In human,
hydatid disease involves the liver in approximately 75% of cases,
the lung in 15% and other anatomic locations in 10% (1).
The right lobe in the most frequently involved part of the liver.
Imaging findings in hepatic hydatid disease depend on the stage of the cyst growth:
1.
- PLAIN RADIOGRAPHY:
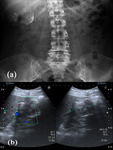
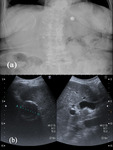
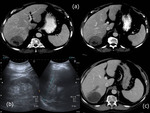
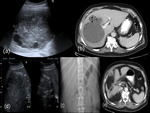
Calcification is seen at radiography in 20-30% (Fig.
2a) of hydatid cysts and usually manifests with a curvilinear or ringlike (Fig.
3a) pattern representing calcification of the pericyst (1).
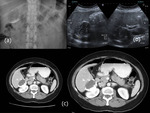
During the natural evolution toward healing,
calcification of all components of cyst occurs (calcification much more coarse and dense)(Fig.
4a).
Therefore,
calcification of pericyst does not indicate necessarily parasite death.
Only when the calcification occurs completely,
tapeworm is death.
2.
- ULTRASOUND
The appearance of hydatid cysts in ultrasound may vary.
Several classifications have been proposed based on the appearance of cysts,
some of the most used are: Classification of hydatid cyst Gharbi in 1981 or WHO classification hydatid cyst lesions,
2003 (World Health Classification Onganization Informal Working Group,
WHO/ IWG).
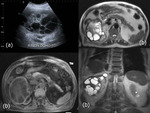
In the early stages hydatid cyst may appear on imaging tests as a simple cyst or cystic lesion,
usually unilocular anechoic content,
wall uniform and clearly visible,
most under 5cm(Fig.
6a,
6d).
In these early stages of development this cyst is not yet fertile (contains no scolex) but its status is active.
There aren't any pathognomonic data in US to distinguish it from other cystic lesions.
In later stages,
the wall of the cyst is usually visible as a double echogenic layer separated by a strip hypoechoic.
Simple cyst shows no internal structure,
but can display multiple echogenic foci due to hydatid sand ("snow flake sign" ).
It can be more evidentif the patient is repostioned the ultrasound examination; moving most dependent area of the cyst ("snowstorm sign").
Detachment of the endocyst from the pericyst is probably related to decreased intracystic pressure,
degeneration,
host response,
trauma or response to therapy (1).The cyst appears as a collection of well defined walls and membranes with multiple floating septa inside or multiseptate multivesicular injury(Fig.
5a,
5b).
Later when the separation of the membranes within the cyst is complete,
the cyst has a content anechoic with laminar membranes that are floating within the cyst ("water lily sign").Ultrasound is the most sensitive test for the detection of membranes,
septa,
and hydatid sand within the cyst.
Multivesicular cysts appears as a collection in a honeycomb pattern(Fig.
10a) with multiple septa which correspond to the walls of the daughter cyst.
Daughter cysts appear as cysts within a cyst.
When daughter cyst are separated from hydatid matrix (mixed echogenicity) they demostrate a âwheel spokeâ pattern (Fig.
7a).
The matrix represents hydatid fluid containing membranes of broken daughter vesicles,
scolices,
and hydatid sand.
Membranes may appear within the matrix as snaking lines,
a finding that is highly specific for hydatid disease.
When the matrix completely fills the cyst has a mixed echogenicity appearance that simulates a solid mass(Fig.
8b).
Since the differentiation of this lesion from other masses or liver abscesses can be difficult,
it is important to find the daughter vesicles or membranes within the lesion which can help us to make a correct diagnosis.
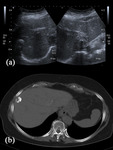
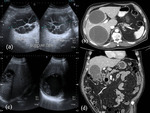
Calcification of the cyst usually occurs in the cyst wall (Fig.
1a),
although internal calcifications may also be seen.
US shows a hyperechoic contour with a cone-shaped acoustic shadow.
