0.
ANATOMY:
The normal gallbladder wall is composed of four layers: the mucosa,
an irregular smooth muscle layer,
a perimuscular connective tissue layer and serosa.
The mucosa forms primary and secondary folds when the gallbladder is empty and flattens as the lumen expands.
The outer perimuscular connective tissue contains large nerves, blood vessels,
lymphatics,
and occasional paraganglia. Along the hepatic surface there is no serosa, but occasional aberrant bile ducts (Luschka ducts) may be seen,
usually surrounded by fibrous tissue.
Thus,
there is continuity of the connective tissue layer of the gallbladder with the interlobular connective tissue of the liver.
The wall may contain small lobules of mucus glands (peribiliary glands) that drain into the saccule of Beale.
The muscle layer is more prominent near the cystic duct,
where it forms the valves of Heister,
and near the sphincter of Oddi in the distal common bile duct.
The subserosa contains adipose tissue,
large blood vessels,
lymphatics,
and occasional ganglion cells.
1. EMBRIOLOGIC DEVELOPMENT:1
The gallbladder,
bile ducts,
and liver begin to develop during the 4th week of embryogenesis as a ventral bud from the most caudal aspect of the foregut (the future duodenum).
This bud is called the hepatic diverticulum.
The hepatic diverticulum has two distinct components: pars hepatica and pars cystica .
The pars hepatica,
the most cranial component,
gives rise to the liver,
common hepatic duct,
and intrahepatic bile ducts.
The pars cystica,
the most caudal component,
gives rise to the cystic diverticulum.
The cystic diverticulum is the anlage of the gallbladder and the cystic duct.
The original hepatic diverticulum elongates to form the common bile duct.
2.
NORMAL APPEARANCE OF THE GALLBLADDER:2
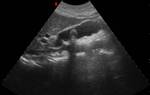
The gallbladder should be imaged after the patient has fasted for 8–12 hours,
which promotes physiologic distention of the gallbladder.
US is the primary imaging modality used specially to evaluate acute right upper quadrant pain,
as it is highly sensitive and specific for the detection of gallstones and biliary dilatation,
and will often be enough to direct treatment decisions.
But there are situations where additional imaging may be required.
In general terms,
CT is an excellent second choice.
It will frequently provide a better overview of the extent of disease where visibility with US is limited (for example in pacients with surgical dressings,
obesity...) and will complement the US findings in more complex cases.
The combination of US and magnetic resonance (MR) imaging or MR cholangiopancreatography provides excellent potential for diagnosis of acute biliary ductal disease aswell as other non-acute syndroms.
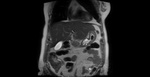
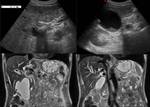
Refering to MR,
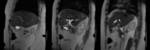
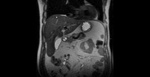
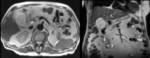
on T2-weighted images,
the gallbladder wall has low signal intensity and stands out against the bright visceral fat.
The wall adjacent to the liver cannot be identified as a separate structure.
On T1-weighted images,
the gallbladder wall has intermediate signal intensity and enhances uniformly after the administration of gadolinium-based contrast material.
The insertion of the cystic duct into the hepatic duct can be demonstrated with routine T2-weighted imaging and MR cholangiography. Normal bile appears uniformly bright with T2-weighted sequences.
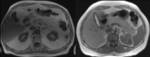
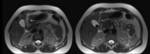
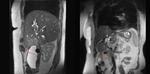
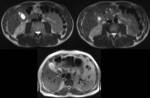
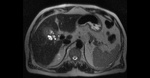
On T1-weighted images,
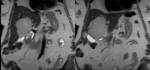
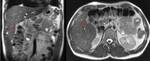
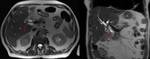
bile varies greatly in signal intensity depending on its concentration. Fig. 1 Fig. 2
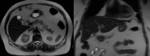
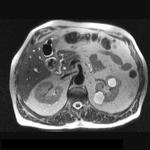
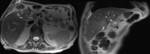
During fasting,
bile undergoes a process of concentration.
