Several techniques are available for evaluation of the prolapse of the pelvic floor:
FLUOROSCOPY
It does not allow for evaluation of soft tissues and a concurrent evaluation of all three compartments is practically impossible.
CYSTOURETHROGRAPHY
It is employed to assess urinary incontinence,
but its accuracy is low (50-60%).
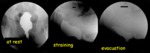
DEFECOGRAPHY
It allows to evaluate the initial level of the pelvic floor and the degree of descent during evacuation.
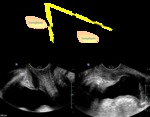
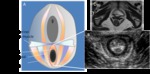
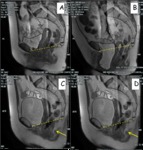
DYNAMIC CYSTOCOLPOPROCTOGRAPHY (fig.2)
This imaging test allows for a concurrent performance of defecography and cystocolpourethrography,
evaluating the rectal ampulla,
the anal canal,
the urethra,
and the vagina at the same time during evacuation using a video recorder.
ULTRASOUND
This imaging modality has the great advantages of being low cost,
readily available,
easy to perform,
and does not use ionizing radiations,
its main limitation is the relatively narrow field of view,
that does not allow for a comprehensive evaluation of all pelvic organs as a whole.
The recent introduction of three-dimensional ultrasound imaging increased visibility of prolapse and of pubo-rectal avulsion,
as well as any enlargement of the uro-genital hiatus,
thanks to the possibility of performing three-dimensional reformatting.
Trans-labial approach allows for an accurate study of both the anterior (bladder and urethra) and medium (vagina and uterus) compartments of the pelvic floor,
as well as a number of connective support stuctures.
The probe (high or low frequence) is applied directly on the perineum,
between the labia majora,
directly on the urethral meatus and the vulva.
Ultrasound beam is directed upwards to visualize the hiatus of the pelvic floor and the pubo-rectal muscle,
and posteriorly to visualize both internal and external sphincters.
Images are acquired with the patient in gynecologic position.
In functional studies of the pelvic floor,
the exam must be performed with bladder replenished of urine,
both at rest and during Valsalva manoeuvre.
A video-loop registration can be useful to assess the urethral-vescical dynamic in relationship with others pelvic organs.
Also,
urethral-vesical angle and urethral funneling may be seen.
The supra-pubic scan allows for evaluating bladder morphology and wall thickness as well as residual urine after urination.
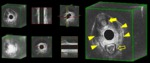
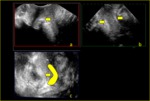
Volumetric evaluation allows for an acquisition of the entire volume of the posterior compartment of the pelvic floor,
that can be later reformatted on different planes,
according to the relevant structure to assess (fig.7).
This allows for a precise evaluation of the sphincters and of the musculotendinous structures and for a representation of the anatomic structures along all possible axial-oblique and coronal plans,
adapting to the anatomic plan to be evaluated.
So three-dimensional ultrasound imaging increases visibility of prolapse and of pubo-rectal avulsion,
as well as any enlargement of the uro-genital hiatus.
Volumetric imaging of the pelvic floor can be obtained using two different techniques:
-
Endo-vaginal mechanic probes with sectorial US emission,
used with a trans-labial approach.
Dataset has a trapezoid shape;
-
Endo-rectal/endo-vaginal with circumferential US emission.
Dataset has a cyilindric shape.
Endo-anal ultrasound allows for evaluating integrity of the inner and outer sphincters in patients affected by fecal incontinence.
The mucosal and submucosal layers have generally a hyperechoic appearance.
The inner sphincter has a uniform hypoechoic appearance and its thickness usually does not exceed 3 mm.
Conversely,
the outer sphincter is slightly hyperechoic with variable thickness.
Although ultrasound is a well-established imaging modality to evaluate the anterior compartment and of the anatomy of sphincters,
the role of this modality in the assessment of rectocele,
invagination,
and prolapse is still debated.
Dietz demonstrated a good correlation between ultrasound and clinical staging of prolapse of all compartments,
while other authors reported poor agreement between ultrasound and conventional proctography.
