GASTROINTESTINAL TRACT PATHOLOGIES
Necrotizing enterocolitis (NEC)
Necrotizing enterocolitis is a serious abdominal disorder of premature neonates; it usually affects the terminal ileum and ascending colon.
Clynical symptoms include abdominal distension,
hematochezia,
apnea,
acidosis,
temperature instability,
lethargy.
Diagnosis is usually made on the basis of abdominal radiographs showing pneumatosis,
a thick-walled bowel,
free air and portal venous air.
Sonography may be useful when perforation and abscess formation are suspected.
Mural thickening of the terminal ileum and ascending colon may be shown.
Free intrabdominal fluid containing echogenic debris or a loculated right lower quadrant mass suggests perforation and abscess formation.
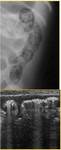
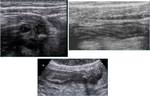
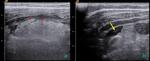
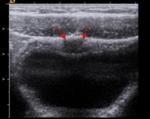
Intramural gas (Fig. 5) is an early sign that may precede clinical signs.
Although abdominal US can depict intraluminal bowel gas,
it does not display the pattern of gaseous distention as well as plain abdominal radiography.
The commonest cause of portal venous gas in neonates is the passage of small amounts of gas through an umbilical venous catheter in the absence of NEC.
In NEC,
portal venous gas is an extension of intramural gas that enters the veins of the bowel wall and passes into the portal venous system.
Portal venous gas has been reported on plain abdominal radiographs in up to 30% of neonates with NEC and these are usually,
but not always,
the more severely affected cases.
Portal venous gas is not always associated with a fatal outcome.[3]
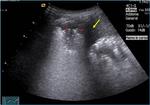
Congenital intestinal obstruction
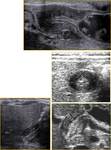
Congenital intestinal obstruction is the most common condition producing a distended and tender abdomen in an irritable neonate.
Diagnosis of obstruction is usually made by plain radiographs and contrast studies.
Sonography can show free fluid,
bowel distension,
thickened bowel wall,
iperperistaltism or absence of peristalsis.
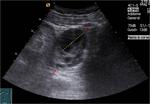
Fig. 6
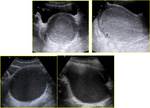
Hypertrophic pyloric stenosis
Premature infants tend to present at 3-6 weeks from birth.
Hypertrophic pyloric stenosis is rarely seen in children older than 6 months.
Clinical presentation is characterized by nonbilious projectile vomiting and dehydration (with hypochloremic metabolic alkalosis).
In hypertrophic pyloric stenosis,
the circular muscle layer becomes thickened,
which narrows the pyloric channel and elongates the pylorus.
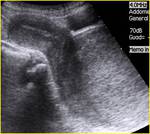
Normal pylorus. Fig. 7
The first and most important step in patient workup of suspected hypertrophic pyloric stenosis is a thorough physical examination.
If the clinical suspicion for hypertrophic pyloric stenosis is moderate to high,
ultrasonography is also recommended.
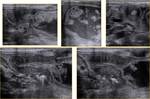
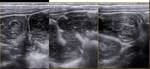
Ultrasound specific signs of Hypertrophic pyloric stenosis are:
1) elongation of the pyloric channel: DL > 17mm (range 15-20mm)
2) Antero-posterior diameter of the pylorus > 12mm
3) Thickness: >2mm (range 2.5-4mm)
Fig. 8
Indirect signs of Hypertrophic pyloric stenosis:
- gastric distension
- gastric hyperperistaltism
- alteration of gastric peristalsis + gastroesophageous reflux.
- shoulder sign
- beak sign
- double track sign
The shoulder sign is seen during barium examination and refers to the bulging of the hypertrophied pyloric muscle into the lumen of the antrum.
The "beak" sign is peak of barium entering the narrowed pyloric channel.
Cohen HL et al.
performed a fluid aided real-time ultrasound examination of 10 cases of hypertrophic pyloric stenosis,
showing the ultrasound equivalent of the "double track" sign.
This finding is the result of pyloric fluid compressed into smaller tracks as it is impinged upon circumferentially by the thickened circular muscle.
This sign,
previously seen in barium studies,
although nonspecific,
may prove to be a sensitive ultraound diagnostic criterion.
Fig. 9 Fig. 10
A negative ultrasonogram often leads to a upper gastrointestinal study (UGI study) to rule out other diagnoses that a focused ultrasonographic evaluation does not detect.
This study more effectively rules out other problems,
such as malrotation and gastroesophageous reflux.[4]
Intestinal intussusception
M>F; peak age between 3 and 9 months.
