Ankylosing spondylitis
Sacroiliitis is the earliest alteration,
followed by the involvement of the dorsal-lumbar spine. The involvement of the cervical spine is almost always late,
and it can occur even 20 years or more after the disease’s onset.
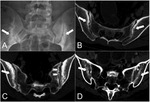
Sacroiliitis affects both the synovial (antero-inferior) and the ligamentous (postero-superior) aspects of the joint,
presenting,
in most cases,
a bilateral and symmetric distribution.
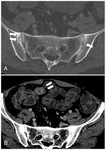
In the early stages alterations are represented by juxta-articular osteoporosis,
superficial erosions and progressive subchondral osteosclerosis,
which is first focal,
then more and more extended (Fig.
1A,
B).
The erosions tend to appear in the synovial portion of the joint on the iliac side,
where the cartilage is thinner,
but they are often masked by reactive subchondral osteosclerosis (Fig.
1C).
As the disease progresses,
erosions become more numerous and tend to coalescence,
thus resulting in a diffuse bone resorption which creates the illusion of an expansion of the joint space.
Subchondral osteosclerosis reduces in the following stages,
which are characterized by an increase in the fatty content of cancellous bone (post-inflammatory fatty conversion of bone marrow).
The osteo-proliferative stage is characterized by the development of irregular bony bridges that cross the joint space,
reducing its width until complete ankylosis (Fig.
1D).
The remnants of the joint space are sometimes visible as a thin sclerotic line on plain-film radiographs,
which appears hyperdense on CT images.
Conventional radiography does not allow an early diagnosis,
but it still represents the most frequently requested radiological investigation to confirm the clinical suspicion of ankylosing spondylitis.
The modified New York criteria,
proposed in 1984,
still represent a largely diffuse radiographic scoring system,
and they have also been applied to CT (Fig.1). CT also represents the "reference standard" for detection of osteoproductive alterations.
MRI is the only imaging modality that may provide an early diagnosis,
showing bone marrow oedema,
which appears hypointense on T1-weighted images and hyperintense on fluid-sensitive ones (STIR or T2-weighted images with fat signal suppression).
The spinal involvement,
which may be earlier,
contemporary or subsequent to the onset of sacroiliitis,
occurs with a greater frequency at disco-vertebral junctions and in correspondence to interapophyseal and costo-vertebral joints.
It includes enthesitis with bone erosion,
post-inflammatory fatty conversion of red bone marrow,
osteosclerosis and osteoproliferation with ectopic bone formation.
The enthesitis of the disco-vertebral junction,
which occurs in correspondence to the anterior and posterior corners of vertebral bodies,
is associated with erosions,
resulting in the typical "lesions of Romanus".
Osteosclerotic foci develop in correspondence to corner erosions ("shiny corners"); they progressively become larger,
causing the "squaring" of the endplates of vertebral bodies,
with loss of the normal concavity of the anterior vertebral wall (“square” vertebra or "squaring" ).
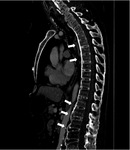
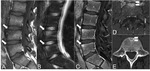
"Shiny corners" are the expression of osteitis and appear hypointense on T1-weighted MR images and hyperintense on T2-weighted images.
As the disease progresses the "shiny corners" become hyperintense on T1-weighted images due to the post-inflammatory fatty degeneration of bone marrow (Fig.
2).
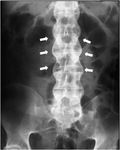
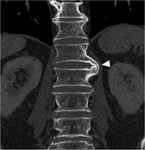
The chronic inflammation at the discovertebral junction determines the onset of an osteo-proliferative process with formation of syndesmophytes (Fig.
3),
which differ from osteophytes for their vertical course and the absence of associated disc degeneration.
In advanced stages the ossification of vertebral (longitudinal,
supra- and interspinous) ligaments may occur,
leading to ankylosis .
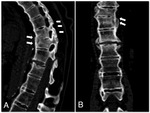
The presence of symmetric syndesmophytes along the whole spine (cervical spine is the last rachidian region to be involved) leads to the characteristic "bamboo" spine appearance (Fig.
4).
An extensive inflammatory involvement of the intersomatic disc and adjacent vertebral endplates may occur,
the so-called Andersson spondylodiscitis,
wich,
on MRI examination,
is characterized by a diffuse hypointense signal on T1-weighted images involving the intersomatic disc and adjacent vertebral endplates.
It appears hyperintense on fluid-sensitive sequences and shows significant enhancement after intravenous administration of Gadolinium-based contrast agents.
Interapophyseal joints are not preserved and erosions,
sclerosis and progressive ankylosis may develop at this level with formation of a continuous bonny pillar due to the fusion of the articular processes of adjacent upper and lower vertebrae.
Although ectopic bone formation is a typical finding of ankylosing spondylitis,
this pathological condition is also characterized by diffuse osteoporosis and low mineral density of bone,
with an increased risk of vertebral fractures (Fig.
