349 HIV positive patients were seen in a specialist joint HIV/rheumatology clinic between 4/2/2002 and 1/12/2011. Of this group of patients a number of specific diagnoses were made with the help of imaging.
Multi-modality imaging of HIV associated myopathy,
arthropathy,
spondyloarthrophy,
musculoskeletal infection and neoplasm from our institution are demonstrated.
Arthropathies
Arthalgia and arthritis was the most common complaint in HIV positive patients our joint HIV/Rheumatology clinic. The classification can be difficult as patients often present with non-specific symptoms and incomplete manifestations of specific arthritides.
The picture is further complicated by the fact that patients may have pre or co-existing conditions,
for example,
spondyloarthritis or rheumatoid arthritis,
or joint manifestations secondary to the HIV virus itself – studies have shown that HIV related P24 antigen can been isolated from synovial tissue in HIV positive patients with arthritis.
Reiter syndrome has been linked to HLA B27 in both HIV positive and negative individuals.
Reiter syndrome has been described in HIV infected patients following infection withYersinia,Salmonella,
andShigellaspecies but may follow an incomplete course from the classic triad of urethritis,
conjunctivitis and arthritis.
In fact axial skeleton involvement and uveitis are uncommon. In some series the prevalence of Reiter syndrome is higher in HIV infected individuals; this is most marked in sub-Saharan populations where the incidence of spondyloarthropathy is almost zero outside of the HIV infected population.
The classic imaging findings of Reiter syndrome are asymmetric joint involvement with erosions and new bone formation and a predilection for paravertebral ossification.
It particularly affects the small joints of the lower extremity.
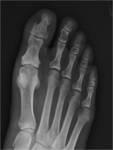
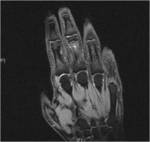
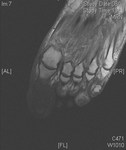
Psoriatic arthritis has been described as having a higher incidence in HIV populations and this is reflected in our institutional experience.
Clinically it has similar manifestations to those of Reiter syndrome,
except there is a greater predilection for the small articulations of the wrist and hand (fig 1).
Psoriatic arthritis tends to be polyarticular and asymmetric,
in which case it rapidly progresses to a deforming and incapacitating form of the disease.
Involvement of the sacroiliac joint and spine is rare.
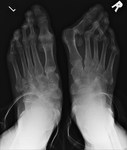
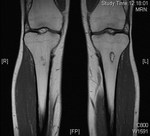
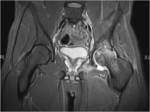
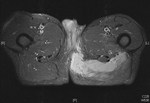
HIV associated arthritis can occur. It is classically oligoarticular,
asymmetrical and peripheral,
commonly affecting the knees and ankles (fig 2).
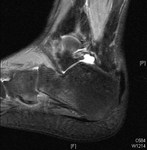
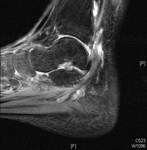
It usually has a brief course (< 6-8 weeks) and imaging may be unnecessary. In our experience this entity is usually diagnosed clinically although we present one case of a patient with monoarticular pain and swelling who had an MRI scan demonstrating a joint effusion of the ankle and incidental tenosynovitis of the posterior tibial tendon (fig 3).
Some patients with HIV associated arthritis have been reported to have a disease course of longer than 6 weeks with joint destruction,
although radiographs of the affected joints are often normal.
The relationship between HIV and rheumatoid arthritis (RA) is controversial. It was initially postulated that RA should improve with the onset of HIV due to the reduction in autoreactive T lymphocyte mediated joint inflammation and synovitis.
However,
several case series have shown the opposite effect with worsening of pre-existing RA or the development of a symmetrical polyarthritis indistinguishable from RA other than being seronegative for the rheumatoid factor. In our experience we encountered both clinical entities and imaging was able to suggest the diagnosis based on both the pattern of synovitis and the finding of worsening classical RA deformities in the presence of HIV infection (fig 4). Documented radiographic findings in symmetrical polyarthritis include osteopaenia,
soft-tissue swelling,
joint effusions,
joint space narrowing,
marginal erosions,
periosteal reaction,
and joint deformities such as flexion contractures,
ulnar deviation,
and swan neck deformities (fig 5). It has been suggested that proliferative bone formation and periostitis is a radiological feature that can help differentiate symmetric polyarthritis of HIV from RA.
