Ultrasonography (US) is usually the screening method of choice,
particularly useful for detection of cystic membranes,
septa and hydatid sand [6,
17].
Although it may display the majority of the findings of Computed Tomography (CT),
this,
with its high sensitivity (94%),
might be indicated in cases in which US fails due to patient-related difficulties and in the presence of disease complications,
as well as to determine the resectability of the lesions when surgery is indicated [6,
12,
18,
19].
Intravenous administration of contrast material is only necessary when complications are suspected [12].
In very uncertain cases Magnetic Resonance (MR) may be performed to confirm the hypothesis,
being the best imaging procedure to demonstrate a cystic component [20].
Both,
CT and MR might reveal cyst’s rupture,
CT being the best demonstrating complication by bacterial superinfection,
including abscess formation with air-fluid level [12,
14].
Conventional Radiography (CR) only reveals calcified lesions,
20-30% of liver HC being seen [7].
CT and CR are the best modalities for detecting calcification [13].
HC’ radiologic appearance widely varies,
according to their growth stage and whether they are complicated or not.
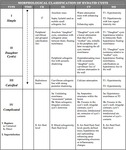
According to their appearance,
they can be classified in four types,
resumed in table 1.
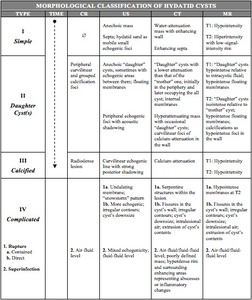
Table 1: Classification of hydatid cysts on the basis of their appearance. Adapted from the classification presented on reference 7, in correlation with the imaging features of our series and those of the other references reviewed.
LIVER
Most hepatic HC are located in the right lobe [6,
7] and frequently presents exophytic growth,
especially in the bare area of the liver and gastrohepatic ligament [6].
Rupture occurs in the majority of the HC (50-90%) due to the degeneration of parasitic membranes mainly as a result of its age,
host defence or chemical reactions,
but also after trauma [6].
Although it can be asymptomatic,
the passage of cystic fluid into the host’s blood circulation may produce anaphylaxis [8,
16].
In contained rupture only the endocyst’s detachment occurs,
seen as floating membranes.
Direct ruptures also involve the pericyst,
allowing free passage of the cyst’s content,
occasionally into the biliary ducts,
peritoneal or pleural cavities,
hollow viscera or abdominal wall.
[6,
15,
16]
Bacterial superinfection of HC is always secondary to rupture,
whether contained or direct,
occurring in up to 25% of cases [6,
7].
Portal vein involvement is very rare,
there being only a few reported cases of compression with secondary thrombosis and cavernous transformation,
caused by cysts located in the caudate lobe and hepatic bifurcation [21,
22].
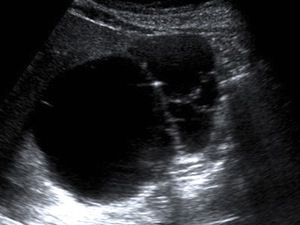
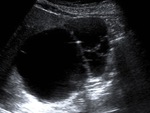
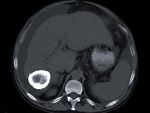
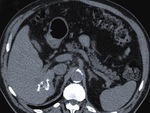
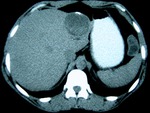
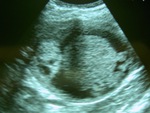
Fig. 1: An 83-year-old woman presented two type I HC in the liver at US scan, the largest one, was an anechoic lesion with a few septa and a calcification focus.
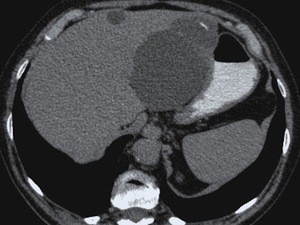
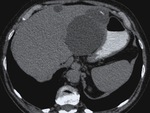
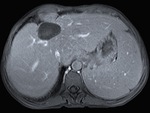
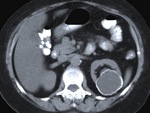
Fig. 2: The same lesion as in figure 1 at contrast-enhanced CT, was low-attenuated with slight enhancement of its wall and septa, the calcification focus also being evident. The smaller cyst on the right, in an earlier stage, was just a low attenuation nodule, indistinguishable from a simple nonparasitic cyst.
