Multidetector Computed Tomography (MDCT) is recommended as the imaging modality of choice to assess SRH.
- Unenhanced scans are usually sufficient to detect fresh blood collections,
which appear hyperdense (40 to 70 Hounsfield Units) (fig.
04).
However,
unless contraindicated a multiphasic contrast-enhanced acquisition is strongly recommended to better assess severity,
anatomical extent and underlying cause
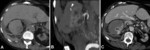
- An early acquisition (30 to 40 seconds delay) after intravenous contrast medium administration provides an arterial phase scan that is necessary to detect or rule out active contrast extravasation indicating ongoing bleeding (fig.
05).
- The venous phase acquisition (70 to 90 seconds) is most useful to detect the underlying cause.
Although determining the aetiology may be challenging,
with a correct multiphasic technique the specificity of CT has been reported to approach 90%.
- Additionally,
the (optional) excretory phase acquisition allows to diagnose or rule out extravasation of opacified urine,
which leads to the formation of an urinoma (fig.
06).
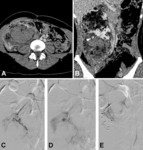
Multiplanar MDCT images consistently provide an accurate assessment of the haematoma’s extent and topography.
Intraparenchimal haematoma (fig.
02)
- usually has a limited size
- has a round or ovoid shape
- can be surrounded by intact parenchyma
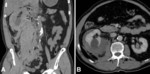
Subcapsular haematoma (fig.
03,
04,
05)
- is a well-demarcated collection
- has a convex interface with the kidney producing a lenticular or linear shape
- causes bulging of renal capsule
Perinenal haematoma (fig.
03,
05,
07,
08,
09)
- is confined within anterior and posterior pararenal fasciae
- forms a crescent – shaped collection along the side of the kidney
- may follow a path along bridging perirenal septa,
producing a linear or curvilinear pattern
- may extend inferiorly in the retroperitoneum and inside the peritoneal cavity
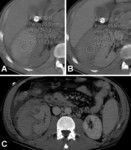
Perirenal hematoma should be differentiated from subcapsular hematoma,
since the latter may lead to compression of renal parenchyma and loss of function (fig.
04C).
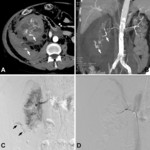
Transarterial angiography with embolization is indicated when active bleeding is detected at contrast enhanced CT (fig.
02,
07).
This minimally invasive procedure allows a rapid control of the bleeding,
obviating emergency invasive laparotomy and nephrectomy.
Vascular access is generally obtained via the common femoral artery.
Embolization is performed with coils,
polyvinyl alcohol (PVA) particles,
microspheres,
and/or Gelfoam.
Superselective catheterization (fig.
02) of renal artery branches with microcatheters provides controlled occlusion of specific small renal artery branches,
with very little effect on the surrounding normal renal parenchyma and sparing of renal function.
When nephrectomy is inevitable,
pre-operative embolization (fig.
07) of the renal artery or of its segmental/lobar branches provides tumour angioinfarction,
decreases intraoperative blood loss,
and allows a less-extensive surgical resection in case of renal tumors.