CF is one of the most common fatal genetic diseases in Caucasians,
affecting approximately 1 in every 2000-4000 children born yearly.
It is an autosomal recessive disorder and it is estimated that 1/25 people are carriers of the defective gene.
The CF gene and its product,
the CF transmembrana conductance regulator (CFTR),
cause abnormal chloride ion transport on the apical surface of exocrine gland epithelial cells.
This results in abnormally thickened,
viscous secretions,
which affect multiple organ systems (lungs,
pancreas,
intestine,
liver…).
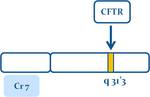
Over 1500 different mutations have been identified at this CF gene,
located on the long arm of chromosome (7q31-q32) Fig. 1 .
The most frequent mutation,
which occurs in 70% of cases,
is a three base-pare deletion called DF508 mutation Fig. 2,
which leads to the loss of a single phenylalanine in the protein.
Two types of clinical presentation can be distinguish Fig. 3:
- The classic or typical CF is the most common (80-90%).
The CF transmembrane conductance protein is nonfunctional and this will affect multiple organ and systems (lung,
pancreas,
sinuses,
liver,
intestine...).
- The nonclassic or atypical CF is characterized by a decrease in protein function but not complete loss thereof.
The affected organ is the pancreas and it is characterized by recurrent episodes of pancreatitis.
Recurrent sinusitis episodes are also common in this group.
Twenty years ago,
up to 70% of patients with CF died before their first birthday,
usually associated with digestive or respiratory complications.
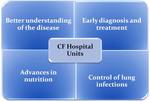
Recent advances in the clinical management of CF have had a significant impact on patients life and today the median life expectancy is around 40 years.
This fact is due to better understanding of the disease,
an early diagnosis and treatment,
advances in nutrition and control of lung infections (the leading cause of morbidity and mortality in these patients).
These improvements should be joined to the development of CF Hospital Units,
both in children and in adults,
which takes a multidisciplinary and comprehensive monitoring of these patients Fig. 4.
Because CF is a chronic and multisystem disease,
patients are recurrent candidates to the Hospital Services including the Emergency Services.
Emergent pathology in CF patient can be divided in two main groups:
1. Pulmonary manifestations
One of the most affected organs in CF is the lung,
and pulmonary failure still accounts for more than 95% of deaths.
Children with CF are born with morphologically normal lungs but they will develop respiratory manifestations in the first year of life in 75% of cases (often cataloged as recurrent episodes of bronchiolitis or bronchitis).
Recurrent respiratory infections in early childhood are responsible for structural irreversible damage in the lung parenchyma (mainly bronchiectases).
At a variable age these patients will develop obstructive pulmonary dysfunction and in the final stages of the disease they develop pulmonary hypertension,
making the lung transplantation the unique option of treatment.
The radiological monitoring of these patients,
as recommended by the clinical guidelines is done as follows:
- Chest radiograph at the diagnosis and after any episode of pulmonary exacerbation.
- High resolution lung CT (HRCT) at diagnosis and then 1 time / year.
CT is the imaging modality of choice to identify and quantify the lung structural disease.
Many early structural changes are seen in the CT even before spirometric changes.
The most common cause for which CF patients come to the emergency room (ER) are respiratory exacerbations,
which are usually caused by S aureus,
H influenzae and P aeruginosa.
Clinically they are characterized by increased cough and dyspnea,
change in the quantity and quality of sputum,
increased sense of fatigue and decreased in regular physical activity.
The early diagnosis and treatment of these episodes are essential to prevent progressive destruction of lung parenchyma and try to restore patients to the basal status previous to the infectious process.
The imaging test for a respiratory exacerbation episode is always a chest radiograph,
which is usually sufficient for diagnosis.
The use of CT is reserved for patients who have atypical respiratory symptoms or those who do not respond to medical treatment.
Radiologists should be familiar with the typical findings of CF and those that arise as a result of an acute episode.
Whenever possible,
it is advisable to compare the current radiograph with previous,
which will give us information of the evolutionary state of the disease and the variations since last study.
