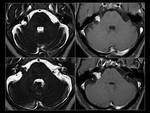
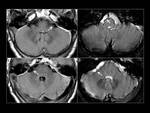
Classification of Disorders Causing Ataxia in Adults
Cerebellar Ataxia:
Cerebellar ataxia is the result of disorder affecting the cerebellum,
or its afferent or efferent tracts.
- Long Duration or Gradually Progressive Cerebellar Ataxia:
Chronic ataxia is the largest group and includes ataxia associated with intracranial mass lesions,
paraneoplastic syndromes,
congenital and hereditary disorders,
multiple sclerosis,
idiopathic degenerative processes,
nutritional deficiencies,
toxins and drugs.
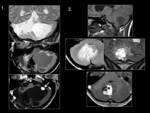
- Mass lesions: (Fig 8 - 12)
The exclusion of posterior fossa masses is usually one of the first steps in chronic cerebellar ataxia evaluation.
In adults,
the most common posterior cranial fossa masses associated to cerebellar ataxia (affecting cerebellar parenchyma or brainstem) are metastases,
hemangioblastomas,
medulloblastomas,
and infiltranting astrocytic tumor of brainstem (Astrocytoma and Glioblastoma).
Large extra axial masses as meningiomas or epidermoid cysts can be a cause of ataxia by compressive effect in cerebellar or brainstem parenchyma.
Frontal lobe and thalamic masses can also present with cerebellar ataxia.
- Paraneoplastic Cerebellar Degeneration
Paraneoplastic cerebellar degeneration usually presents with subacute ataxia.
It can occur with any tumor but is most frequent in breast,
gynecologic and lung tumors and in association with Hodgkin’s disease.
It is caused by antineuronal antibodies.
- Congenital Disorders: (Fig.
13)
The most common congenital disorders that can cause ataxia include Dandy Walker syndrome,
Joubert syndrome and Rhombencephalosynapsis. These disorders usually manifest during early childhood,
but these patients can reach adult age.
- Hereditary Disorders associated to ataxia:
Although genetic testing is mandatory for hereditary ataxias; family history,
physical examination and MRI findings help in the diagnosis.
Hereditary ataxias are a clinically and genetically heterogeneous group of disorders transmitted as autosomal dominant or autosomal recessive traits.
Autosomal dominant spinocerebellar ataxias (AD - SCA) are the largest group of hereditary disorders associated to ataxia.
Spinocerebellar ataxias involve not only the cerebellum,
but also the spinocerebellar tracts of the spinal cord.
(Fig.
14)
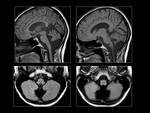
Other hereditary ataxias include dentorubral-pallidoluysian atrophy and autosomal recessive spinocerebellar ataxias as Friedreich’s ataxia (which causes a “mixed” sensory/cerebellar ataxia with predominance of sensory ataxia) and ataxia – telangiectasia syndrome (also causes a “mixed” sensory/cerebellar ataxia but with predominance of the latter).
In Friedreich’s ataxia the major pathological findings are cell loss in the dentate nucleus,
and combined degeneration of the spinocerebellar tracts,
pyramidal tracts and posterior columns.
The disease usually becomes clinically presents in the second decade of life; initially with signs of posterior column degeneration followed by spasticity and cerebellar signs.
Typical findings on physical examination include,
progressive sensorial ataxia with impaired proprioception; and in advanced stages of the disease,
cerebellar ataxia and dysarthria.
(Fig.15)
In adults,
this group is almost exclusively represented by multiple sclerosis.
It typically presents as chronic or subacute cerebellar ataxia,
especially at a young age.
A relapsing-remitting course and the presence of multiple demyelinating lesions in the brain and/or spine on MRI,
suggest the diagnosis.
Multiple sclerosis may cause cerebellar ataxia when it affects the cerebellum,
or its afferent or efferent pathways,
including supratentorial,
brainstem or spinal cord levels or causes sensorial ataxia when it affects the conscious proprioceptive pathway.
(Fig.
16)
- Degenerative Processes: this group includes:
- “Idiopathic late - onset cerebellar ataxia” or ILOCA,
which is a disorder that affects adult patients and produces predominantly,
cerebellar symptomatology,
in the absence of family history and an identified genetic marker.
- Multiple System Atrophy (MSA),
which is a sporadic progressive neurodegenerative disorder of adult onset,
that usually presents after the fifth decade of life as a combination of cerebellar,
pyramidal,
extrapyramidal and autonomic alterations.
Parkinsonian features predominate in 80% of patients (MSA-P subtype) whereas cerebellar symptoms,
with gait and limb ataxia,
dysarthria and cerebellar oculomotor disturbance,
predominate in 20% of patients (MSA-C subtype).
Autonomic symptoms and cognitive dysfunction are frequent.
(Fig.
17)
- Subcortical arteriosclerotic encephalopathy,
which is associated with hypertension,
and shows diffuse and confluent regions of periventricular white matter involvement (leukoariosis).
- Nutritional Deficiency,
Toxins and Drugs:
This group includes exposure to toxins,
as solvents and methylmercury; and to different drugs,
especially some anxiolytic and anticonvulsant medications.
