1.
Introduction:
Ischiofemoral impingement is caused by a narrowing of the ischiofemoral space and leads to muscular,
tendon and neural changes.
Patients present with nonspecific hip and groin pain,
raising a wide range of differential diagnoses.
2.
Differential diagnosis of hip pain:
Positive results for IFI in our study were seen in 11 studies corresponding to 10 patients (12%) between 28 and 64 years old (mean age of 44).
One patient had an operation after diagnosis and an MRI was repeated after surgery.
Other positive results from the MRI images included femoroacetabular impingement (FAI) in 32 patients (32%),
trochanteritis in 4 patients (4.4%),
sacroileitis in 3 patients (3.3%),
bursitis in 2 patients (2.2%),
avascular necrosis of the femoral head in 2 patients (2.2%),
sequelae of Perthes in 2 patients (2.2%),
1 case of liposarcoma (1.1%) and 1 acetabular fracture (1.1%).
3.
IFI and anatomy of the hip:
Our results show a tendency of ischiofemoral impingement to develop in patients with coxa valga ,
more frequently in women and in dysplastic hips.
3.1.
Women and IFI:
Of the 10 patients with positive results for IFI,
eight were young women (80%) and there were only two men (20%),
which suggests that women may be more prone to impingement because of the wider positioning of the ischial tuberosities in the female pelvis.
3.2.
IFI and coxa valga:
The neck-shaft angle was measured and the 10 patients (100%) had an enlarged angle corresponding to coxa valga.
Fig. 3 and Fig. 4 .
3.3.
IFI and dysplasia:
Hip dysplasia is not uncommon in adults,
and can vary from subtle acetabular dysplasia to complex sequelae of developmental dysplasia of the hip.
Dysplasia in adults is caused by a non resolved dysplasia from childhood or due to hormonal or mechanical factors.
Bone and soft tissues are assumed to be normal and they are submitted to chronic forces that exceed their level of tolerance causing bone deformation and articular soft tissue changes that lead to articular degeneration.
The femoral head is displaced ventrolaterally causing instability of the hip and adopting an exaggerated valgus position that contributes to IFS narrowing.
Five of our patients had a dysplastic-kind hip (50%), of which only one corresponded to a true dysplasia Fig. 5 with a Wiberg angle < 25º (6º) and the other 4 corresponded to minor dysplasia or instabilities.
These instabilities can be classified according to the measurement of the other angles,
AASA and PASA,
as instability of the anterior column,
the posterior column,
or both.
In our patients,
two had affection of both columns,
one had a posterior instability and one an anterior instability.
3.4.
IFI and FAI:
Femoroacetabular impingement or FAI is a condition of too much friction in the hip joint causing damage to the articular cartilage or the labral cartilage.
FAI generally occurs as two forms: Cam and Pincer. The Cam form describes the femoral head and neck relationship as aspherical,
the Pincer form describes the situation where the acetabulum has too much coverage of the femoral head.
Most of the time they coexist.
In our results,
there was one case of IFI associated with FAI type PINCER due to acetabular retroversion.
It corresponded to a young athlete man Fig. 6 .
3.5.
Pure IFI:
Of the 10 patients with IFI,
only 4 (40%) had a non dysplastic hip and no findings of FAI.
4.
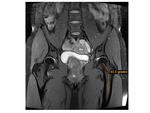
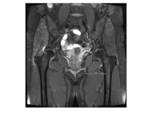
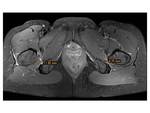
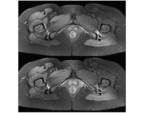
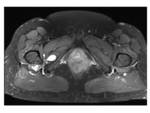
MRI signs:
Bilateral involvement was found in 8 cases (80%),
more often with asymmetrical findings.
Fig. 7
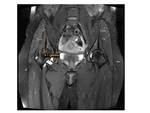
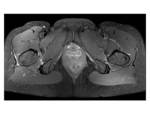
1.
Narrowing of the ischiofemoral space varied from 5mm to 1.5cm and severe clinical symptoms were not related to narrower spaces.
All spaces were measured on an axial plane,
T1 or T2 W.
Fig. 8
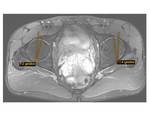
2.
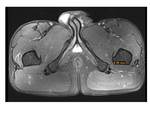
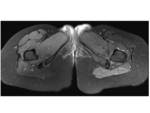
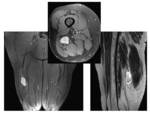
Changes in the quadratus femoris muscle were seen in 9 cases,
from edema (most frequently) to fibrilar ruptures. The narrowing of the IFS can compress the muscle causing edema,
inflammation and fatty replacement.
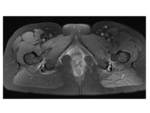
Edema was seen as focal edema in the region of the muscle at the narrowest point of the IFS Fig. 9 and also as diffuse edema extending outside the muscle Fig. 10 . These changes in the QFM can also cause a narrowing of IFS and QFS due to enlargement of the muscle.
Fibrilar ruptures were described in five cases Fig. 11
When radiologists find changes in QFM,
narrowing of the IFS should be studied.
All our cases were acute onsets so no fatty infiltration was seen.
3.
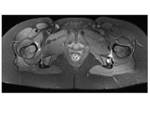
Hamstring tendon changes were described in 4 cases as enlarged tendons or fluid surrounding tendons due to inflammation,
contributing to the narrowing of the QFS.
Fig. 12 Fig. 13
4.
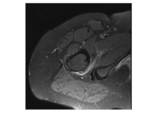
Involvement of other structures can also be found: for example,
the inflammation can extend further and affect the iliac psoas muscle,
the external obturator muscle or the sciatic nerve.
The iliac psoas muscle was involved in three cases Fig. 14 ,
the external obturator muscle Fig. 15 Fig. 16 was affected in two cases and we had one case of sciatic nerve affection Fig. 17
5.
Incidental findings:
Incidental findings such as one case of trochanteritis and one case of schwannoma of the sciatic nerve Fig. 18 were found in patients with positive results for IFI.
6.
Treatment:
Optimal treatment in these patients remains unclear1.
Usually,
conservative treatment is the rule,
with either oral drugs, such as nonsteroidal antiinflamatory,
or echo-guided instillations to reduce pain.
Physiotherapy is recommended.
Recently,
surgery is beginning to have a role in these cases4,
with resection of the lesser trochanter that widens the ischiofemoral space,
which appears to obtain positive clinical results and partial relief of symptoms.
Fig. 19