- Radiological findings in a CF patient
100% of patients with CF have lung involvement. Findings on chest radiograph depend on the stage of the disease and the degree of parenchyma destruction.
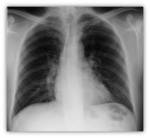
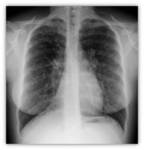
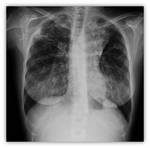
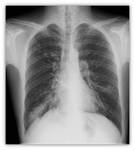
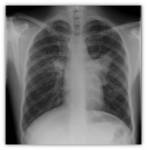
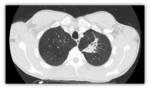
- Chest X-ray: It may be normal in early stages Fig. 5 or may show nonspecific linear images in the lower lobes.
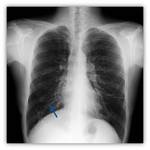
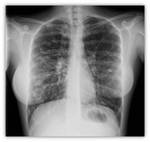
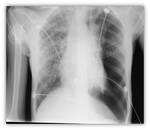
As the disease progresses,
thickening of these linear images and even tubular lesions with the appearance of "rail station",
characteristic of cylindrical bronchiectasis Fig. 6 are identified.
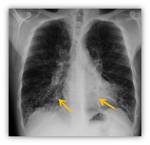
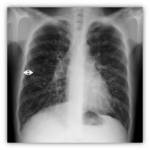
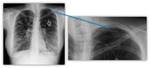
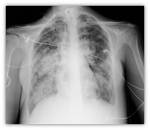
In advanced stages saccular bronchiectasis as annular images in both lungs,
sometimes full of mucous or fluid levels inside Fig. 7 Fig. 8 Fig. 9 are found.
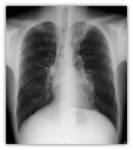
Others common findings are hyperinflation areas and oligohemia in the periphery of the lung due to reducing pulmonary arterial perfusion Fig. 10.
In late stages of the disease are frequent retractions by fibrous scarring,
loss of volume and an important parenchymal destruction Fig. 11.
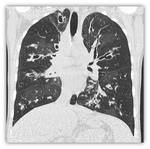
- High resolution lung CT: numerous radiological studies have reported the diagnostic superiority of CT over chest radiograph for the pulmonary involvement in CF.
The most frequently morphologic CT findings are bronchiectasis,
peribronchial wall thickening,
mosaic perfusion,
mucous plugging,
air trapping and parenchymal opacities.
The most typical finding of this disease are bronchiectasis.
The classification of Lynne
Reid that divided them into the following groups:
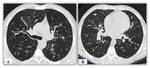
a) Cylindrical or tubular bronchiectasis: the bronchi have regular contours,
uniform diameter and terminating at the periphery.
Inside you can see mucus plugsFig. 12 Fig. 13.
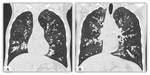
b) Saccular bronchiectasis: It is characterized by the presence of dilated airway with irregular contours like a rosary.
Fluid levels may occur Fig. 14.
c) Varicose bronchiectasis: It is characterized by progressive dilatation to the periphery of the airways,
which end in large cysts,
bags,
or as clusters grapes (this finding is always indicative of the most severe form of bronchiectasis).
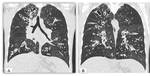
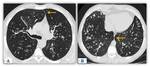
Another typical finding in these patients is the air trapping which is shown in HRCT as patchy areas of higher and lower attenuation,
and that is called "mosaic pattern" Fig. 15.
These density differences between areas are also favored by the vasoconstriction that accompanying the air trapping areas,
where there are not gas exchange and arterial vasoconstriction.
In very advanced disease is often found adhesive atelectasis due to bronchiectasis Fig. 16,
parenchyma retractions,
bullae and diffuse emphysema Fig. 17.
