I.
INTRODUCTION
The meninges that envelop the brain consist in three layers: the dura mater,
the arachnoid mater and the pia mater.
The outermost layer is the dura mater or pachymeninx which lies closest to the calvaria.
Epidural space is a potential space between the outer layer of the dura mater and the inner layer of the skull.
The middle element of the meninges is the arachnoid mater that is attached to the overlying dura mater with a virtual space between both layers,
the subdural space.
The innermost meningeal covering is the pia mater that firmly adheres to the surface of the brain.
Arachnoid mater and pia mater form the leptomeninx and the space between these two layers is the subarachnoid space,
which is filled with cerebrospinal fluid.
- Features normal behaviour of the meninges
The blood vessels within the dura mater lack of vessel unions,
so they do not produce a blood-brain barrier in contrast to arachnoid vessels which are components of the blood-brain barrier.
Because of this,
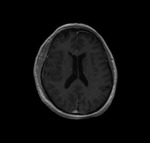
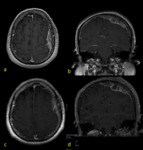
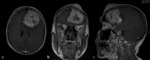
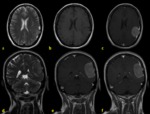
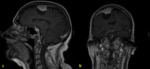
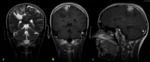
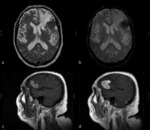
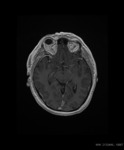
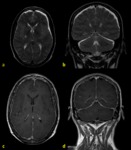
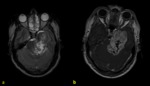
normal dural enhancement is seen clearly on MR images with the following features:
- Thin,
smooth,
discontinuous and symmetric,
- Less strong than the enhancement of the venous sinuses,
- More prominent in the dural reflections of the falx cerebri,
tentorium cerebelli and falx cerebelli.
Fig. 1
II.
IMAGING PROTOCOL or MR TECHNIQUES
Magnetic resonance (MR) is the technique of choice in the diagnosis of the meningeal pathology.
MR is a very reliable tool to determine the extension of the disease and also the associated findings that could be useful to establish the differential diagnosis.
The MR imaging protocol for the depiction of meningeal disease,
in addition to the brain conventional sequences,
should include sequences after contrast administration because this increases the sensibility of the examination and the specificity for meningeal alterations.
Supplementary sequences in the study of meningeal lesions.
Some sequences can be performed after contrast administration besides conventional T1 images:
a) FLAIR/T1FLAIR images.
Post-contrast FLAIR images (especially in delayed-enhanced images) have been described as a useful technique for diagnosing meningeal diseases.
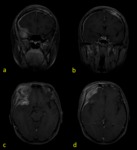
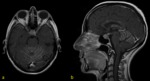
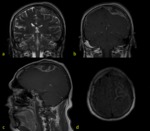
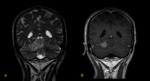
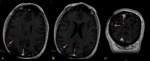
b) Fat suppression sequences (T1 or FLAIR).
In cases with osseous or soft tissues involvement and also in those cases in which the pathology is localized within a region that contains a lot of osseous structures (skull base…).
Fig. 2
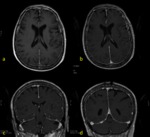
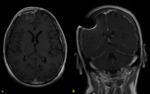
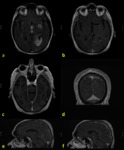
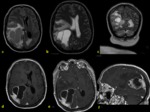
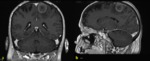
c) T1-3D sequences detect and define in a better way the meningeal enhancement and its features (nodular…) and also provide the opportunity of making multiplanar reconstructions.
Fig. 3 .
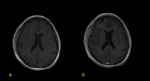
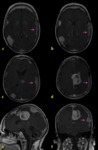
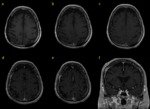
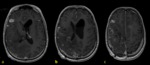
These sequences have some limitations because they tend to overvalue the physiological dural enhancement and,
occasionally,
they don´t stand out the leptomeningeal enhancement.
So,
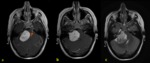
it is always mandatory to perform the conventional T1 image.
Fig. 4 Fig. 5
III.
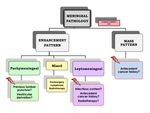
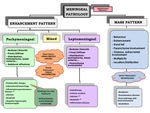
AFFECTED PATTERNS IN MR
Meningeal disease in MR can be classified in two groups: presence of enhancement or mass.
a) The “enhancing pattern”: can be pachymeningeal or leptomeningeal.
- Pachymeningeal: dural enhancement that is adjacent to the inner table of the skull,
interhemispheric fissure and tentorium cerebelli.