Ultrasound evaluation of anterior compartment
At conventional B-mode ultrasound imaging,
urethra has a thin hypoechoic bandlike appearance that can be detected both on sagittal and coronal scans.
The striated sphincter surrounds the hypoechoic structure and appears as a double-layer hyperechoic line when imaged on the long axis.
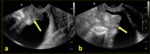
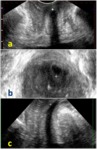
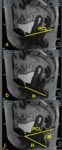
During Valsalva manoeuvre (fig.3),
in patients with urethral hypermobility or cystocele,
the ultrasound beam images the urethra on the short axis.
Thus,
external layer could appear more hyperechoic than what can be appreciated on the long axis.
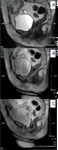
Ultrasound is also extremely helpful in detecting the descent of the anterior compartment,
the anterior vaginal wall,
and the cystocele (fig.4) that results from them.
The principal role of ultrasound in this setting is to evaluate bladder neck mobility and funneling of the internal uretrhral meatus.
The measurement of the position of neck and urethra should be done at rest and during Valsalva manoeuver in order to evaluate the presence of a bladder neck descent (BND).
A BND value of 20-25mm is generally considered normal,
but this has not been established yet.
Ultrasound evaluation of median compartment
Generally,
uterine prolapse is evaluated clinically.
However ultrasound is able to evaluate the effects of cervical anterior displacement that results in abnormal bladder emptying in patients with retroverted uterus.
In patients with antiverted uterus,
ultrasound may also demonstrate the presence of anterior compression on the rectal ampulla that results in obstructed evacuation (colpocele).
Ultrasound evaluation of posterior compartment (fig.12)
Ultrasound evaluation of posterior compartment in clinical routine is yet to come.
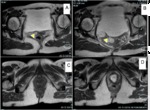
The anal sphincters can be assessed using endoanal approach with 360° rotating probes (fig.6),
with endovaginal approach,
or with three-dimensional probes and subsequent image reformat on axial planes.
Rotating probes have high spatial resolution and allow for evaluating also small sphincterial abnormalities.
However,
an extra-anal approach allows for both avoiding anatomic distortion on the anal canal and performing dynamic evaluation during sphincterial contraction.
Finally,
axial reformat of three-dimensional images are particularly helpful to assess the uro-genital hiatus,
the elevator ani muscle,
and the peri-urethral affections.
The main morphological abnormality related to pelvic floor prolapse is the direct damage or the atrophy of levator ani muscle,
following direct trauma on the pudendal nerve after pregnancy and delivery.
Traumatic avulsions can be assessed using three- or four-dimensional reformat of volume scans.
Implantable devices
Implantable sub-urethral slings (fig.8) are commonly used to treat abnormalities of the anterior compartment.
They usually appear as hyperechoic structures and are easily detectable on three-dimensional reformat axial scans of the perineum at ultrasound.
This imaging modality may be used to evaluate the efficiency of those devices in case of symptoms recurrence.
Meshes are increasingly used in clinical practice and failure of their positioning is a common occurrence.
They can be assessed using three-dimensional ultrasound but their curvilinear course may hinder their complete visibility on a single plane.
Ultrasound can be also used to detect any post-implantation complications (such as abscesses) or wrong positioning.
MRI
The dynamic MR of the pelvic floor can be performed by two different techniques: using open configuration MRI scanner with the patient in supine position or using closed bore configuration MRI scanner with the patient in sitting position.
The second option is useful for evaluation of effects of gravity and so it allows a more physiological assessment of the anorectal dynamic during defecation.
However,
the identification of pathological findings can occur with both techniques without significant clinical differences.
For dynamic studies of the anterior compartment it is necessary an adequate bladder repletion,
while evacuation dynamic studies make it essential rectal filling with various filling materials according to the sequences to perform (generally it is used the introduction of sonographic gel in quantity between 200 and 300 ml before placing the patient in the gantry.
A better highlighting of the vagina,
of the fornix and of the dynamic alterations due to straining is available by filling the vagina with 50 ml of sonographic gel).
The MRI allows both a morphological and a dynamic-functional study.