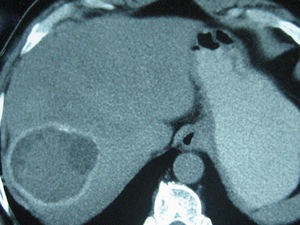
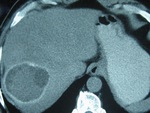
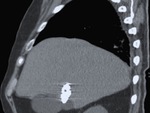
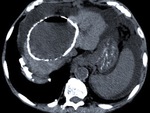
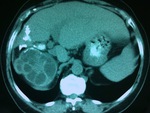
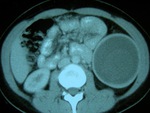
Fig. 3: A type II hepatic HC incidentally found in a 71-year-old asymptomatic man at an unenhanced scan, as a typical water-attenuation lesion with peripheral “daughter” cysts within it, which attenuation was lower than that of the “mother” cyst’s matrix. Note the scattered wall calcifications.
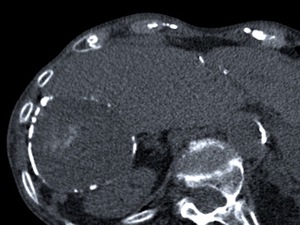
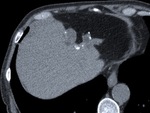
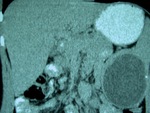
Fig. 4: A large type II HC at an unenhanced CT scan, of higher attenuation than that of the ones previously describe and extensive calcification of its wall, representing the degeneration of an older cyst with amorphous and tenacious content. There were still evident a few floating membranes detached from the endocyst.
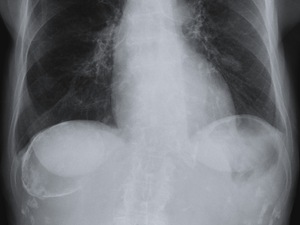
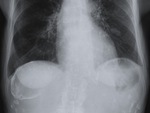
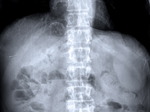
Fig. 5: The same lesion as in figure 4 at CR, showed almost complete calcification of its wall.
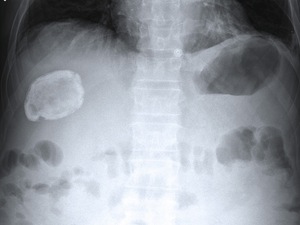
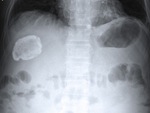
Fig. 6: Round calcified mass in the right hypochondrium detected at abdominal CR corresponding to an old hydatid cyst.
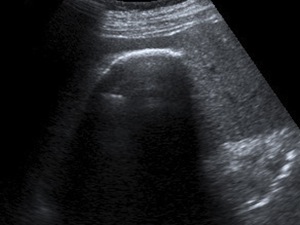
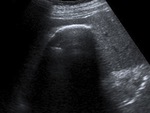
Fig. 7: US scan of the same patient as in figure 6 showed a curvilinear echogenic line with strong posterior shadowing.
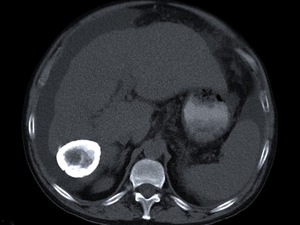
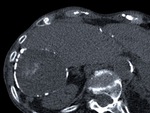
Fig. 8: The same lesion as in figures 6 and 7 at an unenhanced CT scan appeared as an almost completely calcified mass, compatible with a type III HC, which might be assumed to be death. Note the lobulated contours of the liver and ascitis of this 60-year-old man with complicated chronic hepatic disease.
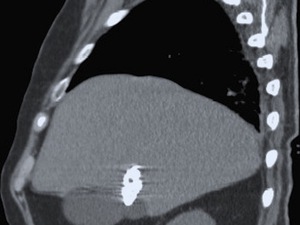
Fig. 9: Another old cyst, totally calcified, at an unenhanced CT scan of an asymptomatic patient with known HD (fig. 9).
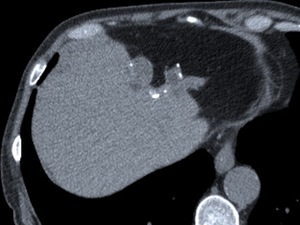
Fig. 10: Type II HC after a direct rupture, probably due to the left hepatectomy noted at this unenhanced CT scan. The lesion appeared partially collapsed with irregularity of its subcapsular contour.
