The High Dose Rate Brachytherapy in real time program began at the Cruces University Hospital in 2011.
Patients:
The inclusion criteria for this radiotherapy treatment were: having an intermediate or high risk prostate carcinoma,
IPSS (International Prostate Symptom Score) under 15/35,
a prostate volume less than 60 cc,
and organ confined disease or extraglandular extension that can be covered securely with the HDR brachytherapy field.
Extension studies:
A PSA analytical cuantification,
prostate biopsy guided by transrectal ultrasound,
and extension studies with bone scintigraphy,
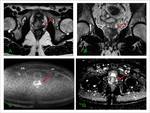
abdomen and pelvis CT and prostate MRI were permormed.
Treatment:
The protocol of our Hospital establishes that patients with intermediate risk are treated with a combination of HDR brachytherapy and external beam radiotherapy (EBRT),
with or without the addition of antiandrogen hormone therapy for 6 months,
depending on the characteristics of the disease.
The high-risk patients receive a dose escalation therapy with HDR brachytherapy and EBRT,
with androgen deprivation therapy for 2 years.
MRI Technique:
Studies were performed using a 1.5 T (Achieva,
Philips Medical Systems) and body multichannel antenna (Cardiac Sense-MS).
The parameters of the sequences had been previously optimized for this coil.
All patients were studied in supine position after intramuscular administration of butyl scopolamine (Buscopan) and after cleansing rectal enema before going to trial.
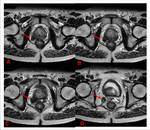
A localizer image was performed in three planes and then T2 Fast Spin with TR / TE 2800/140 msec and echo train of 16,
with a field of view of 23 x 18 cm and a 256 x 176 matrix,
4-mm section thickness and NEX = 3,
including prostate and seminal vesicles.
Subsequently,
axial T1 sequences of the entire pelvis from the iliac crest to pubis symphysis were performed,
with a field of view 25 cm and TR / TE of 619/10 msec,
slice thickness of 4 mm,
NEX = 2; and T2 axial volumetric sequence (VISTA) as a guide for planning brachytherapy.
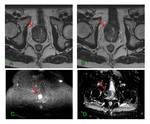
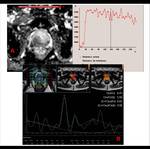
For the functional study,
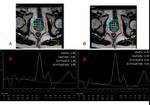
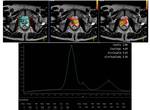
spectroscopy MRI sequences were performed (PRESS),
with three-dimensional imaging of chemical shift and parametric maps (relationship maps choline-creatine/citrato ratio) in correlation with morphologic T2-weighted images.
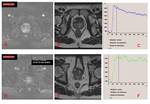
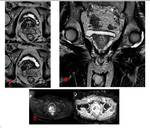
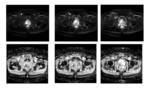
The diffusion sequence,
DWI, was performed using an imaging technique of one echoplanar shot with TR / TE 3112 / 80 milliseconds; FOV 29 cm; slice thickness 4 mm,
0 mm gap; matrix of 156 x 123; NEX = 4,
and b values of 0,
500,
1000 s/mm2.
Prior to the study,
it was established that the b value of 1000 s/mm2 provided the highest image contrast between normal and malignant prostatic tissue in our 1.5-T system.
The ADC values obtained from DWI sequences were made with b values of 0,
500 and 1000 s/mm2 and the ADC maps were generated by calculating the ADC value for each pixel in each cut.
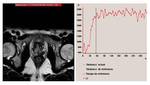
Finally a dynamic FFE T1 volumetric sequence was permormed (TR / TE 4.4 / 2.1,
angle 12 °; slice thickness 4 mm,
gap 0,FOV 23 cm,
matrix 92 x 90,
NEX = 2,
with 20 dynamic phases) in the axial plane.
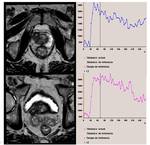
From the resulting image data,
we analyzed the various curves of perfusion to allow detection and localization of the tumor.
All MR studies were evaluated by radiologists involved in uro-radiology.
Data and statistics:
We performed a descriptive analysis using frequency distributions and percentages for qualitative variables,
and the mean or median and standard deviation or interquartile range for continuous variables.
Comparison of proportions between qualitative variables was performed using the Chi-square test or the corresponding corrections,
like Fisher correction when the expected frequencies were <5.
We calculated the OR and confidence intervals using univariate logistic regression.
The comparison between two groups with a continuous variable was performed using a nonparametric analysis Mann-Whitney U depending on distributional characteristics.
The statistical software used was SPSS 20.0 vs.