This pattern does not draw sulci and basal cisterns and it can be diffuse or focal,
lineal or nodular. Fig. 3
- Leptomeningeal: contrast enhancement follows the subarachnoid spaces of sulci and cisterns. Fig. 6
- Please note: It is important to keep in mind that meningeal enhancement distribution does not purely differentiate dural from leptomeningeal involvement because both layers are closely related.
Therefore the presence of pachymeningeal pattern doesn´t imply that leptomeningeal covering is respected.
b) The “mass pattern”: requires a detailed internal behaviour description and if there is bone or parenchymal involvement,
dural tail and multiplicity of lesions.
IV.
MENINGEAL PATHOLOGY
The most frequent causes of abnormal meningeal enhancement are postoperative changes,
meningeal fibrosis following subarachnoid haemorrhage,
infectious pathology and neoplasms.
1.
Postoperative changes
2.
Tumoral pathology
3.
Infectious pathology
4.
Inflammatory /granulomatous pathology
5.
Intracranial hypotension syndrome
6.
Idiopathic hypertrophy pachymeningitis
7.
Miscellany
1.
Postoperative changes: transient focal pachymeningeal enhancement is seen in the majority of patients undergoing a cranial surgery.
This enhancement can also be diffuse,
patchy and mixed (with associated leptomeningeal component). Fig. 7
2.
Tumoral pathology
a) Meningioma is the most common non-glial primary cerebral neoplasm.
It can adopt “mass” shape (the more typical one) or “en plaque” shape.
In the last one type there is an extensive dural thickening with sessile appearance and can infiltrate the adjacent bone. Fig. 8
Three categories are described (WHO): typical meningioma,
atypical and anaplastic. Fig. 9
Typical meningioma features: Fig. 10
- well defined mass,
- homogeneus signal and enhancement
- dural tail (60%): this finding suggests meningioma but it is not pathognomonic,
- calcification foci,
necrosis and haemorrhage can be present as well as xanthomatous and cystic changes (10-15%). Fig. 11
- supratentorial location (90%)
- associated peritumoral edema (50%)
- osseous destruction can be present but the most common associated osseou change is hyperostosis.
Meningiomas can infiltrate adjacent bone and present extracranial component. Fig. 9
In about 1-9% of the cases multiple meningiomas are seen (16% in postmortem studies).
It is related to the antecedent of radiotherapy.
Fig. 8 .
Multiple meningiomas are different from meningiomatosis which is a manifestation of the type 2 neurofibromatosis.
It is important to remember that,
despite meningioma can have atypical presentation,
it is the most frequent meningeal tumor.
b) Other neoplasms that can originate from the meninges are: mesenchymal and osteocartilaginous tumors,
primary pigmented lesions,
hemangiopericytoma… Fig. 12
Meningeal covering can be affected for a wide variety of pigmented lesions of the CNS.
They can be circumscribed or diffuse and their imaging appeaerance depends on the amount of melanin and the presence of haemorrhage.
They include:
- primary pigmented lesions of the CNS,
- metastatic melanoma, Fig. 13
- other CNS tumors than can show melanin trasformation including shwannoma,
medulloblastoma and some gliomas.
Primary melanocytic neoplasms are rare lesions arising from normally ocurring leptomeningeal melanocytes.
They include: diffuse melanocytosis,
meningeal melanomatosis (in neurocutaneous melanosis),
melanocytoma and malignant melanoma.
When a pigmented lesion is discovered it´s essential to look for a primary pigmented tumor outside the CNS.
The features of these neoplasms overlap because they can show diffuse leptomeningeal proliferation or little focal masses can be present.
They can also have different signal intensity so frequently they cannot be distinguished from meningiomas or other neoplastic or infectious lesions.
c) Metastatic lesions
- Oncohematologic diseases
- Osseous lesions with dural involvement
- Meningeal metastases
- Oncohematologic diseases. Leucemic or linfomatous cells can affect the skull diploe,
the dura mater,
the leptomeninges or all of them.
They can have a focal or diffuse appearance. Fig. 14
Primary leukemia of the CNS is extremely rare and it normally shows some masses with enhancement and dural base.
Secundary lymphoma usually has extraaxial location and can be epidural,
subdural,
subarachonid or a combination of all of them. Fig. 15
In these patients,
infectious processes and chemical meningitis can also occur and their manifestations can be similar to the tumoral disease so the cytological exam of the cerebrospinal fluid is indispensable.
- Cranial osseous metastases.
They are relatively common and secondarily they can infiltrate the adjacent dura mater and brain parenchyma.
Fig. 2 Fig. 16
- Meningeal metastases. The most frequent tumors metastasizing to the meninges are breast and lung cancerm lymphoma-leukemia and malignant melanoma.
Primary tumors of the CNS (medulloblastoma,
PNET,
ependymoma,
germinal cells tumor,
astrocytoma and glioblastoma ) show afinity for the meninges.