Water is reabsorbed and the concentration of cholesterol and bile salts increases,
leading to a shortened T1 relaxation time and,
consequently,
to bright bile on T1-weighted images.
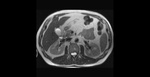
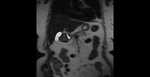
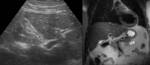
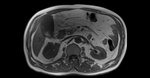
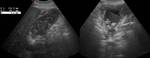
A layering effect is sometimes observed,
with concentrated and denser bile in the dependent position. Fig. 3
3.
PATHOLOGY OF THE GALLBLADDER:
3.1 Congenital abnormalities:2
There are many uncommon anomalies of the gallbladder and biliary tree that are delineated with MR cholangiography.
MR cholangiography is useful in defining the biliary anatomy for preoperative planning,
and anatomic variants.
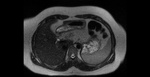
3.1.1.
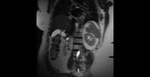
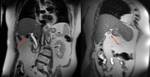
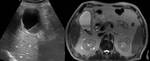
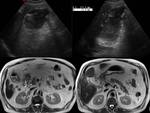
Agenesia: Gallbladder agenesis is rare.
The congenital disorder has to be taken into account if no gallbladder can be found during imaging or surgery.
Sonography is not the adequate method for diagnosing gallbladder agenesis. Fig. 4
3.1.2.
Septy: Septation of the gallbladder are developmental anomalies of the gallbladder. Multiseptate gallbladder is a very rare congenital anomaly and the patients usually present with biliary symptoms.
There may be concomitant cholelithiasis.
Fig. 5 Fig. 6
Partial or complete septation can also be seen. Fig. 7
3.1.3.
Bilobed or duplicated gallbladder: It is a congenital abnormality that is well defined at MR imaging and MR cholangiography.
This entity is rare and may be associated with right upper quadrant pain.
Classifications vary,
with distinctions sometimes being made between bilobed gallbladder and true gallbladder duplication.
Bilobed or duplicated gallbladder has been found to predispose to complications such as cholelithiasis and cholecystitis.
Delineation of the anatomy is important for preoperative planning and avoidance of biliary injury. Fig. 8
3.2 Anatomic variants:
3.2.1.
Unusual shaped gallbladder: A great variety of shapes can be found within the gallbladder,
which can sometimes can be associated with cholelithiasis or consequent complications. Fig. 9
3.2.2.
Luschka bile duct:3 The anatomy of the biliary system is highly variable,
and some of these variations and anomalies can be problematic for surgeons. Surgery carried out in ignorance of such anomalies can result in accidental injury to the patient or to inadequate ligation of these ducts.
As a result,
persistent bile leakage or segmental biliary obstruction may occur.
Operative cholangiography has been used to help avoid these complications.
In general,
the bile duct of Luschka is a thin,
short,
vestigial bile duct lying in the gallbladder bed. Fig. 10
3.3.
Benign non inflamatory entities:
3.3.1.
Schleroatrophic gallbladder:4 Also know as porcelain gallbladder.
The true incidence of it is unknown,
but it is reported to be 0.6-0.8%,
with a male-to-female ratio of 1:5.
Most porcelain gallbladders (90%) are associated with gallstones.
Sonograms do not depict porcelain gallbladder as well as CT scans do; sonographic findings can mimic those seen with a nonfunctioning gallbladder,
large calculus,
and emphysematous cholecystitis as we can see an hyperechoic semilunar structure with posterior acoustic shadowing that simulates a stone-filled gallbladder, an irregular clump of echoes with posterior acoustic shadowing or also an echogenic gallbladder wall without acoustic shadowing.
Fig. 11
In MR we can better define the small sized gallbladder,
with narrow lumen and diffuse and fibrous wall thickening. Fig. 12
3.3.2.
