PATIENTS
Between January 2010 and December 2012 a total of 352 consecutive patients who arrived in our Emergency Department with an history of low-energy isolated abdominal trauma and in stable haemodynamic conditions were analyzed (224 males; 128 females - mean age 27±2.8 years).
The major causes of blunt abdominal trauma are reported in Table 1.
All patients underwent US and CEUS with the use of a second-generation contrast agent (Sonovue,
Bracco-Milan,
Italy).
Written informed consent was obtained from all the patients or from their relatives in case of minors.
Only the patients with positive CEUS findings for abdominal injury were then studied with CE-MDCT.
The patients with negative CEUS findings and negative clinical and laboratory tests underwent no further imaging investigation; a phone call was made to all patients one week later to know whether they had got any symptom related to the trauma.
Patients who referred symptoms and presented any alteration in laboratory tests were recalled and subjected to a new CEUS examination.
EXAMINATION TECNIQUE
Conventional ultrasound and contrast-enhanced ultrasound were performed with a Siemens ACUSON Sequoia 512 (Siemens Medical Systems,
Forchheim,
Germany) using a curved array 4 Mhz multi-frequency.
After the abdominal baseline ultrasound,
in the same session,
CEUS was performed with an intravenous bolus injection of a second-generation blood pool contrast agent (Sono Vue,
Bracco,
Milan,
Italy) consisting of stabilized microbbubbles (MB) of sulfur hexafluoride gas covered by a stabilizing phospholipidic membrane.
The Sequoia system was equipped with contrast pulse sequences (CPS) software which detects the MB’s fundamental nonlinear response; a continuous low mechanical index (MI 0,15-0,19) real time tissue harmonic imaging (Cadence) allows real-time gray scale imaging.
A total of 4,8 ml of Sonovue was administrated through a 18G needle put in an antecubital vein,
fractionated into two 2,4 ml doses followed by 5-10 ml of saline [1-4].
For pediatric patients Sono Vue dose has been calculated as follows: age in years /10 in ml [5].
Immediately after the first bolus the right-sided organs (the right kidney and the liver subsequently) were explored for 1-3 min.
With the second dose left side organs (the left kidney and finally the spleen) were focused for other 3-4 minutes [3].
Only patients with positive CEUS findings underwent CE-MDCT examination within 1 hour after CEUS,
using a standard arterial and venous protocol with a 16 detector CT scanner (16 LightSpeed ,
GE Healthcare,
USA) .
No patients received oral contrast medium and all patients had a pre-contrast acquisition series.
A non ionic contrast medium volume of 100-150 ml was injected at 2-4 ml /sec through a 18-20 G angiocatheter . A delay ranged from 40 to 50 sec was used for the arterial phase and from 80 to 100 sec for the second acquisition; in presence of collections,
a late-phase study (3-15 min) was performed to identify any active bleeding or urinoma.
DATA COLLECTIONS
On US a parenchymal traumatic lesion was depicted as an intraparenchymal hyper or hypoechoic area or a distorsion of the normal echoic structure [1-4].
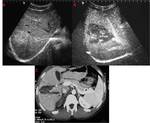
On CEUS examination traumatic injury was identified as a perfusion defect represented by an hypoechoic area with ill- or well-defined margins with or without interruption of the organ profile.
Lacerations can appear as a hypoechoic linear lesion,
usually oriented perpendicular to the organ surface.
(Fig. 1)
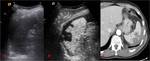
Haematomas are represented by non-enhancing areas.
(Fig. 2).
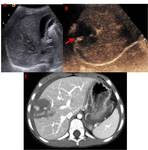
Focal extravasation of microbubbles outside a lacerated organs suggest active bleeding (Fig. 3).
We evaluated the presence and number of traumatic lesions in US,
CEUS and CE-MDCT and the lesions' grading on CEUS and CE-MDCT,
comparing CEUS results with US findings for lesion numbers and with CE-MDCT values for number and grading.
For the CEUS and CT grading of lesions we used the America Association for the Surgery of Trauma (AAST) classification [6-7].