- Radiological findings in the acute episode
During the pulmonary exacerbation episode,
the following radiological findings can be found:
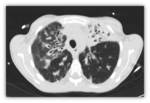
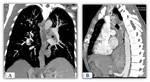
- Consolidations or pulmonary infiltrates,
as areas of increased attenuation with or without air bronchogram Fig. 18 Fig. 19.
Sometimes it is difficult to assess this finding due to the structural damage to the lung parenchyma.
Comparison with previous radiographs of the patient can help.
- Pneumothorax, due to subpleural bullae rupture,
which may occur in up to 19% of CF patients,
especially in adults Fig. 20 Fig. 21.
- Atelectasis,
lobar or segmental,
present between 5-10% of respiratory infections Fig. 22 Fig. 23.
- Hemoptysis.
There are two types,
minor hemoptysis which is common and often accompanies respiratory infection episodes and greater hemoptysis Fig. 24 ,
in which there is bleeding of 240-300 ml/24 h and the patient's life is in danger.
In this last type,
the mortality is very high (85%).
Approximately 1% of patients with CF will have an episode of massive hemoptysis each year.
In these patients,
the realization of an CT angiography of can help locate the affected vessel and planning the treatment Fig. 25 .
2.- Abdominal manifetations
Abdominal pain is one of the most common causes why CF patients consult in the ER.
There are several causes and they are more or less related to the impairment of exocrine pancreatic gland.
When the pancreas destruction is important,
the patient develops pancreatic exocrine insufficiency (up to 85% of CF patients),
there is not enough enzymes to the food digestion,
so malabsorption and steatorrhea will be developed.
This coupled with the CFTR malfunction in intestinal cells that leads to a decrease of the amount of water into the intestinal lumen that facilitates the development of thick feces,
which together with a maldigestion of food,
causes abdominal pain,
food impaction and even may progress to intestinal obstruction.
Today,
thanks to a proper enzyme treatment,
these episodes have decreased in frequency.
The most common causes of abdominal pain are:
a) Esophagitis,
gastritis and peptic ulcer.
The patients with CF usually have gastroesophageal reflux,
It is thought to be due to elevated abdominal pressures from chronic cough,
faeces retention and to long-term use of medications that tend to reduce lower esophageal sphincter pressures.
In a CF patient with epigastric pain and/or vomiting,
esophagitis,
gastritis and gastric or duodenal ulcers must be rule out.
b) Cholecystitis.
Approximately 12-24% of CF patients have cholelithiasis.
It is usually asymptomatic but it can cause episodes of cholecystitis.
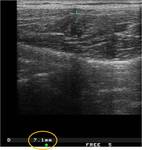
The ultrasound is the indicated imaging technique and the imaging findings are dilated gallbladder,
wall thickening (> 3 mm),
perivesicular edema and Murphy sign.
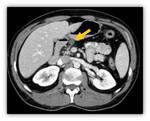
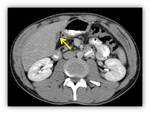
c) Pancreatitis
One of the most frequently organs affected in CF is the pancreas.
Exocrine gland insufficiency affects 85%–90% of all CF patients and is a result of inspissated secretions leading to proximal duct obstruction with subsequent acinar disruption and replacement by fibrous tissue and fat.
Endocrine gland dysfunction is reported in 30%–50% and is thought to result from fibrosis and gland atrophy.
Episodes of recurrent pancreatitis occur frequently in patients who have residual pancreatic exocrine function,
that are more frequent in those patients with atypical or nonclassical disease.
Pancreatitis episodes are less frequent (1%) in patients with typical or classical CF,
because there is greater destruction of the gland,
the exocrine reserve is small and the inflammatory episode is less symptomatic.
These patients develop few post-pancreatitis complications Fig. 26 Fig. 27 .
d) Intestinal Obstruction / Pseudo-obstruction
Distal intestinal obstruction syndrome or meconium ileus equivalent is a well-known complication that occurs in 10-24% of CF.
It is thought to be caused by pancreatic insufficiency,
thickened intestinal secretions,
undigested food remnants and poor motility,
with resultant impaction of mucofeculent material in the distal ileum.