Dural metastases have similar spectrum of presentation than meningiomas and they can also have dural tail.
Fig. 17 Fig. 18 Fig. 19
Meningeal carcinomatosis can affect the dura matter,
leptomeninges or both.
Leptomeningeal involvement is expressed as thin lines or small nodules with enhancement extending along the cortical surface.
Fig. 20 Pachymeningeal carcinomatosis is a rare type of metastatic intracraneal disease.
The dura mater appears diffusely thickened as a membrane with nodular aspecto that covers the brain but not the adjacent subarachnoid space.
The presence of neoplasm near to the meninges or a small foci of meningeal tumor can produce,
in addition,
a diffuse fibrose response in the adjacent meninx.
Both tumor and fibrosis show enhancement so the specificity of this finding is limited.
3.
Infectious pathology
Infectious pathology generally produces leptomeningeal involvement.
Fungal infections can show nodular thickening and enhancement,
as leptomeningeal carcinomatosis does.
Some infections can associate pachymeningeal enhancement (tuberculosis,
fungus…),
usually with nodular appearance.
Fig. 21
4.
Inflamatory/granulomatous pathology
Churg-Strauss syndrome,
Wegener granulomatosis,
reumatoid artritis,
sarcoidosis… These pathologies are associated to a characteristic clinical context.
They can present CNS involvement with infiltration of meninges that produces dural enhancement with nodules and masses localized in the basal cisterns.
Fig. 22 Fig. 23
5.
Intracranial hypotension syndrome
Loss of cerebrospinal fluid (CSF) pressure that can be idiopathic,
after a lumbar puncture,
CSF fistulae,
postsurgical,
posttraumatic…
The classical clinical syndrome consists in:
- Positional headache,
- Low CSF pressure,
- Pachymeningeal enhancement,
usually diffuse,
with possible associations (subdural effusions,
prominence of venous sinuses,
descent of the brain).
Disappearance of these findings is confirmed in the follow up.
Fig. 24 Fig. 25
Pachymeningeal enhancement after lumbar puncture without complication is normally resolved in 48-72 hours. Fig. 3
6.
Idiopathic hypertrophy pachymeningitis
This pathology is a rare inflammatory fibrossing disease with focal or diffuse thickening of the dura mater.
The most frequent manifestation is headache and it is an exclusion diagnosis.
7.
Miscellany
- Radiotherapy can produce meningeal changes,
normally leptomeningeal enhancement,
although it can be mixed. Fig. 26
- Cerebrovascular accident can associate leptomeningeal enhancement.
- Subarachnoid haemorrhage can be accompanied by pachymeningeal enhancement.
- Hemophagocytic syndrome is a rare childhood disease characterized by histiocytic and lymphocytic infiltration in different organs.
Parenchymal alterations and leptomeningeal enhancement can be present.
- Amiloidosis can originate amilod deposits in the dura mater and simulate meningiomas.
V.
DIAGNOSTIC ALGORITHM Table 1 Table 2
There are some points to keep in mind when elaborating the radiological report
1.
CLINICAL CONTEXT
The clinical context is very important in meningeal pathology and the radiologist must pay attention to the medical history in each patient.
2.
DESCRIPTION OF THE RADIOLOGICAL FINDINGS
- To make a deep and correct description of the findings
- To recognize the presentation pattern and its characteristics
- To describe the associated findings: parenchymal or osseous involvement,
distribution,
location and potential complications
3.
CONCLUSION
It is important to delimit the differential diagnosis following the diagnostic algorithm of the meningeal pathology,
with some considerations:
- When no clinical history of interest is present and pachymeningeal enhancement exits,
this finding is non-specific.
- The first question to ask when pachymeningeal enhancement is present is if it has been performed a previous recent lumbar puncture.
- In the case of an extra-axial mass,
whatever its features,
the most frequent ethiology is meningioma,
taking into consideration that in an oncological context,
dural metastases could show similar manifestations.
- A mass with hyperintensity in T1WI can correspond to a meningioma with previous bleeds or to a pigmented lesion.
- Leptomeningeal nodular enhancement suggests neoplastic or fungal ethiology.
- Infections more frequently produce leptomeningeal pattern.
- The leptomeningeal pattern is caused more commonly by infections than tumors.
- Leptomeningeal metastases are more frequent than pachymeningeal metastases.
- Occasionally superficial tumors with large dural contact can simulate extra-axial masses. Fig. 27
- Meningioma can also infiltrate the adjacent bone and present extra-cranial component.
So in the presence of a lesion with osseous,
dural and extra-cranial components the differential diagnosis will be between dural neoplasm (primary or secondary) and osseous tumor,
being the last the most frequent.
- Shwannomas should be considered in the presence of a mass in the posterior fossa (ponto-cerebellar angle) or in locations where nerves are passing.
Fig. 28 Fig. 29