(Fig.
18)
Central pontine myelinolisis can be a cause of ataxia in chronic alcoholics or malnourished patients following rapid correction of hyponatremia; although,
it most frequently presents with coma,
locked-in syndrome or quadriplegia.
(Fig.
19)
Chronic alcoholism can cause ataxia in three different ways: by neurotoxicity of ethanol and its metabolic products (Fig.
20),
by associated chronic liver disease,
or by thiamine deficiency (Wernicke encephalopathy).
- Late Postsurgical or Posttraumatic changes:
Gliosis and malacic changes in cerebellar as well as in afferent and efferent cerebellar tracts can be a cause of long duration ataxia.
(Fig.
21)
- Acute Cerebellar Ataxia as a Possible Manifestation of Stroke: (Fig.
22 and 23)
Hemorrhage or infarction resulting in ataxia can occur in the cerebellum,
lateral portion of the medulla or pons,
mesencephalon,
red or thalamic nuclei,
posterior limb of the internal capsule,
or frontal or parietal cortex.
Wallenberg or lateral medullary syndrome is secondary to infarction in the posterior inferior cerebellar artery (PICA) territory,
and is associated with ipsilateral hemiataxia.
Ischemic causes include lacunar,
cardioembolic,
or atherothrombotic infarcts,
and venous thrombosis.
Hemorrhagic causes that should be considered are hypertensive hemorrhagic stroke in the first place,
but also vascular malformations and venous thrombosis.
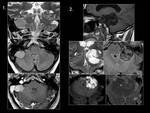
- Acute Cerebellar Ataxia as a Possible Manifestation of Infection: (Fig.
24 and 25)
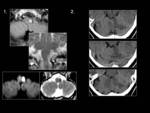
Among the most important infectious causes of ataxia are bacterial cerebellitis,
cerebellar abscess and prion-associated encephalopathies as Creutzfeldt-Jakob disease.
Among parainfectious disorders are acute cerebellitis,
which is more common in children but can also be seen in adults; and Miller-Fisher syndrome,
which is a variant of Guillain-Barré syndrome that causes cerebellar ataxia and opthalmoplegia.
- Acute Cerebellar Ataxia following head Trauma:
Traumatic injuries to the cerebellum,
brainstem or frontal lobe,
producing interruption of the frontopontocerebellar tract can produce ataxia.
Sensorial Ataxia:
Disorders that damage the conscious proprioceptive pathway result in sensorial ataxia,
which usually presents as long duration or gradually progressive ataxia.
Among the main causes of sensorial ataxia are: multiple sclerosis (with affectation of posterior spinal columns or the medial lemniscus in the brainstem) (Fig.
16),
vitamin B12 deficiency (which leads to subacute combined degeneration of spinal cord with demyelination of the posterior columns,
posterior roots,
and pyramidal tracts of spinal cord),
vitamin E deficiency,
Friedreich’s ataxia (Fig.
15),
neurosyphilis (tabes dorsal which affects the lumbosacral dorsal columns and spinal nerve roots) and sensory polyneuropathies (diabetes mellitus,
alcohol consumption)
Vestibular ataxia:
Vestibular ataxia can be caused by any focal lesion that affects the vestibular system including the vestibular areas of the cerebral cortex.
Vestibular ataxia can be caused by injuries to the vestibular nuclei in the brainstem or the VIII cranial nerve,
either in the cerebellopontine angle or the internal auditory canal. Disorders affecting the vestibular nuclei include: tumors and ischemic or hemorrhagic strokes (Fig.
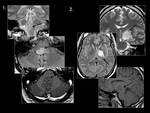
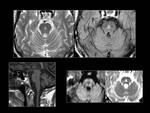
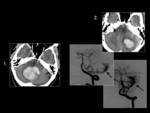
11 and 22); while cranial nerve damage can be produced by tumors (meningiomas and schwannomas) (Fig.
26),
superficial siderosis (Fig.
27) or less frequently by meningeal carcinomatosis. Trauma with damage of vestibular structures can cause vestibular ataxia.
Other causes of acute vestibular ataxia are labyrinthitis,
vestibular neuronitis,
labyrinthine infarction and perilymph fistula,
all them of clinical diagnosis.

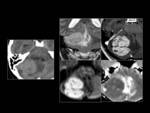
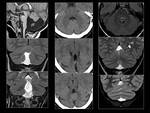
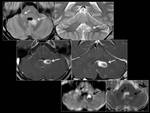
![Fig. 25: Spontaneus Creutzfeldt-]akob disease.
86 years old female with gait ataxia and rapidly progressive dementia.
MRI demonstrates a diffuse cerebral volume loss on sagittal T1WI (left top). Axial FLAIR image (left bottom) shows a bilateral symmetrical hyperintensity in heads of caudate nuclei, pulvinar nuclei ("Pulvinar" sign) and putamens. These hyperintense areas show restricted diffusion: low ADC (middle) and high signal intensity on DWI (right column).](https://epos.myesr.org/posterimage/esr/ecr2013/115891/media/489371?maxheight=150&maxwidth=150)