Miscellaneous
Adult onset Stills disease (AOSD) is a poorly understood condition that is thought to occur due to an immune reaction to an infectious or other trigger.
In the context of HIV infection it is proposed that immune dysfunction and dysregulation of T cell number and function in combination with the commencement of HAART causes a rapid shift in the T cell mediated immune system and triggers what is known as immune reconstitution inflammatory symdrome (IRIS).
These changes can precipitate the onset or deterioration of infectious,
malignant and autoimmune conditions.
IRIS is thought to result from rapid,
marked restoration of pathogen-specific immune responses usually within the first 8 weeks of HAART. Symptoms are myriad and include fevers,
arthralgia and rash.
Patients are usually negative for RF and ANA. In our experience we saw one patient fulfilling the criteria for AOSD in HIV who had sudden onset fevers,
arthralgia and rash following 12 days of HAART.
He was managed with a long course of steroids and subsequent imaging for knee and hip pain demonstrated multiple bone infarcts in the femur and tibia thought most likely to be a complication of corticosteroid therapy.
Radiologically an important feature in differentiating bone infarct from other medullary lesions is that the central signal usually remains that of normal marrow. The marrow is not replaced.
T1WI may show a serpigionous peripheral low signal due to granulation tissue and to lesser extent sclerosis with a central signal usually that of marrow (fig 6).
On T2WI a  double-line sign may be seen similar to in avascular necrosis (AVN) (see below),
this consists of a hyperintense inner ring of granulation tissue and a hypointense outer ring of sclerosis
double-line sign may be seen similar to in avascular necrosis (AVN) (see below),
this consists of a hyperintense inner ring of granulation tissue and a hypointense outer ring of sclerosis
AVN is something that is encountered frequently within our HIV population. The incidence of osteonecrosis has been reported as 4.4% in the HIV population which is higher than the general population. There are several possible reasons for this including: Protease inhibitor mediated hyperlipaemia or impairment of corticosteroid metabolism,
higher alcohol intake,
radiation therapy and opportunistic infection. The radiological findings do not differ from those seen in the general population. MRI is the most sensitive modality often showing the classic ‘double line’ sign of infarcted subcondral bone adjacent to normal bone marrow (fig 7)
HIV associated polymyositis is a recognised entity occurring in less than 1% of HIV infected patients. Myositis in patients with HIV infection and AIDS can be a result of host response to the virus,
secondary to zidovudine (formerly called azidothymidine [AZT]) therapy,
or caused by opportunistic infections such as toxoplasmosis.
The presentation is that of muscle weakness and raised creatinine kinase with a classic proximal muscle distribution with sparing of the facial and extra-ocular muscles in HIV. Skin involvement is unusual.
Definitive diagnosis is with muscle biopsy although imaging may play a role in suggesting the diagnosis with MRI being the most useful test. T1WI shows signal isodense to muscle,
T2 or STIR will show high signal (fig 8). Unlike pyomyositis,
another muscular complication in HIV,
there is no rim of enhancement on post-contrast sequences.
Infectious
Pyomyositis is a more common manifestation in HIV. This is usually the result of opportunistic infection with Staph aureus,
although other organisms can be implicated including; S pyogenes,
Mycobacterium tuberculosis,
M avium-intracellulare,
Nocardia asteroides,
Cryptococcus neoformans,
and Toxoplasma. The clinical presentation consists of three stages: Pain in one muscle group and low grade fever; followed by increasing pain,
fever and oedematous change; and finally development of an abscess with necrosis of the muscle and worsening systemic illness. CT is useful in demonstrating the asymmetry in muscle size,
oedema and collections.
MRI is more sensitive for early changes. Internal abscess signal may vary on T1 and T2WI depending on the protein content.
As already mentioned contrast rim enhancement is a classical finding.
Osteomyelitis is another infectious musculoskeletal process more commonly encountered in the HIV population than the general population. Like pyomyositis the most common organism isolated is S aureus,
though infection with any number of organisms including mycobacterium tuberculosis,
E coli,
C neoformans and N gonorrhoea are encountered. The radiological findings are not specific to HIV infection. Plain radiography may be normal in the early stages of infection; later showing soft tissue swelling,
periosteal reaction,
cortical destruction and sequestration.