The morphological study is conducted through the use of Fast Spin Echo T2-weighted traditional sequences according to the three orthogonal planes of the space,
allowing a very good anatomical detail of pelvic organs and muscles and so to highlight signal abnormalities or pathological asymmetries that often turn out to be the cause of altered pelvic functionality.
The dynamic-functional study is generally realized through ultrafast single shot T2-weighted sequences on axial and sagittal scanning planes,
with single acquisition time of 10-12 seconds,
thus allowing to capture the first image in the basal state and then:
1.
During contraction maneuver,
in order to assess the contraction of puborectal muscle.
2.
During defecatory phase with the contrast in the rectum,
in order to examine the rectal alterations and the pelvic organs prolapse.
3.
Post-defecatory during Valsalva manouver,
in order to identify and emphasize the presence of possible enterocele and cystocele.
The sequences performed in the individual phases can be assembled with cine-loop technique,
allowing the cine-MR imaging defecography.
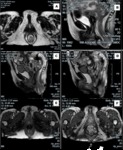
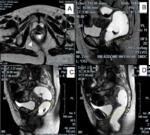
MR interpretative criteria (fig.13):
A) pubo-coccygeal line (PCL) drawn between the lower edge of the symphysis pubis and the last coccygeal joint.
It represents the plane of the pelvic floor and it is the anatomical landmark by which the pelvic organ prolapse has to be measured
B) The H line corresponds to the plane passing through the lower margin of the symphysis pubis and the posterior wall of the rectum at the level of anorectal junction.
C) The M line is a vertical line drawn at right angles between the rear end of the H line and the PCL line.
In normal conditions the H line has an extension of not more than 5 cm and the M line an extension of not more than 2 cm.
Bladder and urethra: the bladder and urethra are easily visible with MRI both in static and dynamic phase; urethral and bladder hypermobility can be demonstrated during Valsalva.
An abnormal descent and rotation of the the bladder floor and urethra below the pubo-coccygeal line are considered abnormal and can be defined with the term of cystocele (fig.12).
However,
this event is also found in subjects continents and nulliparous: the cut-off for the definition of the cystocele is set at 20 mm.
Vagina and uterus: the cervico-vaginal junction and the vaginal wall are visible in static and dynamic phase in the median sagittal plane.
The uterine and vaginal prolapse is generally defined as the descent of the vaginal wall or cervico-vaginal junction below the pubo-coccygeal line; this condition can be found also in normal subjects for which the cutoff of the descent for the definition of prolapse is generally quantized in 30 mm.
Only above this value functional implications with possible impediment to the rectal emptying can be found.
Puborectal function: normal puborectal contraction leads to a reduction of 11° between the contraction and the push.
During pushing,
the ano-rectal junction migrates superiorly and anteriorly.
During the evacuation the puborectal muscle normally relaxes,
resulting in an enlargement and an increase of ano-rectal muscle.
Dynamic MRI showes small changes of ano-rectal angle,
due to the relaxation of the puborectal muscle during evacuation in patients with obstructed defecation.
The rectocele (fig.11) is a prolapse of the anterior rectal wall whose entity is measured from the line above the anal canal.
In the elderly patient rectocele less than 2 cm has to be considered normal.
A prolapse over 4 cm acquires clinical significance.
The syndrome of the descending peritoneum is a complete loss of tone of the whole pelvic floor,
which results in a complete descent of the pelvic floor during Valsalva or evacuation.
The etiopathogenesis is various: delivery,
constipation and pudendal neuropathy,
associated to other diseases (eg diabetes).
Defeco-MRI can quantify the descent of the anorectal junction below the PCL,
furthmore the enlargement of the hiatus can determine elongation of the H and M lines with modification of caudal angle of the elevator.
The syndrome can determine incontinence as well as incomplete evacuation.
This syndrome can be evaluated by anal manometry,
endo-anal US realized with rotating probe,
but MR-defecography can clearly demonstrate alteretions related to sphincterial damage in order to plan the surgical treatment performed to solve the incontinence (if defeco-MR shows associated rectocele or enterocele,
the surgical tretment to perform is different).