diffuse or focal increases of the peri-aortic fat density.
Fig. 5
Signs of rupture:
Are easy to identify in most cases,
and the presence of any of these signs and an AAA,
should be reported as AAA rupture,
in presence or even in absence of signs of acute contrast leakage:
1.
- The presence of a retroperitoneal hematoma.
2.
- Hematoma at the root of the mesentery.
3.
- Collection of blood in the psoas muscle,
without a cleavage plane with the aneurysm sac.
Treatment planning:
The treatment of AAA,
can be performed with surgical or endovascular techniques,
the latter began to be suitable for high-risk surgical patients but,
over time their indications include a larger group of patients.
The following aspects about the aneurysm should be registered:
1.
- Aneurysm angulations,
with respect to the longitudinal axis of the aorta.
2.
- The neck of the aneurysm: is defined as the segment between the most distal visceral vessel cranial (proximal) to the aneurysm and the beginning of the pathologic aortic segment:
2a.
- Diameter: the diameter should be obtained including wall and measured perpendicular to the aorta.
If in doubt,
should be overestimated or report the greatest measure obtained.
Measures greater than 32mm are complicated to treat with endoprothesis. Fig. 6
2b.
- Length: usually defined by the renal arteries,
must be greater than 12-15mm.
If it is difficult to establish,
always report the shortest measure.
A curved MPR is the best method to evaluate it.
Fig. 7
2c.
- There must have no thrombus / atheroma: if it is circumferential or greater than 2mm thick,
must be referred.
3.
- The aneurysm sac:
3a.
- Diameter: measured on a plane orthogonal to the axis of the aorta,
estimates the risk of breakage.
The aneurysm endoluminal narrower diameter should be reported.
3b.
- Length: From the beginning of the aortic aneurysm,
until the point where it recovers normal diameter and morphology,
or to the aortic bifurcation.
Best if it is done over a curved MPR.
3c.
- Distal diameter: Before the iliac bifurcation,
the aortic diameter should be measured,
which will reveal the possibility of treatment using unilateral or bilateral iliac extensions.
We recommend a diameter of at least 20mm for bilateral (bi-iliac endoprothesis).
4.
- The iliac: primitive,
external and internal:
4a.
- Length: to plan extensions,
should be at least 30mm.
recommending the use of a curved MPR.
4b.
- General diameters,
focal stenosis or calcification: should be referred.
4c.
- Intrinsic and relative tortuosity to the aneurysm sac: this assessment is often subjective,
but important.
4d.
- Hypogastric patency.
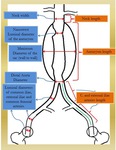
In Fig. 8,
a graphically detailed scheme is shown,
with the different measures,
needed to plan treatment.
The diameters should be obtained on perpendicular planes to the major axes of the vessel,
and the lengths should be taken over curved MPR lumen centered.
Fig. 9
Important anatomic variants:
1.
- The retroaortic or circunaortic disposition of the left renal vein,
which complicates surgery.
2.
- The existence of polar renal arteries: number and size or dominance.
3.
- Assess for significant stenotic disease (atherosclerotic or dysplastic),
superior mesenteric,
celiac trunk and the presence of collateral,
which will supply the territory of the inferior mesenteric artery,
because in the most of the cases,
treatment blocks its origin.