When the cyst wall is calcified(Fig.
2b),
in US is visible only the anterior portion thereof,
and appears as a thick arc with a posterior concavity.
The partial calcification does not always indicate the death of the parasite(Fig.
4 b),
but cysts with dense calcification of all components can be assumed to be inactive.
3.
- COMPUTED TOMOGRAPHY
CT is indicated in cases where US fails due to patient-related difficulties (obesity,
excessive intestinal gas,
abdominal wall deformities,
previous surgery) or complicated disease.
CT has a high sensitivity and specificity for hepatic hydatid disease.
The administration of intravenous contrast is not necessary unless complications are suspected.
CT may display the same findings as US (1).
Cyst fluid demonstrates water attenuation (Fig.
4c).
Calcification of the cyst wall or internal septa is easily detected on CT (Fig.
1b).
A typical hydatid cyst wall shows a high attenuation at unenhanced CT even without calcifications.
There is no clear explanation for this finding,
which can also be found in patients with increased attenuation of the liver as hemochromatosis,
drugs such as amiodarone or when administering intravenous contrast.
Detachement of the laminated membrane from the pericyst can be viewed as linear areas of increased attenuation within the cyst.
Daughter cysts structures are displayed as peripherally located attached to mother cyst.
4.
- MAGNETIC RESONANCE
Hepatic hydatid cysts may have a low-signal-intensity rim on T2-weighted MR images (Fig.
10b).
This finding has been proposed as a characteristic sing of hidatid disease and probably represents pericyst which is rich in collagen and is generated by the host(1).
However,
this finding is not specific to hydatidosis and also described in amoebic abscesses,
hematomas and hepatocellular carcinoma.
When presents,
daughter cysts are seen as cystic structures attached to the germinal layer that are hypointense relative to intracystic fluid on T1-weighted sequences and hyperintense on T2-weighted images(Fig 10b).
Collapsed parasitic membranes appear in MR as a twisted linear structure within the cyst.
However,
calcifications are detected more clearly in the CT; MR is proving superior in demostrating irregularities of the rim,
which probably represent as incipient detachment of the membranes(Fig.11b).
COMPLICATIONS OF HYDATID DISEASE.
A .
- LOCAL COMPLICATIONS.
A.1.
- INTRAHEPATIC COMPLICATIONS.
Include cyst rupture and infection(Fig.
5,
7,
8)
Although rupture may be related to minor trauma,
the natural history of hepatic cyst implies rupture as a complication in 50-90% of cases (1).
Passage of the cyst contenst into the host's blood circulation can produce asaphylaxia due to the antigenic nature of the cyst fluid,
although cyst rupture may be clinically asymptomatic.
Have been described in the literature three different types of cyst rupture:
- Contained: Occur when endocyst breaks but pericyst remains intact.
It can be displayed as a membrane floating within the cyst.
May be related to trauma,
treatment response or cyst degeneration as part of the natural history of the same.
- Communicating: Implies passage of cyst contents into the biliary radicles that have been incorporated into the pericyst(Fig.
5,
7).
- Direct: Occurs when both pericyst and endocyst rupture,
allowing the spill hydatid material into the peritoneal cavity,
pleural cavity,
viscera or abdominal wall.
Direct rupture is more frequent in lesions located near the edges liver,
where there is less protection due to a cyst with a layer pericystic poor or poor response of host tissues to offer support.
In comunicating and direct rupture the cyst is drained and can become smaller and less spherical.
Both US and CT can demonstrate a defect in the wall of the cyst (Fig.
5d) and the contents thereof step through the defect,
especially in direct rupture.
In the MR images can be shown in an interrupt signal of low edge intensity of the cyst wall and an extrusion through the defect content.
Infection occurs only after rupture of both the pericyst and endocyst(direct and communicating rupture),
which allows bacteria to pass easily into the cyst (5-8% of cases) (1).Under normal conditions laminated layer is impermeable and prevents the passage of bacteria.
On clinical examination appears as a liver abscess.