Poliposis:1 Cholesterol polyps of the gallbladder represent approximately one-half of all polypoid lesions in the gallbladder and have no malignant potential. At gross inspection,
cholesterol polyps appear as small,
yellow,
lobulated,
polypoid or tumorlike projections attached to the gallbladder mucosa by a pedicle.
Cholesterol polyps are single or multiple and are usually less than 10 mm in diameter.
On US images,
small cholesterol polyps appear as brightly echogenic masses or nodules attached to the gallbladder wall,
with a typically round or slightly lobulated shape and with no posterior acoustic shadowing like typical stones do.
It is often difficult to distinguish a nonshadowing adherent stone from a cholesterol polyp.
In MR they can also be seen as small wall attached tumorlike lesions. Fig. 13
3.3.3.
Focal or diffuse adenomyomatosis: There are three variants of adenomyomatous hyperplasia: localized (or fundal),
segmental,
and diffuse.
The localized variant is the most common and is also known as an adenomyoma.
This lesions are created by multiple small cystic spaces that represent prominent epithelial invaginations (Rokitansky-Aschoff sinuses or intramural diverticula).1
The segmental variant is typically located in the body of the gallbladder. Diffuse adenomyomatous hyperplasia is characterized by diffuse gallbladder wall thickening with intramural diverticula that
appear as cystic spaces within the wall.
Intramural diverticula appear sonographically as anechoic or echogenic spaces in the gallbladder wall.
Bile-containing diverticula appear anechoic,
whereas those that contain biliary sludge,
cholesterol,
or stones are echogenic.
The visualization of Rokitansky-Aschoff sinuses on T2-weighted MR images has been reported to be useful in the differentiation of adenomyomatous hyperplasia from gallbladder carcinoma. Fig. 14
3.4.
Gallbladder contents:
3.4.1.
Cholesterol or pigmented cholelithiasis:5 Women are affected more commonly than men,
with an increase with age in both sexes.
The pathogenesis of gallstones is related to supersaturation of bile constituents,
most notably cholesterol,
and likely related to defects in biliary lipid metabolism.
Diet,
a sedentary lifestyle and a genetic predisposition to stone formation can predispose to their prevalence.
Pigment stones have by definition less than 25% cholesterol,
and the major component is calcium bilirubinate.
Calcium carbonate is a less common constituent.
Ultrasonography is the method of choice for detection of gallstones.
The characteristic US findings of gallstones are a highly reflective echo from the anterior surface of the gallstone,
mobility of the gallstone on repositioning the patient,
and marked posterior acoustic shadowing.
On MR imaging sludge is seen hypointense on the T2-weighted image and hyperintense on the T1-weighted image,
aswell as gallstones,
better defined and rounded shaped.
Fig. 2
3.4.2.
Hemobilia:6 Biliary tract blood,
known as hemobilia,
is usually caused by malignant tumors such as hepatocellular carcinoma,
blunt trauma,
hemorrhagic cholecystitis, rupture of an aneurysm of the hepatic artery,
hemorrhagic diathesis or biopsy.
The MR imaging findings indicative of hemobilia are clots,
which appear as defects in the gallbladder and bile duct at MR cholangiopancreatography,
and hemorrhagic bile,
which has high signal intensity on fat-suppressed T1-weighted images and low signal intensity on heavily T2-weighted images.
A fluid-fluid level can be observed in the lumen of the gallbladder and extrahepatic bile ducts.
Dynamic contrast enhanced MR imaging may be necessary to detect
the bleeding point and to diagnose the causative malignant tumor.
Fig. 15
3.5.
Benign inflamatory diseases:
3.5.1.
Acute cholecystitis: It usually results from obstruction of the cystic duct or gallbladder neck. In most patients,
an impacted gallstone is the underlying cause.
Acalculous cholecystitis, a condition caused by adenomyomatosis, gallbladder polyp,
malignant neoplasm,
or other causes,
occurs in approximately 5%–10% of patients who have acute cholecystitis.