Intussusception occurs when a portion of the digestive tract becomes telescoped into the adjacent bowel segment.
The traditional diagnostic approach to childhood intussuscption of plain radiography and enema examination is being changed to plain radiography and ultrasonography at some istitutions.
The classification of this condition depends on the gastrointestinal tract involved:
-
Colo-colic
-
Ileo-cecal (the most frequent in children)
-
Ileo-ileal
-
Ileo-cecal-colic
Intussusception is usually idiopathic in the first year of age; in the olders it recognizes a lot of different causes (appendicitis,
lymphoma,
Meckel's diverticulum,
celiachia,
gastronintestinal duplication cyst,
etc).
On cross section the usual sonographic image is a "target" or "doughtnut" appearance; the longitudinal appearance is that of a pseudokidney characteristic of thickened bowel.
Other ultrasound signs suggestive of intussusception are: double ring sign at Dolor doppler US,
large adenopathies,
free fluid,
bowel distention.
Fig. 11 Fig. 12
In some cases,
if the onset of intussusception is recent and blood is absent in the fecies,
it is possible try to resolve the pathology during the ultrasound examination.
Indicators of ischemia and irreducibility are trapped fluid at US and absence of blood flow at Doppler imaging.
In our institution we usually perform sonographically-guided hydrostatic reduction by contrast enema.
Fig. 13 The aim of enema therapy is to reduce the greatest number of intussusceptions without producing perforation.
Barium,
water-soluble contrast media,
water,
electrolyte solutions,
or air may be used with radiographic or US guidance.[5]
Acute appendicitis
It represents 80% of surgical pediatric emergencies.
Clinical presentation could be unusual,
expecially in the youngers.
For this reason it could be discovered in the late stage when an abscess or diffuse peritonitis is present.
Clinical signs of acute appendicitis are: abdominal pain,
fever,
elevated WBC,
nausea,
leg pain,
lower right thoracic pain,
etc.
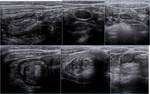
At ultrasonography the appendix appears enlarged,
thickned,
with endoluminal fluid and/or appendicolith; other US findings are hyperechoic mesentery,
lymphadenopathies,
free fluid,
abscess.
Fig. 14 Fig. 15 Fig. 16
Doppler examination can show an increase of vascularity of the appendiceal wall in the first stage and loss of vascularity in the late stage.
Failure to identify the appendix by ultrasound or identification of a normal appendix less than 6 mm in diameter,
makes the diagnosis of appendicitis very unlikely.
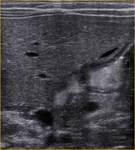
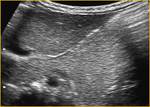
Differential diagnoses in patients with suspected appendicitis are Chron's disease Fig. 4,
ovarian pathologies,
mesenteric adenitis,
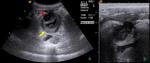
nephrolitiasis and Meckel's diverticulitis Fig. 2.[3,6,7]
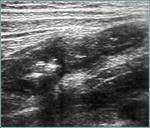
Mesenteric adenitis
It can mimick appendicitis because it causes abdominal pain,
fever and elevated WBC.
Mesenteric adenitis is classified as primary or secondary depending on wether an identifiable inflammatory process can be found (secondary) or not (primary).[7]
Ultrasound examination shows several enlarged nodes in the mesentery. Fig. 17
Omental torsion
Omental torsion is a rare cause of acute abdominal pain,
and clinically mimics acute appendicitis.
Torsion of the omentum is a condition wherein the organ twists along its long axis to such an extent that its vascularity is compromised.
Although omental torsion is rarely diagnosed preoperatively,
knowledge of the entity is important to the surgeon because it mimics the common causes of acute surgical abdomen.[8,9]
Fig. 18
Other causes of gastrointestinal pain
Fig. 19
Small intestine duplication
In 1937,
Ladd introduced the term duplication of the alimentary tract.
This condition consists of a group of congenital anomalies with the following 3 characteristics:
- A well-developed coat of smooth muscle is present.
- The epithelial lining represents some portion of the alimentary tract.
- Duplications are frequently intimately attached to some portion of the gastrointestinal tract.
Clinical presentation depends on the type,
size,
location,
and mucosal lining of the duplication.
Cystic duplications of the small intestine can be anchor points for intussusception or can result in volvulus,
whereas long tubular duplications with proximal communication drain poorly,
and retention of intestinal contents can obstruct adjacent intestine.
Distal communication is more common and is more difficult to diagnose than proximal communication.
The diagnosis is often not established before surgery.