US and CT findings are similar to those found in other hepatic abscesses (Fig.
7).
US findings are not specific.
Although the lesions usually show poorly defined margins,
can also be well defined.
The findings that suggest infection include a solid lesion appearance of a pattern produced by mixed solid and liquid components,
echogenic foci inside and air or fluid levels within the cyst.
CT is the test of choice to confirm a cyst complicated by infection.
Infected cyst usually manifests on CT as a mass with poorly-defined margins,
unlike the well-defined masses displayed in uncomplicated cases.
If administered intravenous contrast may appear a typical hyperdense halo around the abscess.
Sometimes,
can be seen patchy areas in the surrounding parenchyma of injury in connection with inflammatory changes.
As in the ultrasound on CT can be seen solid or mixed pattern appearance (solid and cystic components).
Addition in TC can be seen more clearly the existence of air and fluid levels within the cyst (Fig.
7a,
7d).
A.2.
- EXOPHYTIC GROWTH.
Cyst growth beyond limits the liver.
Anatomical structures such as the liver capsule,
ligaments or peritoneum can be used by hydatid cysts to grow beyond the boundaries of the liver.
The two most common routes are to the diaphragm and chest from the bare area of ââthe liver and into the stomach through gastrohepatic ligament.
A.3.
- TRANSDIAPHRAGMATIC CHEST INVOLVEMENT:
Involvement of the diaphragm and thoracic cavity occurs in 0.6 to 16% cases of hepatid hydatid disease(2),
with a mortality that varies in different cases from 5.6 to 43.7%(1).
Transdiaphragmatic migration (Fig.
9) usually occurs from cyst located in the posterior segments of the right lobe and has been linked to its proximity to the diaphragm.
The bare area of ââthe liver is the most common route of migration transthoracic,
and is described as a potential pathway for the migration of hepatic abscesses,
mainly because that naked areas lacking peritoneum offers little resistance exophytic cyst growth.
The used of other pathways is much less common.
Trasdiaphragmatic migration can vary from a simple adhesion to the diaphragm to rupture into the pleural cavity,
seeding in the pulmonary parenchyma and chronic bronchial fistulae.
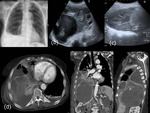
Chest radiograph may show pleural effusion (Fig.
9a),
elevation of the hemidiaphragm,
lung consolidation or laminated atelectasis at the lung base.
Occasionally,
an hourglass-shaped lesion or loculated pleural effusion similar to an empyema can be seen in the posterior thorax on the lateral projection (1).
US can help confirm the presence of hepatic hydatid disease and demonstrate pleural effusion (Fig.
9b,
9c) although rarely diaphragmatic defect is described with this imaging technique.
CT is useful in demonstrating transdiaphragmatic migration of hydatid disease and evaluate intrathoracic components (Fig.
9d).
MR in coronal and sagittal planes is also very valuable to demonstrate the migration through the diaphragm.
MR images allows accurate presurgical diagnosis based on various degrees of transdiaphragmatic migration and thus proved useful in surgical planning.
A.4.
- PERFORATION INTO HOLLOW VISCERA:
Spontaneous rupture of the cyst into hollow viscera is an extremely rare complication with an estimated frequency of 0.5% (1).
This complication may be associated with clinical symptoms such as hydatidemesis or hydatidorrhea.
Ussualy,
communication is not discovered until the surgery,
but in some cases can be found at radiology (Fig.
5,
7).
CT can demonstrate the existence of a cyst with a fluid level,
finding the oral contrast administered to the patient within the cyst cavity.
In some cases,
the performance of the TC with the patient in the lateral position right or left can help demonstrate in filling or emptying the cyst cavity.
Barium-enhanced CT can be used to demonstrate the fistula between the cyst and the hollow viscera.
A.5.
- PERITONEAL SEEDING:
Peritoneal hydatidosis is almost always secondary to hepatic disease,
however,
have been reported rare cases of primary peritoneal involvement.
The overall frequency of peritoneal disease in case of echinococcosis involving the abdomen is aproximately 13% (1).