The symptoms caused by acute cholecystitis include right upper quadrant pain,
tenderness,
and increased fever and resemble those caused by a peptic ulcer,
acute pancreatitis,
acute hepatitis,
acute gastritis,
or acute appendicitis.6
MR imaging findings of acute uncomplicated cholecystitis include:
- Gallstones,
often impacted in the gallbladder neck or cystic duct.
- Gallbladder wall thickening (3 mm or more).
- Gallbladder wall edema.
- Gallbladder distention (hydropic gall bladder when diameters are more than 10x5 cm).
- Pericholecystic fluid.
- Perihepatic fluid.
The presence of one or more of the six criteria is indicative of acute cholecystitis. Fig. 16
An impacted gallbladder neck stone is usually depicted at MR cholangiopancreatography and heavily T2-weighted imaging as a round signal defect larger than the diameter of the cystic duct,
aswell as in fat-suppressed T2-weighted images.
A stone usually appears as a round area of low signal intensity on T1-weighted,
T2- weighted,
and steady-state coherent images.
A stone with high cholesterol content may appear as a hyperintense lesion on T1-weighted images.
It is important to differenciate from other gall bladder lesions such as polyps or tumors,
which have intermediate or high signal intensity on T2-weighted whereas stones are usually depicted as hypointense lesions.
When refering to thickened gallbladder wall it is important to mention that wall thickening can also be seen in chronic cholecystitis,
adenomyomatosis, malignant neoplasm,
and acute hepatitis.
However, a thickened wall with a diffuse or patchy distribution of increased signal intensity on fat-suppressed T2-weighted images is suggestive of an acute inflammatory process.
Extension to the adipose tissue surrounding the gall bladder aswell as increased contrast enhancement in the gallbladder wall,
pericholecystic fat,
and intrahepatic periportal tissues,
are also supportive of acute cholecystitis.4
We also have to mention cases of acalculous cholecystitis,
which accounts for 5%–10% of all cases of acute cholecystitis and occurs most commonly in patients in the intensive care unit.
Predisposing factors include trauma,
mechanical ventilation,
hyperalimentation,
the postoperative state,
diabetes mellitus,
vascular insufficiency,
prolonged fasting,
burns,
and the postpartum state.
These conditions share the propensity to produce gallbladder ischemia.
Acalculous cholecystitis carries high morbidity and mortality rates partly because of difficulty and delay in making the diagnosis.
Complications of acute cholecystitis develop in up to 40% of patients with acute cholecystitis:
- Empyema of the gallbladder: Occurs when pus fills the distended and inflamed gallbladder.
This complication typically occurs in diabetic patients. Pus within the gallbladder resembles sludge,
seen in MR heavily T2-weighted images as lower signal intensity content in the gallbladder.Fig. 17
- Gangrenous cholecystitis: Results from increased intraluminal pressure due to cystic duct obstruction, leading to marked distention of the gallbladder, ischemic necrosis of the wall,
and intramural hemorrhage or abscess.
It is more common in men,
patients of advanced age,
and those with coexisting cardiovascular disease. 2
Irregular or asymmetric thickening of the gallbladder wall is well demonstrated on MR,
either in fat-suppressed T2-weighted images,
fat-suppressed T1-weighted images,
and contrast-enhanced fat-suppressed T1-weighted images,
with other additional findings such as ulceration (shown as a concave hyperintense area on fat-suppressed T2-weighted images), intramural hemorrhage,
necrosis,
fistulas and abscess (shown as an inhomogeneous hyperintense area on fat-suppressed T2 and T1-weighted images).
When administrating an intravenous contrast agent,
we typically find an inhomogeneous wall enhancement accompanied by lack of enhancement of part of the inflamed wall,
aswell as disrupted mucosal enhancement.
Fluid collections or abscess caused by associated gallbladder perforation or an intramural abscess may also be observed. Fig. 18
- Emphysematous cholecystitis:6 It is a rare form of acute cholecystitis,
described with more frequency in patients between 50 and 70 years of age and underlying diabetes mellitus and peripheral atherosclerotic disease.
