The diagnosis should be careful with mesoblastic nephroma because their imaging findings are similar to Wilms tumor in children with one year old or less (8).
Sometimes neuroblastoma simulates the Wilms tumor presenting as a solid intrarenal neoplasm,
characterizing the undifferentiated neuroblastoma (10).
At ultrasound,
Wilms tumor commonly presents with an echogenic mass with discrete hypoechoic areas corresponding to necrosis (13).
The Doppler study can be done,
since the more vascularized,
more aggressive is it behavior (24).
The neuroblastoma,
presents itself as a heterogeneous form,
hypoechoic areas interspersed with irregular echogenic areas (13).
A "lobe" with increased echogenicity in part from a tumor,
is a secondary finding to tumor growth pattern,
but according to Amundson et al,
this "lobe" were diagnosed as neuroblastoma at anatomopathological study in all cases in which was identified ultrasonographically,
with high specificity to the method (11).
In renal tumors,
monitoring ultrasound before treatment and after the treatment,
must be performed periodically every three months.
Even after nephrectomy of the affected kidney,
the other kidney monitoring should be performed (26).
In situations where the abdominal CT scan demonstrates intratumoral calcifications,
entrapment vessels in the tumor and / or tumor extension beyond the midline,
large vessels displacement and / or kidney - the use of contrast mandatory if there is no contraindications (21) - the diagnosis of neuroblastoma is more common (6,8).
However,
are also characteristics which can be seen in Wilms tumor,
although they are much less common (6,8).
The spread around the celiac and superior mesenteric arteries,
differentiates neuroblastoma from Wilms tumor,
as is most common in the neuroblastoma (23).
Invasion of the inferior vena cava,
which can occasionally extend to the right atrium (21) is strongly predictive of Wilms tumor,
while paravertebral mass with spinal canal invasion are for neuroblastoma (8).
Tumor calcifications,
when present in Wilms tumor,
mean that tumor growth is slow,
and possibly a good prognosis sign in adult patient (16).
For neuroblastoma diagnosis,
MRI has high sensitivity,
but scintigraphy with metaiodobenzylguanidine has a greater specificity.
However,
the two methods combination increases the sensitivity and specificity of the diagnosis,
improving the accuracy of diagnosis (18).
In children with Wilms tumor,
MRI serves more as a method to answer questions or CT scans misdiagnosis (20),
especially to patency of the vena cava (21).
Comparison of radiologic findings between the two pathologies.
|
|
WILMS TUMOR
|
NEUROBLASTOMA
|
|
X-RAY
|
Outline mass with displacement of adjacent structures and lifting the diaphragm side of the lesion,
and may occasionally present calcifications (28).
|
Large abdominal mass with thin and dotted calcifications (22).
|
|
ULTRASOUND
|
Large solid mass with homogeneous echogenicity,
well-defined,
with (22) and discrete hypoechoic areas corresponding to necrosis (13),
causing distortion and displacement of the collector system and the capsule (23).
|
Solid adrenal heterogeneous mass,
poorly defined (23) and may present calcifications (22,
23,25,26),
necrosis (26) and hemorrhage (24).
|
|
CT SCAN
|
Spherical intrarenal mass (25),
heterogeneous (26) with calcifications - 13% of the cases (25) - and fat (21).
Well defined,
with mixed attenuation,
little contrast enhancement,
cystic areas due to hemorrhage and necrosis (22),
and lymph node metastasis (21).
When originates from cortex can have exophytic growth (25).
Used for staging (22,23).
|
Poorly defined mass that may have calcifications - 90-95% of cases (25,26),
occupying most of the central abdomen.
There is engagement / displacement of the great vessels,
renal vessels (22) and extending to periaortic and retrocrural lymph nodes (26).
|
|
MRI
|
Well-defined mass with relatively distinct margins (25) with predominantly low signal on T1-weighted images and high signal on T2-weighted images (22,25,26).