Most of these cases are related to previous surgery of liver disease,
although spontaneous asymptomatic microruptures of hepatic cysts into the peritoneal cavity are not uncommon,12%(1).
CT is the modality of choice because it allows imaging of the entire abdominal cavity and pelvis.
Cysts may be multiple and located anywhere in the peritoneal cavity.
Radiological findings are similar to those of liver disease.
Peritoneal hydatid disease can grow to fill completely the peritoneal cavity,
simulating a multiloculated mass.
This pathological condition has been referred to as encysted peritoneal hydatidosis.
A.6.
- BILIARY COMMUNICATION:
Communication of hydatid disease with biliary tree has been described in up to 90% of hepatic cysts (2).
This can be explained by the fact that during the growth of the cyst,
small biliary radicles are incorporated into the pericyst.
However,
frank rupture into the biliar tree occurs only 5-15% of cases (2).
Jaundice,
fever and chills are symptoms that occur most often associated with biliary obstruction and cholangitis occurring secondary to this communication.
The communicating rupture of the cyst to the biliary tree can occur through small fissures or bile-cyst fistulas (55% of cases) or through a large perforation that allows access to a primary biliary branch.
It is essential that the findings in imaging tests that are suspicious for biliary communication are described to ensure adequate surgical management.
However,
dilatation of the biliary tree does not always indicative cyst breakage; it can result from direct compression of the biliary branches by the cyst (Fig.
6) or a associated common bile duct stone.
The only direct sign of rupture into the biliary tree is the visualization of a defect in the cyst wall or of a communication between the cyst and the biliary radicals.
In cases of a wider communication,
US and CT demonstrate rupture in 46-75% and 77% (1) of the cases,
respectively.
In some cases,
the passage of material through the defect hydatid and subsequent filling of the biliary radicals or the bile duct (common bile duct) can be displayed.
In such cases,
ultrasound images show anechoic,
rounded or echogenic linear structures without posterior acoustic shadowing in the biliary tract.
CT may demonstrate high attenuation material passing through the defect of the cyst wall and filling of the biliary radicals or common bile duct.
CT is superior to US in depicting hydatid cysts contents in the distal segment of the common bile duct.
Endoscopic retrograde cholangiopancreatography and percutaneous transhepatic cholangiography may demonstrate the communication in more detail.
Indirect signs of biliary communication include increased echogenicity at US and fluid levels and changes in signal intensity on MR images.
A air-fluid level within the cyst,
previously described as a sign of infection,
is also considered a sign of breaking both the biliary tree or hollow viscera or bronchopleural fistula.
Lipid material which forms a fat-fluid level within cyst has also been described as an indirect sign of biliary communication.
A.7.
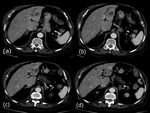
- PORTAL VEIN INVOLVEMENT
Involvement of the portal vein compression or thrombosis,
with secondary cavernomatosis,
are rare and are caused by cysts located in the caudate lobe and the hepatic bifurcation (Fig.
8c).
Direct portal invasion is a very rare complication.
US shows lack of flow at the portal vein and the existence of numerous vessels at the hepatic hilum associated with portal cavernomatosis.
CT and MR images help confirm cystic filling of the portal lumen and helped assess the lack of flow within the portal venous system (1).
A.8.
â ABDOMINAL WALL INVASION:
Cysts can invade the right anterolateral abdominal wall from the right hepatic lobe and the anterior abdominal wall from the left hepatic lobe.
Cysts typically pass through a small hole adopting an hourglass morphology.
The images reveal a cystic mass in the abdominal wall that is similar to and is in communication with the components hepatic hydatid cyst.
B.
HEMATOGENOUS DISSEMINATION
B.1.
â LUNGS.
The lungs are the second most commonly affected organ in hematogenous spread in adults and probably the first in children (15-25% of cases) (2).
Compressible organs such as the lung or brain facilitate the growth of the cyst,
and this has been proposed as the reason for the high prevalence of the disease in childhood.