US may demonstrate characteristic intraluminal and intramural gas as highly echogenic reflectors,
which can be mistaken for biliary calculi.
Fig. 19
CT is the most sensitive and most specific imaging modality for identifying gas in the gallbladder lumen or wall,
as well as MR,
where typical finding of intraluminal gas consists of numerous floating signal void bubbles in the upper dependent portions of the gallbladder or extrahepatic bile duct,
associated to gallstones in the lower dependent portion.
These signal voids are due to the susceptibility artifact caused by the air-tissue interface,
which is more clearly seen in fat-suppressed T1 and T2-weighted and black blood T2-weighted spin-echo echo-planar images,
and helps to distinguish between intramural gas and intramural stone. Fig. 20
- Mirizzi syndrome: Obstructive complications of the bile duct have to be considered too,
and can be caused by various diseases such as impaction of a calculus,
postinflammatory or postsurgical strictures,
and malignant tumors.
The role of imaging in these cases are to determine the level and severity of the bile duct obstruction and to identify the cause of obstruction of the extrahepatic bile duct,
such as a common bile duct stone,
sclerosing cholangitis,
Mirizzi syndrome,
or malignant pancreaticobiliary neoplasm.2
Mirizzi's syndrome is a rare complication in which a gallstone becomes impacted in the cystic duct or neck of the gallbladder causing compression of the common bile duct or common hepatic duct,
resulting in obstruction and jaundice.
The obstructive jaundice can be caused by direct extrinsic compression by the stone or from fibrosis caused by chronic cholecystitis (inflammation).
A cholecystocholedochal fistula can occur. Fig. 21
3.5.2.
Chronic cholecystitis: It is almost invariably associated with gallstones.
The gallbladder appears small and contracted,
with irregular and thickened walls.
Signs and symptoms are vague and include abdominal distention,
epigastric discomfort,
and nausea.
After the administration of gadolinium-based contrast material,
the gallbladder wall enhances less intensely than in acute cholecystitis.
The enhancement is usually smooth and slow,
unlike in gallbladder carcinoma,
in which it is usually irregular and early. Fig. 22
3.5.3.
Xanthogranulomatous cholecystitis:6 Unusual form of chronic cholecystitis that may simulate malignancy radiologically and pathologically. It is predominantly seen in women between the ages of 60 and 70 years.
Patients present with signs and symptoms of cholecystitis: right upper quadrant pain,
vomiting,
leukocytosis,
and a positive Murphy sign.
Slightly less than one-half of patients have a tender,
palpable,
right upper quadrant mass at physical examination.
Complications are common (perforation,
abscess formation,
fistulous tracts...).
Althouth the mechanism is not yet clearly established,
the extravasation of bile into the gallbladder wall is believed to have a role in the development of the inflammatory process.
The gallbladder wall is thickened,
shown hiperintense in T1 sequences and the infiltrative process may extend into the adjacent soft tissues, liver,
colon,
or duodenum.
Stones are present in the majority of the patients. Fig. 23
3.6.
Malignant pathology:
3.6.1.
Primary carcinoma of the gallbladder:7 it is an uncommon,
aggressive malignancy that affects women more frequently than men.
Older age groups are most often affected,
and coexisting gallstones are present in the vast majority of cases,
as they cause chronic irritation and inflammation of the gallbladder,
which leads to mucosal dysplasia and subsequent carcinoma.
Porcelain gallbladder is an uncommon condition in which there is diffuse calcification of the gallbladder wall,
and 10%–25% of patients with this condition have gallbladder carcinoma.
The symptoms at presentation are vague and are most often related to adjacent organ invasion,
with extension to the liver and biliary tree,
periportal and peripancreatic lymphadenopathy,
hematogenous metastases,
and peritoneal metastases,
making common that the majority of patients present with advanced disease.
Gallbladder carcinomas are epithelial in origin and account for 98% of all gallbladder malignancies.
The remainder are sarcomas,
lymphomas,
carcinoid,
metastases,
and other unusual malignancies.