Bone scintigraphy is sensitive for infection,
but its specificity is poor with false positives seen in trauma and degenerative change.
MRI has been shown to be most sensitive and specific for the diagnosis of osteomyelitis,
82%–100% and 53%–83% respectively as published by Santiago et al.
Areas of bone oedema and pus appear as low signal on T1WI (fig 9) and high signal on T2WI. Contrast enhancement can demonstrate areas of bone and soft tissue infection as well as demonstrating necrotic bone.
Bacillary angiomatosis is an unusual form of osteomyelitis that specifically affects the HIV infected population. Patients present with cutaneous lesions due to haemangioendothelial proliferation in the skin. Bone lesions on imaging tend to be osteolytic foci that may range from well-circumscribed lytic lesions involving the cortex to ill-defined lesions with extensive cortical destruction,
medullary permeation,
and periosteal reaction.
CT and MRI are more sensitive,
especially MRI where the lytic lesions appear dark on T1WI and bright on T2WI.
Septic arthritis resulting from opportunistic infection is seen in the context of HIV infection but is surprisingly uncommon outside of the context of concurrent intravenous drug use.
As with pyomyositis and osteomyelitis a number of organisms may be implicated and as well as bacterial and mycobacterial infection,
fungal causes should be considered.
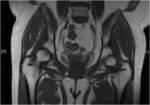
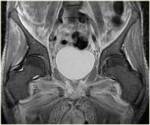
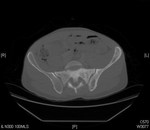
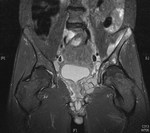
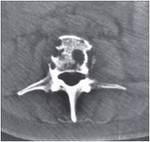
We present a case of mycobacterium tuberculosis (TB) infection of the hip joint from our institution to highlight some of the imaging findings of this condition (fig 10). In TB septic arthritis the history is often more protracted with gradual onset of pain and immobility of the affected joint.
Findings on radiography may include soft tissue swelling,
osteopaenia,
loss of joint space and destruction of the articular surfaces. MRI is more sensitive to early changes and may show marrow and soft tissue signal abnormalities due to oedema,
septic bursitis or extra-articular spread.
Neoplastic
Musculoskeletal neoplastic manifestations that may be seen in HIV infection include lymphoma and Kaposi sarcoma. The incidence of non Hogkins lymphoma (NHL) is 60 times greater in HIV positive patients compared with the general population. It tends to be a feature of late stage HIV with CD4 counts < 200 cells per microlitre and as such is considered an AIDS defining illness.
Primary lymphoma of bone is rare outside the context of immunosuppression but has been described in HIV infection,
most commonly affecting the lower extremity,
spine,
pelvis and skull. Radiological appearances are varied and lymphoma can produce lytic,
sclerotic or mixed lesions but usually without a marked periosteal reaction.
Commonly there is a permeative pattern with an accompanying soft tissue mass often in the psoas muscle,
pelvis or lower limb. CT is the first line investigation of choice as it has the ability to detect bone and soft tissue changes (fig 11) as well as stage the patient for distant lymph node sites. MRI has improved soft tissue and bone marrow evaluation as an advantage and can be helpful following CT to assess the extent of disease and target an appropriate biopsy site (fig 12,
13).
Bone marrow changes are commonly seen as low signal on T1WI and high signal on STIR sequences.
Kaposi sarcoma (KS) is a low to intermediate grade mesenchymal tumour that involves the lymphovascular system.
The tumour can have multi organ involvement inclusive of the pulmonary,
gastrointestinal,
cutaneous and musculoskeletal systems.
In the musculoskeletal system it is a rare finding in isolation and is commonly seen in the context of multifocal disease or local extension of a soft tissue mass. Radiographic findings include permeative,
erosive lesions with periosteal reaction.
CT and MRI add further information about extent of bony destruction (fig 14) and marrow infiltration/soft tissue involvement respectively.
Wu et al describe scintigraphy as useful in further characterization,
showing red blood cell pooling,
thallium-201 uptake,
and no abnormalities at Ga-67 scintigraphy.
Infection and tumours such as lymphoma show avidity to gallium instead,
making scintigraphy a potential tool for narrowing the differential diagnosis.