Many cysts are acquired in childhood and remain asymptomatic for long periods of time,
and are diagnosed incidentally on a chest radiograph.
Cysts are multiple in 30% of cases,
bilateral in 20%,
and are located in the lower lobes in 60% of cases (2).
Calcification in pulmonary cysts is very rare (0.7% of cases),
but can be seen in pericardial,
pleural and mediastinal cyst (2).
Sudden coughing attacks,
rib pain and hemoptysis are the most common symptoms.
After cyst rupture may occur expectoration of cyst fluid,
scolices and membranes.
Although allergic episodes can occur after this rupture,
severe anaphylaxis is rare.
Bacterial infection of the cyst is one of the most serious complications seen after rupture.
Uncomplicated cysts appear as a well-defined mass.
Centrally located cysts are usually round,
although more peripheral may have an oval morphology.
Pulmonary hydatid cysts can vary from 1 to 20cm.
Cyst growth produces erosions in the bronchioles that are included in the periquiste and as a result,
air is introduced between the membrane laminated and pericyst.
This collection of air appears as a thin radiolucent crescent in the upper portion of the cyst and is known as the crescent sing or meniscus sign.
Some authors believe that this is a sign of impending rupture and therefore an indication for emergency thoracotomy.
If air continues to enter this space separating the two layers just completely and cyst shrinks and breaks,
allowing the passage of air to endoquiste.
A air-fluid level inside the encocyst an air between the endocyst and pericyst with an appearance in "onion peel" constitute the Cumbo sing(1).
After partial expectoration of cyst contents,
the cyst was empty and collapsed membranes can be visualized within the cyst (serpent sign).
When the cyst is completely collapsed,
the crumpled endocyst floats freely in the cyst fluid ("water lily sign").
If the liquid is completely evacuated by expectoration,
the remaining solid component will fall to the most dependent area of ââthe cavity (âmass within the cystâ) (1).
Hydatid disease is a rare cause of recurrent acute pulmonary embolism.
This complication may occur after the invasion of the cardiovascular system or direct invasion of the inferior vena cava.
B.2.
- KIDNEYS.
Renal involvement occurs in 3% of cases(1)(2).
Usually remins asymptomatic for many years (Fig.
10).
The most common signs and symptoms are palpable masses in the flanks,
pain and dysuria.
Cysts are often solitary and located in the cortex,
and may reach 10 cm.
before symptoms are noted.
At excretory urography,
uncomplicated cyst may cause a bulge in the contour of the kidney and appear as a round mass that lengthens the infundibula and chalices.
In up to 18% of cases,
the cyst can rupture into the collecting systems,
resulting in acute renal colic and hydatiduria.
Several round filling defects can be displayed in the excretory system due to daughter cysts.
The ring-shaped calcifications of the cyst walls suggest the diagnosis of hydatid cyst.
US and CT images of renal hydatid cysts are similar to those of cysts in other locations (Fig.
10).
B.3.
- SPLEEN
The reported incidence of splenic involvement of hydatid disease ranges from 0.9 to 8% (2).
In some series,
the spleen is the third most commonly affected organ after the liver and lung.
The splenic hydatidosis is mainly produced by systemic dissemination or intraperitoneal seeding from a ruptured liver cyst.
The most common signs and symptoms are abdominal pain,
splenomegaly and fever.
Splenic hydatid cysts are usually solitary,
and radiological findings are similar to cysts in other locations.
Calcification of the cyst wall may occur and is best characterized by CT than by plain radiography or US.
CT may demonstrate the typical high-attenuation linear wall without calcifications as well as daughter cysts within the cyst.
B.4.
- BRAIN.
Hydatid disease affects the central nervous system in 1% of cases and is usually diagnosed in childhood (1) (2).
Although you can find anywhere in the central nervous system more often to be located in both hemispheres,
particularly in the territory of the middle cerebral artery.
In young patients,
radiography of the skull can show suture separation,
unilateral enlargement of the vault or erosion of the posterior clinoid processes.