5).
Psoriatic spondyloarthritis
The spondylitis-like form of Psoriatic arthritis is characterized by sacroiliitis associated with spondylitis.
The main features related to the axial involvement are: a) syndesmophytes that differ from those of ankylosing spondylitis (the so-called "non-marginal bulky syndesmophytes " or “para-syndesmophytes”); b) involvement of the sacroiliac joints,
which may be bilateral and symmetrical,
or unilateral (Fig.
6); c) sparing or modest involvement of interapophyseal joints.
Syndesmophytes of psoriatic spondyloarthritis are more frequent in the thoraco-lumbar spine and appear as radiopaque elements that are roughly linear or curvilinear,
thick,
fluffy and parallel to the lateral surface of vertebral bodies and intersomatic discs.
They can also tend to coalescence,
appearing as a massive osteophytic bone bridge joining two or more contiguous vertebrae,
but they rarely lead to the "bamboo" spine,
and remain isolated and asymmetric.
Unilateral asymmetric distribution and separation from the lateral aspect of the vertebral bodies are the main radiological features which allow to distinguish psoriatic syndesmophytes from those of ankylosing spondylitis and spondylitis associated with inflammatory bowel diseases.
The main radiological findings of psoriatic sacroiliitis,
which may also occur in the absence of spondylitis are: erosions,
which are more frequent on the iliac portion of the joint,
osteosclerosis,
joint space narrowing,
and,
rarely,
ankylosis.
Interapophyseal joints of the cervical spine are frequently involved (in opposition to what happens in the thoracolumbar spine),
and they may eventually become ankylotic,
while anterior atlo-axial subluxation is much more rare.
Reactive spondyloarthritis (Reiter's syndrome)
The eponym Reiter's syndrome indicates a clinical syndrome characterized by conjunctivitis, urethritis or gastroenteritis,
followed by the onset of aseptic arthritis after an interval of 1-4 weeks.
The term reactive arthritis is related to the pathogenetic theory of this SpA in which an infection of the conjunctival,
intestinal or urethral-genital mucosa may represents the trigger for a systemic autoimmune reaction which determines an aseptic inflammatory process involving the axial skeleton or appendicular joints.
The involvement of the appendicular skeleton is typically represented by asymmetrical oligoarthritis,
often unilateral,
which shows a predilection for the large synovial joints of the lower limbs.
The involvement of the sacroiliac joints is frequent and has the same radiological features of psoriatic sacroiliitis.
Also the spinal involvement,
although rare,
has features similar to those of psoriatic SpA.
In fact,
a typical early finding is represented by coarse syndesmophytes,
which are not distinguishable from those of psoriasis and are located most frequently in correspondence to the lower three thoracic and the upper three lumbar vertebrae.
The involvement of the interapophyseal joints is associated to erosions,
osteosclerosis and ankylosis,
but these findings are less frequent than those observed in ankylosing spondylitis.
Enteropathic Spondyloarthritis (Enteroarthritis)
Enteropathic SpA are related to ulcerative colitis and Crohn's disease,
of which are considered extraintestinal manifestations.
Two types of arthritis have been described: the peripheral and the axial one.
The peripheral arthritis is oligoarticular,
asymmetrical,
often transient and migratory; both large and small joints can be affected,
most frequently in the lower limbs.
With regard to the axial arthritis,
the incidence of sacroiliitis varies from 10% to 20%,
while that of spondylitis from 7% to 12%.
It should be remembered that these values may underestimate the real incidence of the axial inflammatory involvement,
which may have a subclinical course that eludes diagnosis,
being masked by symptoms of bowel inflammation (Fig.
7).
Radiological features of both spondylitis and sacroiliitis are closely similar to those of primitive ankylosing spondylitis.
SAPHO Syndrome
The acronym SAPHO was used to indicate the clinical association of synovitis,
acne,
pustulosis,
hyperostosis and osteitis.
According to the more widely accepted pathogenetic hypotheses,
SAPHO syndrome has been considered a “reactive osteitis”,
which represents the consequence,
in genetically predisposed individuals,
of a nonspecific immune response,
triggered by an infection.
The bone involvement concerns mainly the sterno-costo-clavicular region,
the spine,
and sacroiliac joints.
In the early phase osteitis appears as focal osteosclerosis associated to erosive changes of the bone cortex and edematous thickening of the adjacent soft tissues.
Subsequently,
hyperostosis (diffuse osteosclerosis with increased bone volume) and synovitis may develop.
The latter can be primary or secondary to the intra-articular extension of an adjacent osteitis.
Synovitis appears more frequently in the sacroiliac joints,
where the involvement is often unilateral,
and in the sterno-cost-clavicular joints.
It has been demonstrated a prevalent involvement of the anterior vertebral corners of the thoraco-lumbar spine (Fig.
8).