Type:
Educational Exhibit
Keywords:
Obstruction / Occlusion, Multidisciplinary cancer care, Puncture, Complications, Percutaneous, Fluoroscopy, CT, Liver, Interventional non-vascular, Biliary Tract / Gallbladder
Authors:
A. BHARADWAZ; AARHUS, Re/DK
DOI:
10.1594/ecr2013/C-0744
Imaging findings OR Procedure details
Between 1st June and 30th November 2012,
111 consecutive percutaneous biliary interventions in 68 patients were performed.
Multiple procedures (67) accounted for 60% of all interventions compared to 40% single procedures (44).
Peripancreatic cancers and cholangiocarcinomas were the leading causes of biliary obstruction requiring biliary interventions.
All procedures were performed with therapeutic intentions.
No stand alone diagnostic PTC was performed.
Non-dilated or minimally dilated ducts were targeted by a 21G fine needle whereas obviously dilated bile ducts were punctured by an 18G needle.
Ultrasound was used for guidance in all cases.
Most patients had external-internal biliary drainage catheters placed at the end of the procedure though some had internal self-expanding metallic stents (SEMS),
plastic stents or external biliary pigtail catheters deployed.
In this series of 111 consecutive biliary interventions in 68 patients,
twelve major complications (10.8%) occurred of which 4 were vascular viz.
liver rupture with bleeding,
liver injury with hematomoa formation,
biliary venous fistula resulting in major blood loss and pseudoaneurysm of right hepatic artery with bleeding (Table).
Table: Complications following biliary interventions
| |
|
NUMBER |
PERCENT (%) |
| |
|
|
|
| Total procedures |
|
111 |
100 |
| Major complications |
|
|
|
| |
Death |
2 |
1.8 |
| |
Contributing but not directly causing death |
2 |
1.8 |
| |
Sepsis |
4 |
3.6 |
| |
Local Peritonitis |
2 |
1.8 |
| |
Abscess |
2 |
1.8 |
| |
Total |
12 |
10.8 |
| Minor complications |
|
|
|
| |
Mild to moderate pain |
7 |
6.3 |
| |
Mild fleeting infection |
4 |
3.6 |
| |
Low BP |
4 |
3.6 |
| |
No or reduced production |
3 |
2.7 |
| |
Total |
18 |
16.2 |
| Vascular complications |
|
|
|
| |
Liver rupture and bleeding |
1 |
0.9 |
| |
Liver injury and hematoma |
1 |
0.9 |
| |
Pseudoaneurysm with bleeding |
1 |
0.9 |
| |
Biliary venous fistula |
2 |
1.8 |
| |
Hemobilia stopping spontaneously |
2 |
1.8 |
| |
Total |
7 |
6.3 |
NB: The values represent number and percentage of procedures and not of patients as some patients had more than one complications simultaneously.
Note that liver rupture and biliary venous fistula leading to significant hemorrhage occurred in the same patient.
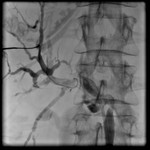
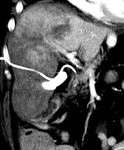
This patient,
an 83 year old female,
with cholangiocarcinoma developed hemobilia under SEMS deployment due to biliary-venous fistula formation (Fig.1).
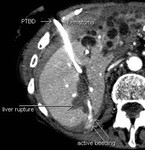
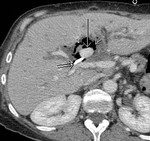
It was considered necessary to put additionally an external-internal catheter which was technically very difficult due to sharp angulation at the entry point into the bile duct.
Vigorous manipulation to put the catheter in place resulted in liver rupture and hematoma formation (Fig.2).
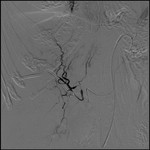
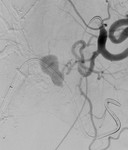
Angiography was negative for arterial bleeding (Fig.3) and patient was a poor candidate for surgery due to age and co-morbidity.
There was continued fall of hemoglobin level and patient died of circulatory failure after 4 days.
Another patient,
a 70 year old man operated with gastrectomy for stomach cancer developed duodenal blow out syndrome.
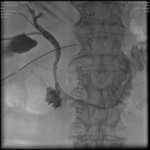
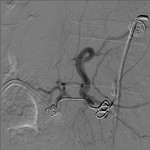
After numerous unsuccessful attempts with a fine needle (21G) to cannulate intrahepatic bile ducts,
an external-internal biliary catheter was eventually placed for bile diversion through gall bladder by transhepatic approach (Fig.4).
Post-procedural CT scanning performed due to significant drop in hemoglobin level revealed liver injury and hematoma formation from numerous punctures during failed transhepatic biliary cannulation.
No active arterial bleeding was demonstrated (Fig.5).
Surgery was ruled out because of poor performance status and the patient died after one week.
One more death was contributed to,
though not directly caused,
by pseudoaneurysm formation and bleeding after repeated biliary procedures for a patient with biliary reconstruction after removal of an intrahepatic choladochal cyst (Fig.6,7).
Pseudoaneurysm developed in the right hepatic artery was embolized with coils (Fig.8) which resulted in large areas of parenchymal ischemia and later abscess formation.
The patient died 4 months later due to multiple concurrent complications viz.
infection,
liver necrosis and repeated bleeding.
The only other case of mortality linked to biliary procedures in this series can be attributed to sepsis.
One case of biliary venous fistula was well-temponaded by upsizing the biliary catheter.
Two other cases of hemobilia stopped spontaneously.