Often appears heterogeneous in T1 and T2 weight images (25).
Demonstrates better venous extension CT scan (25).
Used for staging (22,23).
|
Good for viewing the involvement of the spinal canal (23),
being seen as foci of low signal intensity on T1-weighted images (22).
|
|
PATHOLOGICAL
EXAMINATION
|
Variable amounts of blastema,
stroma and epithelium (27),
beyond anaplasia in 5% of these tumors (21,27),
whose finding indicates resistance to chemotherapy (27).
|
Necrosis,
hemorrhage and cystic softening areas (27).
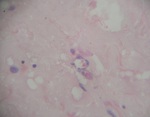
Small cell with primitive appearance with a dark core,
little cytoplasm with ill-defined margins,
embedded in a finely fibrillar matrix,
making swirling or rosette-like structures - Homer Wright rosettes - with larger primitive cells and intercellular neuronal tissue (25,
27 ).
|
The tumor response to treatment is evaluated from preoperative therapy using similar methods to those who made the diagnosis,
often in combination,
to evaluate even the resectability of the tumor,
until the postoperative period (14).
Imaging tests,
in conjunction with the patient's clinical and epidemiological data,
allow the diagnosis of pediatric renal tumors,
but the pathological examination is still necessary (7).
CASE REPORTS
CASE 1
04 years old patient,
female,
black,
born and raised in SĂŁo Vicente,
was referred to another service with a diagnosis of splenomegaly.
Mother states that the patient has abdominal pain for three days,
with abdominal distension,
worse after eating,
fever not measured 24 hours and five episodes of vomiting.
Denies comorbidities,
problems during pregnancy and medication.
On physical examination,
the mass was palpated stiffened and cylindrical to approximately 05 cm from the left costal margin extending to the left flank to the mesogastrium with pain during the deep palpation.
Negative rebound.
Remaining physical normal.
CBC showed leukocytosis (17550) and 575000 platelets.
PCR: 99.52 mg / L and urine 1with the presence of ketone bodies and calcium oxalate crystals +.
Myelogram after puncture of the iliac crest,
showing slight hypercellularity compared with leukocytes / erythrocytes 5:1.
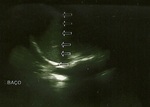
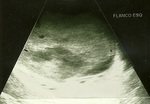
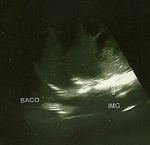
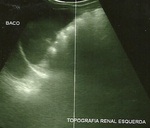
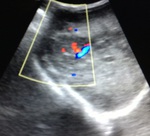
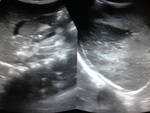
At ultrasound (Figures 1-3) was noted in the left renal topography presence of rounded image,
heterogeneous,
predominantly echogenic,
with cystic areas and hypoechoic intermingled with precise limits and regular contours,
not producing acoustic artifact and without significant flow Doppler,
pushing the spleen cephalically.
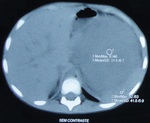
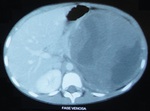
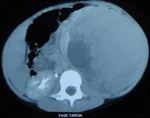
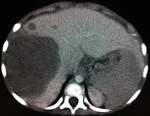
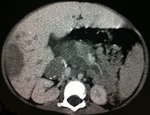
Requested abdominal CT scan (Figures 4-6) with contrast in which it was found in the left renal topography expansive formation with rounded contours,
heterogeneous,
extra-peritoneal,
showing areas of low attenuation that can be related to necrosis,
measuring approximately 20.0 x 13.5 x11,
5 cm,
extending to the pelvis with heterogeneous impregnation after infusion of intravenous contrast.
The lesion displaces the other abdominal structures to the right,
identifying compression and anterior displacement of the pancreas.
A left nephrectomy (Figure 7) performed without complications,
as well as its monitoring so far.