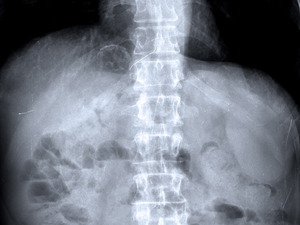
Fig. 11: The same lesion as in figure 10, also evident at CR, due to the extensive calcification of its wall.
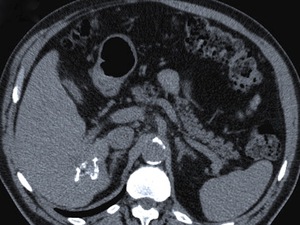
Fig. 12: Later after a direct rupture, HC become collapsed and calcified, as shown at this unenhanced CT scan.
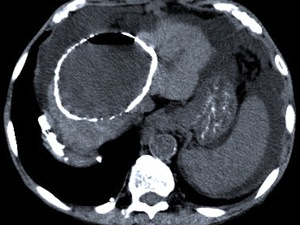
Fig. 13: The unenhanced CT scan of a patient with fever and abdominal pain with a known HD, showed a huge cystic mass with calcified wall and an air-fluid level, suggestive of a complication of bacterial superinfection with abscess formation. Note the lobulated contour of the liver and ascitis due to long-standing hepatic cirrhosis.
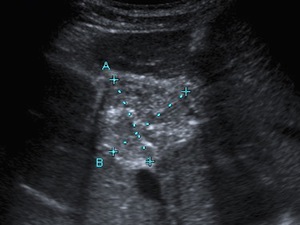
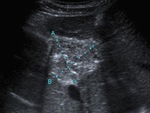
Fig. 14: The abdominal US scan of a 41-year-old woman with hepatic and splenic disease related to Acquired Immunodeficiency Syndrome, with pancytopenia, fever a and pain in the right hypochondrium, revealed an hepatic cystic mass with mixed echogenicity content.
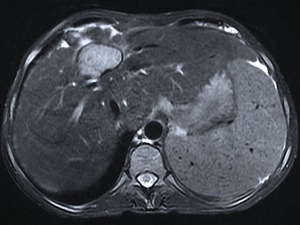
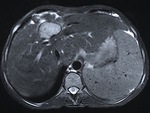
Fig. 15: The same lesion as in figure 14, seen at this T2 weighted MR image was hyperintense and slightly heterogeneous with hypointense signal of its wall, representing its calcification.
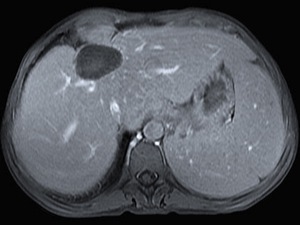
Fig. 16: The same lesion as in figures 14 and 15 at T1 weighted images, presented hypointense content. The findings were suggestive of a superinfection of an HC.
PERITONEUM
Although there are a few cases of primary peritoneal hydatidosis [6],
it is almost always secondary to hepatic disease,
occurring in about 13% of patients with abdominal hydatidosis.
The main etiology is the direct seeding from a ruptured cyst,
mostly after surgery hepatic disease,
but also from spontaneous microruptures.
Cysts are usually multiple and might be located anywhere in the peritoneal cavity,
their imaging features being similar to those of hepatic ones.
[6,
7]
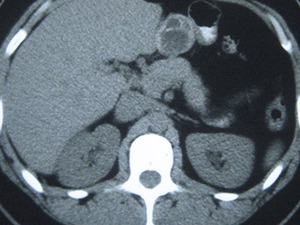
Fig. 17: Hydatid peritoneal seeding in a 34-year-old woman, who underwent a CT scan for persistent pelvic pain. Multiple characteristic type II HC were identified in the peritoneal cavity, including this one in the gastrohepatic ligament.
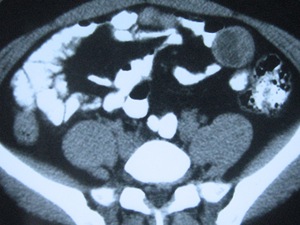
Fig. 18: Mesenteric HC in the same patient as in figure 17.
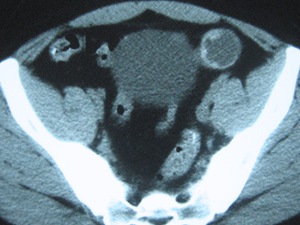
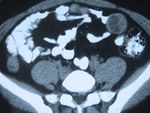
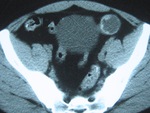
Fig. 19: Type II HC in the left iliac fossa of the same patient as in figures 17 and
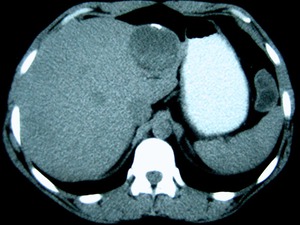
Fig. 20: Type I HC with hyperdense hydatid sand in its dependent portion, detected in the left hepatic lobe of the same patient as in figures 17 to 19, assumed to be the one giving origin to the others.