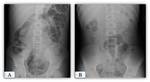
Clinical signs,
symptoms,
and plain radiographic findings can be somewhat nonspecific Fig. 28 .
This complication has decreased in frequency thanks to gastrografin® enemas and an adequate treatment with microsphere pancreatic enzymes.
Other causes that can cause intestinal obstruction in these patients are:
- Intussusception: is found in nearly 20% of CF patients with obstruction Fig. 29 .
It is most frequently ileocolic and is related to an inspissated fecal mass that acts as a lead point.
It may occur as a complication of distal intestinal obstruction syndrome.
- Intestinal volvulus: it is most frequent in infants,
although it can also develop at adulthood.
Generally an intestinal loop containing thick faeces,
tilts and twists its mesentery.
The CT finding of a dilated closed loop and the swirl sign is the key.
- Fibrosing colonopathy: this entity was first described in 1994.
It is characterized by a thickening of the wall of the cecum and ascending colon,
which alters its motility and can cause intestinal obstruction.
It is thought to be related to high-strength pancreatic enzyme replacement (lipase > 20,000 IU / kg / day),
previous episodes of meconium ileus,
impaction food and abuse of NSAIDs.
e) Pseudomembranous colitis
Although half of CF patients are carriers of Clostridium difficile and they often taking antibiotics for exacerbation respiratory episodes,
they infrequently develop pseudomembranous colitis episodes.
CT findings that suggest this entity,
should be communicated to the clinician to confirm or role out it and can treat it correctly Fig. 30 .
f) Acute apendicitis
The frequency of appendicitis in CF is lower than in the general population and its diagnosis is usually more complex due to the following factors
- These patients often have recurrent abdominal pain,
so an episode of appendicitis can be interpreted as one of those unspecific abdominal pain episodes.
- They often take antibiotic treatments for respiratory infections,
which could mask an appendiceal inflammation.
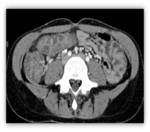
- In these patients normal appendix with a diameter > 6 mm can be found,
due to the mucus accumulation and dilatation of his lumen Fig. 31 .
This must be taken into account when diagnosing a patient with CF of appendicitis,
and look for other imaging clinical and laboratory findings to the diagnostic support.
g) Upper gastrointestinal bleeding
Up to 40% of CF patients develop liver disease,
but only 1% reaches stages evolved with liver cirrhosis and collateral circulation.
When this happens,
variceal bleeding can occur and may be a complaint of these patients to the emergency department.
Management and treatment is similar to the rest of the population.
OTHER FINDINGS:
It is important to know the typical imaging findings of patients with CF,
for a proper interpretation of the images.
In addition to the above,
must remember that in these patients are frequent the following findings:
- Sinuses occupation. Most CF patients have recurrent sinus pathology.
During childhood can present symptoms of nasal obstruction,
snoring or purulent rhinorrhea,
whereas in adolescents and adults are more frequent headaches.
Treatment is symptomatic.
- Collapsed gallbladder Fig. 32 .
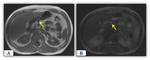
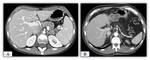
- Liver steatosis Fig. 33 Up to 60% of autopsies of patients with CF and up to 50% of imaging tests (US,
CT,
MRI) show fatty infiltration of the liver.
- Fatty infiltration of the pancreas. Fatty replacement of the pancreas is a typical finding Fig. 34.
When the entire gland is replaced it is called Lipomatous pseudohypertrophy of the pancreas.
- Pancreatic cysts and calcifications.
Calcifications are up by 7%.
The cysts are usually small and isolated Fig. 35,
although it may develop cystic degeneration of the gland that it is known as Pancreatic cistosis.
- Redundancy of the colonic wall. It usually occurs in patients with rare mutations and is characterized by redundancy and folding of the inner layers of the colon (ascending and transverse colon) that can give an image similar to intussusception.
- Nephrolithiasis. Although the kidney is an organ little affected by this disease,
nephrolithiasis can be found in up to 6% of patients with CF.