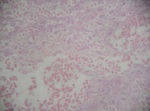
Pathological study confirmed the diagnosis of Wilms tumor (Figure 8 and 9).
CASE 2
02 years old patient,
male,
white,
born and raised in Praia Grande,
hospitalized at ISCMS for pain in the right hip for 04 months with lameness,
worsening since then,
until stop walking with orthopedic follow-up,
being treated for arthriti.
During hospitalization,
mother reported episodes of vomiting,
diarrhea,
abdominal distention,
prostration and tachycardia,
denying abdominal pain.
Denies previous medication,
pregnancy or postnatal complications.
Family history: nothing noteworthy.
At physical examination (Figure 10),
appeared pale 2 + / 4 +,
mitral systolic murmur in the Grade 3 scale ERBS,
abdominal distention with liver palpable to 04 cm from the right costal margin,
spleen palpable to 03 cm from the left costal margin,
painful deep palpation in the upper quadrants and negative rebound.
Left cryptorchidism and not painful neck and armpits adenopathy of 0.5 mm.
Knees and left elbow enlarged without signs of inflammation with atrophy of the lower limbs,
weighing about 11 kg (moderate-severe malnutrition).
Palpable lymph node in the right groin.
CBC showed leukocytosis (12800) and 153000 platelets,
plus 7.6 g / dl hemoglobin and hematocrit 24.1%.
PCR: 34.32 mg / L and ESR 76.
Albumin: 3.45
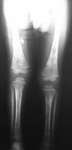
Radiographic examination (Figure 11) of the lower limbs visualized rarefaction of femurs,
tibias and fibulas.
Performed ultrasonography of the right hip,
which was found synovitis.
At abdominal ultrasound (Figures 12-14),
it was noted heterogeneous image,
irregular,
ill-defined,
with Doppler vascularity in the right hepatic lobe.
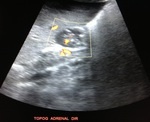
It is also visualized,
at the right adrenal topography a rounded image of imprecise limits,
predominantly hypoechoic,
with calcifications and Doppler vascularization,
measuring about 3.7 x 2.1 cm in its greatest axis.
Given these findings it was performed a complementary method.
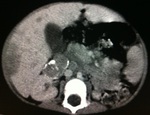
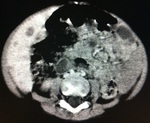
At abdominal CT scans (Figures 15-18),
there were multiple rounded formations of indeterminate nature,
predominantly hypodense,
well delineated,
showing heterogeneous impregnation after the infusion of intravenous contrast,
especially one in the right hepatic lobe measuring approximately 11.0 x 8.3 x 6.45 cm in its greatest axis.
It was also noted bilateral lymphadenopathy,
left perihilar para-aortic and interaortocavais with a confluent aspect and an expansive formation,
ovoid,
heterogeneous,
predominantly hypodense with calcifications inside,
measuring about 3.7 x 2.2 cm in its major axis in the right adrenal,
with indeterminate nature by the present study.
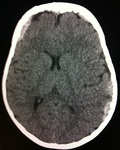
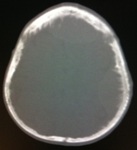
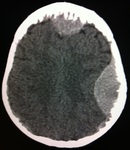
Head CT scan (Figures 19-21) observed an expansive,
extra-axial,
related skullcap in the midline front projection and bilateral parietal,
associated with bone spiculated periosteal reaction in internal diploe.
The lesions promote mass effect with compression of the adjacent parenchyma and measure about 2.0 cm thick in front projection and about 2.5 cm in the left parietal projection.
Made lymph node biopsy in the right inguinal region in which found reactive lymphoid hyperplasia (Figure 22).
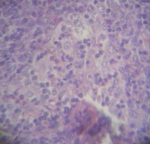
Myelogram shows infiltration by rosette tumor cells,
suggesting neuroblastoma.
After those tests,
the chemotherapy started.