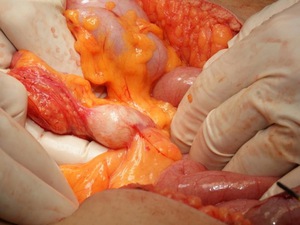
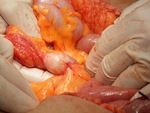
Fig. 21: Intrasurgical photograph of mesenteric HC of the same patient as in figures 17 to 20.
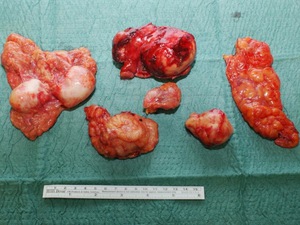
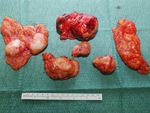
Fig. 22: Photograph of the surgical specimens of the same patient as in figures 17 to 21, confirmed to be HC by pathological examination.
KIDNEYS
Renal involvement rarely occurs,
the reported prevalence being 3%.
Most lesions are solitary,
located in the cortex and frequently asymptomatic until they reach 10 cm,
when they might start causing a flank palpable mass,
pain and dysuria [6,
7,
16].
The differential diagnosis with simple renal cysts and renal cell carcinoma can be made only with percutaneous puncture,
although clinical suspicion should exist in the presence of known concomitant HC in other locations [7].
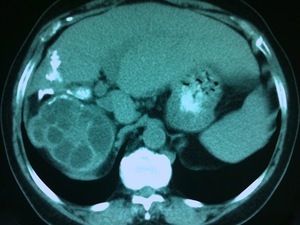
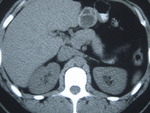
Fig. 23: Renal HC in a 78 year-old woman with long-standing hepatic HD at an unenhanced CT scan, seen as a large multiseptated cystic mass in the right kidney with partial calcification of its wall. An irregular calcified lesion in the right lobe of the liver is also present, corresponding to a collapsed death HC. The patient underwent nephrectomy, the definite diagnosis having being confirmed by pathological examination.
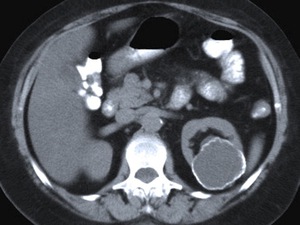
Fig. 24: Primary renal hydatidosis in a 46 year-old woman who presented with left flank pain. The unenhanced CT scan showed a hypoattenuating homogeneous mass with almost complete calcification of its wall, corresponding to an old HC.
SPLEEN
Splenic hydatidosis is rare occurring in 0,9 to 8% of cases,
whether produced by systemic dissemination or intraperitoneal spread from a ruptured hepatic cyst,
primary involvement being extremely uncommon.
They are usually solitary lesions with imaging features similar to those of the ones previously described.
[6,
7]
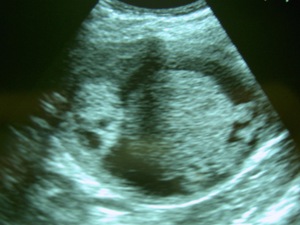
Fig. 25: Primary splenic HC in a 24-year-old woman, who underwent imaging examinations due to pain in the left hypochondrium and a palpable mass. The US scan showed a solitary complex cystic lesion in the spleen, with daughter cysts within it.
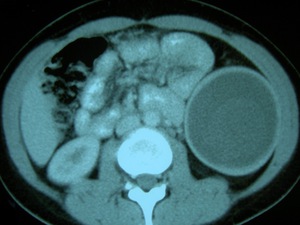
Fig. 26: The same lesion as in figure 25 was also evident at the CT scan corresponding to a type II HC.
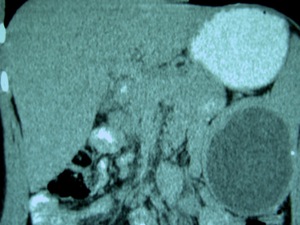
Fig. 27: Coronal CT slice of the same lesion as in figures 25 and 26, showing the incipient calcification of its wall.