The majority (68%) of gallbladder carcinomas are diffusely infiltrating lesions,
and the remainder exhibit intraluminal polypoid growth (32%).
Submucosal spread of infiltrating carcinomas appears grossly as focal or diffuse areas of wall thickening,
nodularity,
or induration in the gallbladder wall.
On T2-weighted images,
the tumor is usually heterogeneously hyperintense relative to the liver,
whereas on T1-weighted images it is relatively iso- or hypointense.
After the administration of gadolinium-based contrast an irregular enhancement is seen. Fig. 24
Treatment is limited because of the late stage of disease at presentation in most cases.
In addition,
there is no standardized therapy for gallbladder carcinoma.8
3.6.2. Lymphoma:2 Lymphoma of the gallbladder is rare and may represent primary non-Hodgkin lymphoma or may be secondary to systemic disease.
At MR imaging,
it is difficult to differentiate between primary gallbladder cancer and gallbladder lymphoma.
MR imaging findings include thickening of the gallbladder wall,
a mass in the gallbladder fossa with extension into the liver,
with the mass being hypointense on T1-weighted images and hyperintense on T2-weighted images relative to the liver; biliary obstruction; and lymph nodes in the porta hepatis.
3.6.3.
Melanoma:5 Of all the tumors that can metastasize to the gallbladder,
melanoma is by far the most common,
accounting for more than 50% of gallbladder metastases.
Most primary melanomas that metastasize to the gallbladder originate in the skin.
US findings include focal thickening of the gallbladder wall and either single or multiple intraluminal mural masses.
CT scans are similar to those on US images.
On magnetic resonance images,
primary and metastatic melanotic melanomas typically show hyperintense signal on T1-weighted images and hypointense signal on T2-weighted images because of the T1-shortening effect of melanin.
However,
because the amount of melanin within these lesions varies and other factors such as hemorrhage or necrosis may be present,
the signal characteristics are inconstant,
and a wide range of signal intensities may be seen.
3.7.
Others:
3.7.1.
Endometrial implants: Endometrial implants may occur on the surface of the gallbladder,
although it is very rare.
On MR imaging,
axial fat-suppressed T1-weighted images show hyperintense lesions on the medial surface of the gallbladder,
seen hypointense on axial T2-weighted MR image,
suggesting the presence of subacute blood.
3.7.2.
Foregut cyst:3 Ciliated hepatic cysts are rare cystic hepatic masses derived from remnants of the embryonal foregut that are embedded inside the hepatic bud during embryological development.
Very few cases hace been described,
and most of them have behaved in a benign way.
The typical image is a cyst with an atypical and heterogeneous content localized in the gallbladder fossa.
Fig. 25
3.8.
Traumatic and postsurgical findings:5
The most common location of biliary injury is the gallbladder, followed by the common bile duct and the intrahepatic ducts. Gallbladder and bile duct injury may occur due to torsion,
shearing,
or compression forces.
US is not generally used for initial study of these cases,
but can help in the evaluation of wall thickness and follow-up of intraluminal known hemorrhage or contained intra or perihepatic bilomas that are treated conservatively. MR cholangiopancreatography may demonstrate collapse of the gallbladder, intraluminal hemorrhage,
or pericholecystic fluid. Hepatobiliar contrast agents can demonstrate the exact origin and extent of bile leaks.
After cholecystectomy, either a portion of gallbladder or a variable length of the cystic duct can be left as a remnant. Fig. 26
Surgical cholangiography is performed with needle cannulation of the remnant to exclude retained stones.
The remnant is readily seen at direct cholangiography and may be seen at MR cholangiopancreatography but is more difficult to see at CT and US.
Usually,
a cystic duct remnant of 1–2 cm is left at surgery,
although remnants up to 6 cm in length may be seen.9
The most common problem associated with the cystic duct remnant is retained calculi,
followed by cystic duct leaks,
which are usually small and occur early in the postoperative period or after removal of tubes that were surgically placed via the cystic duct remnant. Fig. 27