Patients
A retrospective study was conducted in 12 consecutive patients (mean age: 35.2 years; range: 23-46) with PCS with atypical high-flow venous collaterals demonstrated during ovarian venography,
treated at our Department by B-ORTFS between June 2005 and May 2008.
Full approval and waiver of informed consent for our retrospective study was obtained by our institutional review board.
Each patient gave written informed consent prior to the procedure.
Patient population
Patients were referred for treatment by gynecologists after a diagnosis of PCS had been made by physical and color-Doppler US examination and no previous surgical treatment attempts had been performed.
High-flow venous collateral vessels were detected in all patients at the preliminary selective ovarian venography preceding trans-catheter foam sclerotherapy (TCFS),
as previously described (4).
According to the different anatomical situations that can be observed,
we classified high-flow pelvic varicoceles in:
-
non cross-pelvic varicoceles with flow through the ipsilateral hypogastric vein
-
cross-pelvic varicocele:
-
flow through the contralateral hypogastric vein
-
flow through both hypogastric veins
-
flow through the contralateral ovarian vein
-
flow through all the above venous branches
Type Ihigh-flow venous collaterals were present in 4 (33.3%) patients,
type IIa in 3 (25.0%) patients,
type IIb in 4 (33.3%),
type IIc in 1 (8.3%) and type IId in 2 (16.7%).
Ten (83.3%) patients presented continuous pain and dyspareunia,
while 2 (16.7%) patient presented urinary urgency.
A worsening of pain during menstruation was present in 5 (41.7%) patients and the coexistence of lower limb varices was observed in 5 (41.7%) patients.
Two(16.7%) patients were multiparous,
3 (25.0%) were biparous,
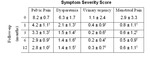
6 (50.0%) were uniparous and one (8.3%) was nulliparous (Table 1).
As previously described,
quantitative measure of symptom perception before the procedure was performed in all patients using a Symptom Severity Score (SSS) evaluating the intensity of each specific symptom (pelvic pain,
dyspareunia,
urinary urgency and menstrual pain) on a 0 (absence) to 10 (maximum intensity) scale (4).
The majority of the patients occasionally took analgesics to reduce pelvic pain.
Pelvic varicocele B-ORTFS
Treatment was performed in a Day Hospital setting.
As previuously described,
a percutaneous access was gained puncturing the right antecubital vein using a 18 Gauge needle,
after a local anesthesia had been performed with 2 ml of lidocaine (4).
After dilation with a 5 Fr 25-cm-long introducer sheath (Introducer II; Terumo Japan) placed over a 0.035” J tipped 180-cm-long hydrophilic guidewire (Radiofocus,
Terumo,
Tokyo,
Japan),
a 4 Fr Simmons 2 (Radiofocus Glidecath; Terumo,
Tokyo,
Japan) diagnostic catheter was used to selectively catheterize the left ovarian vein.
A retrograde venography was then executed by an energetic hand injection of contrast medium to demonstrate the anatomy of the pelvic varices.
In order to assess the eventual presence of right ovarian varices,
a contralateral selective ovarian venography was also performed using a 4 Fr Multipurpose catheter (Torcon NB Advantage; William Cook Europe ApS,
Bjaeverskov,
Denmark).
During venography,
in each patient,
a rapid wash-out of contrast medium from the pelvic varices through atypical high-flow branches tributary to either the hypogastric or ovarian veins was observed.
In cases of type I high-flow pelvic varicoceles,
a contralateral percutaneous common femoral vein access was gained using a 7 Fr introducer sheath (Introducer II; Terumo Japan),
whereas in case of type IIa high-flow pelvic varicoceles,
an ipsilateral common femoral vein access was gained.
Type IIc high-flow pelvic varicoceles required a contralateral antecubital venous access as described above.
Under road mapping,
the major venous vessels (hypogastric or ovarian veins) to which the high-flow collaterals were tributary were selectively catheterized using a 4 Fr Cobra 1 diagnostic catheter (Radiofocus Glidecath; Terumo,
Tokyo,
Japan) advanced over a 0.035” J tipped 180-cm-long hydrophilic guidewire (Radiofocus,
Terumo,
Tokyo,
Japan).
The catheter was exchanged with a 10 mm diameter balloon-catheter which was then inflated to occlude the vessel.
A venographic control was then performed through the balloon catheter to confirm the retrograde opacification of the pelvic varices and to exclude the presence of other atypical high-flow venous collaterals requiring balloon-occlusion.
STS foam was prepared,
as previously described,
by connecting through a three-way stopcock two 10 ml Luer Lok™ syringes containing respectively 2 ml of 3% STS (Fibrovein,
STD Pharmaceuticals) and 8 ml of air and by mixing their contents together until a homogeneous foam was obtained.
After balloon-occlusion and the complete filling of the pelvic varices with contrast media,
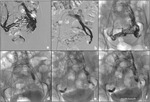
the patient was asked to perform Valsalva’s maneuver while 20-40 ml of 3% STS foam were injected until the contrast media present in the pelvic varices was completely washed-out.
The absence of contrast media in the pelvic varices indicated their complete filling with 3% STS foam (figure 1).
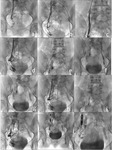
In case of complete stagnation of contrast medium after balloon-occlusion,
one of the balloon catheters was deflated creating an obliged outflow route and than re-inflated immediately after (figure 2).
The balloon-occlusion of the major veins to which the high-flow collaterals were tributary was kept for 30 minutes.
After this period a control venography was performed to demonstrate the complete occlusion of the pelvic varices.
Patients were discharged 4 hours after the procedure.
A 3-day oral anti-inflammatory (200 mg/day nimesulide) and a 5-day oral antibiotic (1 g/day amoxicillin) drug therapy were prescribed.
Follow-up
Physical examination,
a pelvic and transvaginal color-Doppler US examination and aquestionnaire-based assessment of pain using the SSS was performedat 1,
3,
6 and 12 months after the procedure.
The SSS evaluated the presence and the entity of the specific symptoms (pelvic pain,
dyspareunia,
urinary urgency and menstrual pain)during the four weeks preceding the follow-up visit.
Study Endpoints and Statistical Analysis
Study endpoints were rates of technical success and recurrence of PCS during a 12-month follow-up period.
Technical success was defined as the complete occlusion of pelvic varices at post-procedural venography with no evidence of venous flow observed at color-Doppler US.
The appearance of pelvic varices and/or return of SSS to baseline values was considered as a recurrence of PCS.
All data are given as means ± SD.
Categorical data are expressed as percentages.
The paired Student’s t test was used to assess statistical significance of differences before and after treatment (Pvalue < 0.05).
All statistical analyses were performed using theEpi Info 3.5.1 software (CDC ,
Atlanta USA).