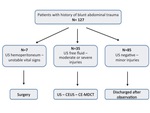
35/127 patients were considered eligible to be included in the study (Fig. 1).
3/35 patients were negative at MDCT examination.
In the remaining 32 patients,
MDCT depicted 35 lesions (left kidney n=11; right kidney n=3; spleen n=9; pancreas n=2; liver n=5). Active bleeding was present in 4 cases,
urinoma in 1.
CEUS identified 30/35 lesions and no lesions in the patients with negative CE-MDCT findings.
CEUS missed 3 active bleedings and the urinoma.
Unenhanced US depicted 9/35 parenchimal lesions.
Thus,
the diagnostic performance of CEUS was much better than that of US,
as sensitivity,
specificity,
PPV,
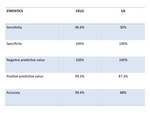
NPV and accuracy in the evaluation of parenchimal lesions were 96.6%,
100%,
100%,
99.3% and 99.4% for CEUS and 30%,
100%,
100%,
87.3% and 88% for US (Table 1).
CE-MDCT is the most used and sensitive imaging modality in traumatic lesion assessment.
It is able to depict both parenchimal and vascular lesions (including active bleeding) which are the major predictors of non surgical management [3].
Baseline US has a low sensitivity in the detection of parenchimal lesions and,
as hemoperitoneum is not always present in patients with solid organ injuries,
it is not reliable in the exclusion of traumatic abdominal lesions [4,5].
Emery et al [6] found that 34% of US negative examination children had an intrabdominal injury at CT and so reached the conclusion that screening US for the depiction of blunt abdominal trauma should be approached with caution.
The introduction of US contrast agents has led to an increase in the diagnostic accuracy of US in many organs and many studies conducted to assess trauma in adults have showed that its sensitivity is almost the same as that of CE-MDCT [7,8].
During the CEUS examination,
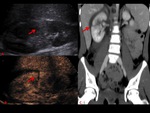
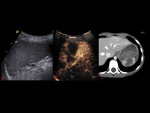
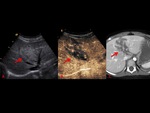
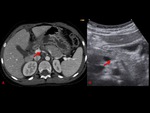
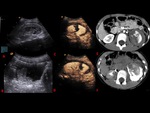
organ injuries appear as strongly hypoechoic areas compared to the homogeneous echogenicity of the surrounding parenchyma (Fig. 3).
In our study we were able to correctly identify at CEUS examination 30/30 solid organ lesions,
with great accuracy in defining also the extension of the lesions compared to CE-MDCT (Fig. 4,
Fig. 5, Fig. 6).
The sensitivity,
specificity,
PPV NPV were significantly higher than those of baseline US,
with good agreement with CT findings.
Our limits were active bleeding and urinomas.
Regarding urinomas we can say that US contrast agents are intravascular and are therefore unsuitable for demonstrating extravasation in the renal collecting system (Fig. 7).
As concern the active bleeding,
we must consider the fact that these are preliminary results obtained from an initial experience in a limited number of patient; in fact Valentino et al.
[9] has previously reported good results in the depiction of active bleeding with CEUS examination in abdominal trauma.
Therefore further studies are needed to confirm and extend our findings.
No adverse effect were observed.