Clinical features
The clinical features in all patients consist of macrocephaly occurring commonly,
in the first year of life with a delayed onset of relatively mild neurologic abnormalities,
consisting of cerebellar ataxia,
pyramidal tract signs and seizures.
Cognitive deterioration becomes apparent over the years,
but communication and social skills remain relatively unaffected.
All patients were born at term without a significant antenatal and prenatal history.
Their parents were consanguineous and they had no specific family history.
Cytogenetic study
The cytogenetic study in a brother and sister,
from one family,
showed a mutation heterozygous type c.136delT.
MRI and spectroscopy
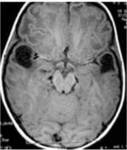
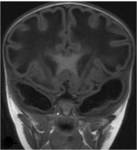
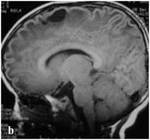
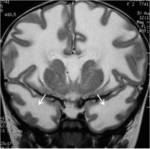
The MRI features were strikingly abnormal with diffuse involvement of the cerebral white matter.
On T1 weighted images,
the involved white matter was hypointense and had a characteristic swollen appearance (fig.1,
2,
3).
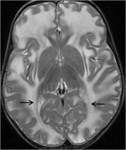
The peripheral and periventricular white matter were equally involved with sparing of some central white matter structures like the corpus callosum,
anterior limb of the internal capsule and bilateral posterior occipital radiations (fig.
4).
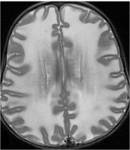
On proton-density,
T2 and FLAIR sequences,
the involved white matter was hyperintense (fig.5,
6,
7).
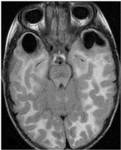
Large,
well-defined,
oval cystic lesions,
which followed cerebrospinal fluid intensity on all sequences,
were seen symmetrically in subcortical locations of bitemporal and bifrontal poles.
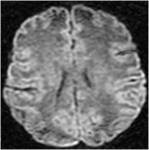
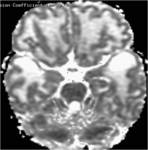
Diffusion tensor imaging showed an increased apparent diffusion coefficient in affected white matter (fig.8,
9).
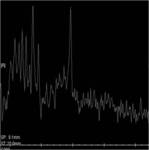
MR spectroscopy of white matter revealed reduction of N- acetylaspartate and creatinine with increased values for myoinisitol (fig.10).
DISCUSSION
Megalencephalic leukoencephalopathy with subcortical cysts (MLC) was first described by van der Knaap et al,
in 1995.
MLC is an autosomal recessive disorder due to mutations in MLC1 gene.
In many reported cases the parents were related.
At birth,
infants with classic MLC are healthy.
Macrocephaly has been identified in all reported cases to date.
Macrocephaly usually develops within the first year of life,
but is present at birth in exceptional cases.
The main presenting features after macrocephaly are pyramidal findings and ataxia which are age dependent.
Spasticity and ataxia usually develop by 5 years of age and are usually slowly progressive.
In all patients,
early psychomotor development is normal,
as was in our patients.
Most patients can walk independently but slow deterioration of motor function with cerebellar ataxia and spasticity usually starts in early childhood.
Autism is observed in some patients.
Mild cognitive deterioration becomes apparent over the years,
but communication and social skills remain relatively unaff ected.
Some patients develop extrapyramidal movement abnormalities with dystonia and athetosis.
Almost all children have occasional epileptic seizures,
easily controlled with drugs,
but status epilepticus can occur.
Minor head trauma can induce temporary deterioration,
most often with seizures or status epilepticus,
prolonged unconsciousness lasting days to months,
or acute motor deterioration with gradual improvement.
GENETICS
Parental consanguinity and disease in siblings suggest autosomal recessive inheritance.
The gene locus has been assigned to chromosome 22qtel and mutations in a gene renamed MLC1 have been identified as the cause.
The MLC1 gene encodes a putative membrane protein with eight predicted transmembrane domains.
This protein is considered to be important for the maintenance and/or compaction of the outermost lamellae of the myelin sheath.
More than 50 mutations MLC1 gene have been reported in the literature.
To our knowledge the c.136del T mutation has not been identified.
INVESTIGATIONS
Laboratory findings
Laboratory investigations are unrevealing.
No biochemical marker of the disease has been found in urine,
blood,
or CSF.
MRI and spectroscopy
- The MRI features were strikingly abnormal with diffuse involvement of the cerebral white matter.
On T1 weighted images,
the involved white matter was hypointense and had a characteristic swollen appearance.
On proton-density,
T2 and FLAIR sequences,
these areas were hyperintense.
The peripheral and periventricular white matter were equally involved with sparing of some central white matter structures like the corpus callosum,
anterior limb of the internal capsule and bilateral posterior occipital radiations.
Large,
well-defined,
oval cystic lesions,
which followed cerebrospinal fluid intensity on all sequences,
were seen symmetrically in subcortical locations of bitemporal and bifrontal poles.
- Diffusion tensor imaging showed an increased apparent diffusion coefficient and reduced anisotropy in affected white matter pointing to reduced cell density with an increased extracellular space.
The markedly increased ADC in the patient’s highsignal white matter indicates severe damage to its integrity,
with respect to myelination and axonal structure.
This suggests reduced cell density with increased extracellular space.
Because parallel axon bundles are the source of anisotropy in white matter,
its reduction implies a loss of myelinated axons as one of the sources of the reduced cell density expected from the increased ADC.
- MR spectroscopy of white matter revealed marked reduction of N- acetylaspartate (NAA),
creatinine (Cr),
and choline (Cho) with normal or increased values for myoinisitol (Ins),
consistent with axonal loss and astrocytic proliferation.
Quantitative proton MRS underlines the MRI evidence of a white-matter disorder without cortical involvement.
Most striking MRS features are marked decrease in NAA,
Cr,
and Cho,
with normal Ins in abnormal-appearing hemispheric white matter.
Reduction of NAA and Cr is consistent with damage to or loss of vital neuroaxonal tissue.
DIFFERENTIAL DIAGNOSIS
Differential diagnosis of MLC includes Canavan's disease,
Alexander disease,
infantile onset GM2,
GM1 gangliosidosis,
glutaric aciduria and merosin deficient congenital muscular dystrophy.
MLC characteristically has an early onset and slow progression whereas Canavan and Alexander's disease have a more rapid progression and neurological deterioration is severe so that the patients have spasticity and seizures from a young age.
Glutaric aciduria was ruled out biochemically.
Absence of muscle weakness and normal CPK ruled out congenital muscular dystrophy.
In Canavan's disease,
involvement of the globus pallidus and the thalamus is seen,
which are spared in MLC also absent in our patient.
Although cystic white matter may be seen in Canavan's disease,
the typical subcortical cyst is lacking.
Alexander's disease leads to a magalencephaly and leukoencephalopathy with frontal predominance,
sometimes hydrocephalus,
cavitation and cystic degeneration in the frontal
deep white matter and abnormal enhancement of caudate nuclei,
anterior columns of the fornices and periventricular areas.
MRI in infantile GM2 gangliosidosis shows prominent involvement of the basal ganglia and thalami in addition to the white matter abnormalities.
MRI feature in infantile GM1 gangliosidosis are very similar to those of GM2 gangliosidosis.
This disease has been successfully diagnosed prenatally.