Our four cases occurred in men,
average age 62.75 years (range = 54-77).
50% were referred to the Unit of tumours diagnosed of sarcoma,
one case went to the traumatolgy service and the remaining to the emergency room.
There was history of severe traumatic injury in the lower limb in all cases,
average of 24 years ago (range 12-34).
The 50% clearly explained a compartment syndrome,
and the rest reported repeated hematomas.
75% suffered a residual equinus foot.
75% were located in the anterior compartment and one in the posterior.
All associated extensive calcification of the interosseous membrane.
The three cases of anterior compartment,
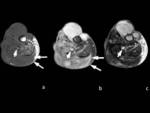
broadly contacted with tibial cortical bone causing remodelling, thick sclerotic periosteal reaction and ill-defined foci of erosion.
In the four cases,
the morphology of the tumour was fusiform and following the path of a muscle or muscle group which was replaced by the mass.
The presences of laminar peripheral calcifications circling the mass were a constant finding.
The 50% associated gross irregular central calcifications.
In the two cases where contrast was administered no significant enhancement was observed.
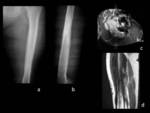
MRI,
performed in three of the four cases,
allowed a better characterization of intralesional necrohaemorragic component but a worse definition of the calcification.
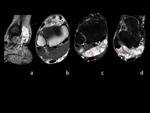
The lesions alterned regions of characteristic iso-hyperintensity in T1 that translated haemorrhage; T2 hyperintensity in relation with cystic and necrotic component; and hypointense variable zones on both T1 and T2 corresponding to the calcifications.
An almost continuous peripheral hypointense halo corresponded to laminar peripheral calcifications characterized in the Rx and CT.
One case showed tibial one marrow oedema and all showed little surrounding soft tissue oedema.
75% of the cases were treated surgically.
The remaining case underwent control evolution and surgery was required on a second time.
In 50% of cases chronic complications persisted as infection and fistulas.
Histological confirmation was available in the 4 cases.
Over 70% of cases reported in the literature,
are men,
fact which may be explained by the higher rate of accidents in this group.
The history of trauma is constant.
The latency between the trauma and the onset of this condition varies widely (from 10years the earliest to 64 the latest).
The main clinical presentation is the appearance of a large slowly growing mass.
The second most common scenario is an infectious pyomyositis.
More than 90% of cases are described to occur in the leg.
Over 60% of cases are exclusively located in the anterior compartment.
The second location is affecting both the anterior and lateral compartments; followed in frequency by the single affectation of lateral or posterior compartment.
Isolated cases of extension at the foot and thigh and location in the forearm have been described.
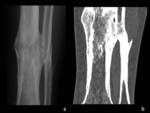
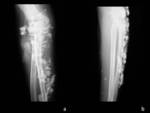
The Rx shows a soft tissue mass with predominantly peripheral linear calcifications in 100% of the reported cases.
Usually associate coarse calcifications and radiolucent areas within the lesion.
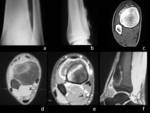
CT shows in almost all the cases,
a fusiform mass occupying and replacing much of a muscular compartment.
The tumour is limited and surrounded by laminar shaped calcifications.
Usually irregular,
amorphous,
central calcifications are associated.
Erosions,
remodeling and reactive periosteal reaction is found in over 60% of reported cases.
Few authors explicitly talk about extensive calcification of the interosseous membrane,
but it seems to be a very frequently associated aspect.
On MRI it characteristically presents as a large mass well defined by the hypointense halo corresponding to peripheral calcifications.
It presents a heterogeneous triple signal internal structure due to hemorrhagic and necrotic component.
Amorphous core calcifications can also be seen as hypointensities on both T1 and T2.
Anyway,
the calcifications are much better depicted with Rx and CT.
Bone oedema was detected in less than 10% of case.
Soft tissues oedema is frequent and due to the compressive effect of the lesion.
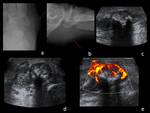
There are few explicit statements about the contrast enhancement behaviour of this pseudotumoral; but the existing ones agree that it does not enhance.
One case reports evidence of blood flow through branches of the posterior tibial artery and clear enhancement of the tumour.
Over 85% of authors recommend expectant attitude in the absence of symptoms.
The biopsy is contraindicated and the surgical treatment may only be considered in case of medically untreatable complication.
That is because of the well documented risk of torpid evolution with chronic fistulous infection as the main protagonist.
Our results are broadly consistent with those obtained from the literature.
The malignant image differential diagnosis should include those sarcomas with a tendency to affect the lower extremities,
with calcifications and juxtacortical location (Fig. 13).
The most common would be: synovial sarcoma,
malignant fibrous histiocytoma (or undifferentiated pleomorphic sarcoma),
juxtacortical (Fig. 14) and soft tissue osteosarcomas and soft tissue chondrosarcoma (Fig. 15).
Benign entities to consider in the imaging differential,
would be myositis ossificans (Fig. 16),
chronic osteomyelitis (Fig. 17) with soft-tissue abscess,
tumoural calcinosis,
fat necrosis,
soft tissue chondroma,
metastatic calcification of renal insufficiency,
myonecrosis phenomena with dystrophic calcifications in context of diabetes and vascular disease,
myositis,
dermatomyositis and scleroderma (Fig. 18).
The deeply hypointensity on the MRI could remind the aspect of collagen-rich entities as desmoid tumour (Fig. 19).
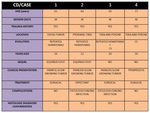
The main differential diagnoses are comparatively evaluated in Table 4 and Table 5.