CT and MR showed a well-defined oval lesion or a cystic mass with an attenuation or signal intensity similar to cerebrospinal fluid.
Cyst may cause a compression of the ventricular system and therefore hydrocephalus,
however not associated with the displayed typical edema in cystic tumors and abscesses.
The lesion does not enhance after intravenous contrast administration and calcification is extremely rare.
B.5.
â BONE:
Skeletal involvement by primary hydatid disease is uncommon and represents 0.5-4% of patients.
The spine and pelvis(Fig.
11 b),
followed by the femur,
tibia,
humerus,
skull and ribs are most frecuently affected.
In bone involvement,
pericyst formation does not occur,
thereby allowing aggressive proliferation unevenly along the lines of least resistance especially the bone canals.
The parasite replaces the osseous tissue between trabeculae due to the slow growth of multiple vesicles.
With time,
the parasite reaches and destroys the cortex producing seed of disease to surrounding tissues.
Intraosseous hydatid disease rarely show the calcifications.
Spinal hydatid disease is the most common form of skeletal involvement and is usually difficult to distinguish from tuberculous spondylitis or chronic osteomyelitis.
Some images have been described characteristics of spinal hydatidosis.
These includes lack of osteoporosis or sclerosis in the host bone,
no damage interdiscales spaces and vertebral bodies and spread of the disease by subperiosteal and subligamentous path; paraspinal extension and particularly the involvement of the adjacent rib.
Although CT allows a very accurate assessment of bone lesions and clearly shows calcifications,
MRI is superior in demonstrating the involvement of neural structures.
Hydatidosis affecting other osseous locations typically manifested areas of different sizes of pure osteolysis that may become confluent and cause thinning of the cortex.
The lesion growth causes breakage of the bone cortex and consequently spread into the surrounding tissues(1).
B.6.
- OTHER LOCATIONS
Hydatid disease can affect almost any part of the human anatomy mainly through hematogenous spread.
The unusual locations include heart,
pericardium,
orbits,
gastric wall,
retrocrural space,
mediastinum,
subcutaneous space,
muscles and adrenals.
Hydatid disease should be included in the differential diagnosis when a cystic lesion is identified in a patient lives or comes from an area where hydatid disease is endemic,
especially if some of the images displayed characteristics that we discussed (multivesicular cyst,
calcification ,
intracystic membranes ...).
The orbital involvement occurs in less than 1% of cases.
In endemic areas,
the orbital hydatid disease is the second most common injury at this level after dermoid cyst.
Serologic tests and imaging findings in other locations help confirm the diagnosis.
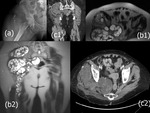
The soft tissue hydatid (Fig.
11) disease occurs in 0.5-4.7% of patients living in endemic areas (3).
The growth of cysts inside muscles is hampered by the contractility of the muscles and the presence of lactic acid.
The affinity for the muscles of the neck and trunk and root ribs can be explained by the high vascularity and low activity of these muscle groups.
Primary muscular hydatidosis is rare.
Radiologic findings of hydatid disease in soft tissue are well defined in the literature.
The multivesicular lesion is characteristics of hydatid disease and presents with multiple daughter cysts within the parent cyst,
whereas complex or solid lesion is the result of inflammatory changes mimicking a tumor.
In that case MR and US could be useful in the diagnosis (3).
On US the multivesicular lesion is characteristic but soft tissue hydatidosis can have multiple appearances unilocular cyst,
unilocular cyst with daughter cysts inside or detached membranes and calcified cysts.
Multiple hydatid cysts can be seen associated with spontaneous rupture,
trauma or surgery.
Edema or acute inflammation caused by compression of or allergic reaction in soft tissue adjacent to the cyst is uncommon but may be seen (2).
MR imaging has become the best imaging modality for the detection and characterization of soft tissue masses (Fig.
11b).
The MR imaging provides excellent definition of muscle,
facial boundaries and tumor mass by its multiplanar imaging capability (4).
A low-signal.intensity rim is evident on T2-weighted MR images(Fig.
11b).