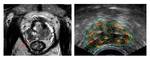
Results:
We have selected 50 consecutive patients with prostate cancer treatment,
candidates to combined HDR brachytherapy and EBRT.
All these patients underwent a pretreatment MRI for local staging.
The median age of patients was 71 years (range 58-78),
median pretreatment PSA 10.15 ng/ml (3.3-66),
the cores obtained median 10 (6-12) and a volume of 35 cc (14-58)
The clinicopathologic characteristics of the patients are presented in Table 1.
The parameters studied in MRI were agreed at uro-oncology tumors committee of our Hospital and were defined as: tumor burden (number of nodules or intraprostatic mass),
laterality of lesions,
the presence or absence of extraglandular tumor extension,
the seminal vesicle invasion,
pelvic lymph node involvement,
and metastatic bone disease in the bone territory.
The distribution of MR predictors in the 50 patients are shown in Table 2.
Of the 50 patients staged with MRI,
35 of them (70%) were overstaged compared with the clinical stage obtained by digital rectal examination (DRE) or transrectal ultrasonography.
Although none of the patients were classified as cT3 (extra-prostatic disease) by transrectal ultrasound or prostate biopsy,
after MRI 23 patients (46%) showed the presence of extraglandular tumor,
cT3b cT3a.
Univariate analysis showed no statistical significance between the risk of extraglandular extension and the remaining studied variables.
This overstaging at the local stadium of patients resulted in changes in the risk group classification.
We have taken into account both risk groups: NCCN [10],
and D’Amico [11].
These results are presented in Table 3.
Changes in risk groups lead to a different therapeutic alternative when a patient undergoes a change from low to intermediate risk and from intermediate to high risk.
This means taking into account the NCCN and D’Amico classification,
that 13 (26%) and 10 (20%) patients respectively,
received a different treatment after performing MRI.
Discussion:
The MRI provides high resolution soft tissue images allowing an appropriate assessment of the local extent of the disease [12].
Recent studies have shown an increase in sensitivity and specificity for the detection of localized prostate cancer when using MRI as a diagnostic tool in the staging of the disease [13].
The extraglandular extension is not a simple binary observation but is rather an important quantitative component.
It is known that the level of extraprostatic extension affects its detection by RM [14]: extraglandular extension >5 mm in the radial diameter awards a poor prognosis in patients receiving radiotherapy [15].
Prostate cancer has a low signal intensity on MRI,
but circumstances like bleeding post biopsy,
prostatitis,
or scar tissue can cause artifacts and the image looks very similar to those of neoplastic lesions.
A meta-analysis of MRI in the local staging of prostate cancer published in 2002 showed a wide range of precision,
from 50% to 92% [16].
This is because of the technology,
the great improvement in the imaging techniques,
and the use of multiparametric MRI.
Turkbey and colleagues from the National Cancer Institute (NCI) in Bethesda,
have shown in a very recent publication positive predictive values for detection of cancer with multiparametric MRI techniques of 98%,
98% and 100%,
in all prostate,
peripheral and central gland respectively [17].
Similarly,
a prospective study with 27 patients demonstrated that multiparametric MRI is significantly more accurate in predicting the final pathological stage than Partin tables [18].
Moreover,
the detection accuracy of the extraglandular extension is much higher when the radiologists are dedicated to Genito-Urinary,
than when they do not [19].
In this study,
the radiologists who reported prostate MRI studies were Urogenital dedicated radiologists.
The gold standard in the 1.5 T MRI for prostate cancer is the use of a body coil with or without endorectal coil.
Recent advances in MRI imaging,
faster sequences,
with coils higher gradients and the post-processing are able to exclude the use of the endorectal coil [20-22].
It has also been postulated that the use of endorectal coil MRI and using 3.0 T MRI would allow a better detection and staging of prostate cancer.
The Cruces University Hospital currently has two MRI scans of 1.5 T.
Although the studies were performed over recent years with a combination of multichannel surface coil and endorectal coil,
endorectal coil is no longer in use for not providing additional information.
In our study,
the impact of MRI in the local disease overstaging has been very striking.
70% of patients suffered an overstaging while 23 patients (46%) of the 50 studied patients increased their local stadium from cT1-T2 to cT3.
There are few studies similar to this one.
In a study published by Clarke et al.
in which 327 patients were staged by MRI prior to radiotherapy treatment,
there was an overstaging of T1-T2 to T3,
also in 70% of patients.
In this study,
most of the overstaged patients were treated different than originally proposed.
They received a combination of low dose rate brachytherapy with iodine 125 seeds and external beam radiotherapy,
not only brachytherapy [23].
Even more important than the local overstaging (cT3a-b),
is its implication in the risk group classification.
In our study,
it has been observed that MRI changed the risk group in 56% of cases when using the classification system of the NCCN,
and in 24% when using the classification system of D’Amico.
Given the NCCN classification,
13 patients (26%) received a different treatment from that originally proposed after performing MRI; and taking into account the classification of D’Amico,
10 patients (20%) changed their treatment from the first originally proposed.
In those cases with extraprostatic extension (stage cT3a) or seminal vesicle infiltration (stage cT3b),
the images were reviewed with the radiotherapist team to confirm the correct coverage of the extraprostatic volume tumor with HDR brachytherapy.
In such situations the number of catheters are increased and the downtime of the 192Ir source in the region corresponding to the area of extraprostatic extension,
to ensure that the coverage for the extraprostatic area with the prescription isodose was suitable,
as shown in figure 15.
Previous studies that have investigated the value of MRI prior to radiotherapy have consistently shown that MRI findings predict biochemical control [15,
24-26].
Nguyen et al.
found that while the presence of seminal vesicle invasion was a prognostic factor,
the existence of extraglandular extension in MRI correlated with an increased risk of biochemical recurrence [26].
However,
Riaz et al,
in the only published study to date about the role of pre-treatment MRI and combination of EBRT and brachytherapy,
showed that the only factors that correlated with biochemical control were the Gleason score and the presence of extraprostatic extension [27].
The two main limitations of our study are the number of patients,
and the lack of final validation of the sensitivity and specificity of the technique with the anatomo-pathology specimen (because these patients are not treated surgically).
However,
the fact that the MRI is reported by uro-radiologists,
and the performing of multiparametric studies with spectroscopic techniques in all patients improve our center’s MRI accuracy.
It is obvious that we must improve the local staging systems for prostatic disease,
and based on the results of our study and others like it,
we think that MRI provides useful information when deciding the appropriate treatment and how to run it.