Fig. 20
URINARY TRACT PATHOLOGIES
Acute dilatation of the renal pelvis can produce abdominal pain,
particularly in younger children; in some of these the pain may be appreciated as midline in the abdomen.
Obstruction is usually at the ureteropelvic junction.
Pyelonephritis with distension of the renal capsule can produce similar pain.
In most children,
pain is localized at the groin or flank.
Clinical signs of urinary tract disorders are: dysuria,
fever,
abdominal pain,
haematuria,
pyuria,
etc.
Ultrasound can show hydronephrosis and its degree,
stones,
thickened bladder walls,
alteration of urine echogenicity.
Fig. 21
Pyourachus
Infected urachal remnant can represent a cause of right lower quadrant pain.
The urachus is an embryonic remnant resulting from the involution of the allantoic duct and the ventral cloaca.
An urachal cyst develops if the urachus remains patent between the umbilicus and the bladder.
Infection of such cysts occur more commonly in adults and only occasionally in children.
Infected urachal cysts usually present with lower abdominal pain,
fever,
midline hypogastric tenderness,
palpable mass and evidence of urinary infection.
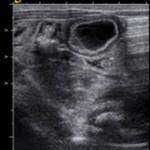
The preferred imaging method for the diagnosis of urachal cyst is ultrasound,
which will show a midline cyst between the umbilicus and the bladder; in cases of sovrainfection (pyourachus) ultrasound will demonstrate wall thickening,
internal debris and complex echogenicity.[10]
Fig. 22 Fig. 23
GYNECOLOGIC DISORDERS
Common gynecologic diseases in the pediatric population that can present with lower quadrant pain include surgical emergencies such as ovarian torsion,
ovarian tumors and hemorrhagic ovarian cysts.
Imperforate hymen is a rare congenital anomaly which emergency physicians often forget to include in the differential diagnosis of lower abdominal pain in a pubescent girl.
These patients often remain asymptomatic until puberty and present in early adolescence with cyclic abdominal pain and ultrasonographic evidence of a pelvic mass (haematometrocolpos,
haematocolpos).
Neonatal hydrometrocolpos is a rare condition that follows congenital vaginal obstruction.
Association with urinary obstruction and upper tract dilatation has been reported in some cases.
Obstruction of the gastrointestinal tract without a coexisting bowel anomaly can also occur,
but this is very rare.
In some cases,
preoperative diagnosis may be difficult.
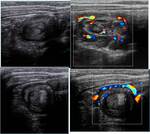
Ovarian torsion
Ovarian torsion results from rotation of the ovary on its pedicle,
producing vascular congestion and ultimately hemorrhagic infarction.
In may occur in the presence of a cyst Fig. 24 or tumor or in a normal adnexum.
The twisted ovary appears sonographically enlarged and hypoechoic.
Color doppler US demonstrates the absence of blood flow in the ovary.
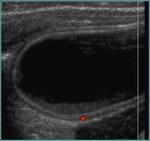
Ovarian cysts
Ovarian cysts may produce pain seconday to pressure on adjacent structures,
hemorrhage or torsion.
Hemorrhagic cysts usually are complex masses with internal echoes,
septations or fluid-debris levels.
Fig. 25 [7]
Neonatal Hydrometrocolpos
It is characterised by an expanded fluid filled vaginal cavity with associated distention of the uterine cavity.
It may present in infancy with a lower abdominal mass,
or be delayed till menarche.
It is caused by the influence of the mother’s hormone stimulation.
It occurs in presence of imperforated hymen (most common),
vaginal stenosis,
lower vaginal atresia,
cervical stenosis.
Fig. 26
The clinical features of hydrometrocolpos in the newborn are dominated by the abdominal mass with regional compression.
Compression of the lower urinary tract has been reported to cause hydronephrosis,
but compression of the gastrointestinal tract with obstruction to the passage of meconium is rare.[11]
Haematometrocolpos/haematocolpos
It refers to a blood filled distended uterus and vagina.
It occurs in presence of an imperforated hymen,
vaginal stenosis or vaginal atresia.
The estimated incidence in teenagers is at ~ 1 in 1000 - 2000 5.
If large enough it can cause obstruction of regional lymph drainage or obstructive hydronephrosis.
Fig. 27 Fig. 28
REFERRED PAIN
Some extra-abdominal pathologies,
including diseases of the spine and chest,
and metabolic disorders such as sickle cell anemia may appear as an acute abdomen.
This conditions should be suspected if abdominal imaging findings are negative.
Pneumonia of the lower lobes may occasionally be diagnosed during the abdominal ultrasound examination.
Fig. 29