-SKULL AND CRANIO-FACIAL DEFORMITY
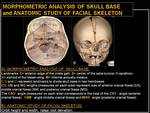
Morphometric analysis of skull base and anatomic study of facial skeleton.
3D CT scanning is used to perform morphometric analysis of skull base and for evaluating facial skeleton deformity.
We evaluated the skull base asymmetry and the craniofacial deformities on the basis of the following measurements:
- the direction and the angle of skull’s endocranial base deflection;
- the angles between the petrosal pyramids and the midline (posterior petrosal sagittal angle: PPSA);
- ethmoidal axis deviation;
- “minor” sutures involvement;
- nasal root deviation;
- orbit height and width.
Note that cranio-facial asymmetry may also be caused by mechanical factors in utero or after birth (positional deformity); skull base is involved only in craniosynostosis (not in positional deformity).
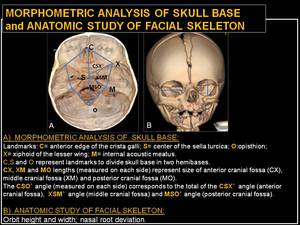
Fig. 12: Morphometric analysis of skull base and anatomic study of facial skeleton.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
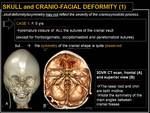
Premature fusion of cranial sutures in infants leads to profound changes in craniofacial form and in skull base simmetry ; there is a complex relationship between calvarium,
skull base and facial skeleton.
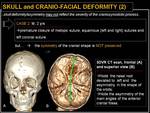
Note that skull deformity/asymmetry (involving the skull base and /or the facial skeleton) may not reflect the severity of the the craniosynostotic process; symmetry is often preserved when multiple sutures are simultaneously closed,
while it is often not preserved when when sutures are asymmetrically closed on the right or left side.
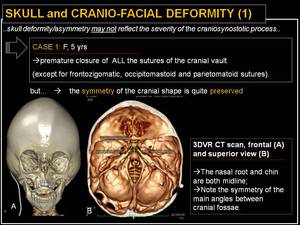
Fig. 13: Skull and cranio-facial deformity (1): symmetry preserved.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
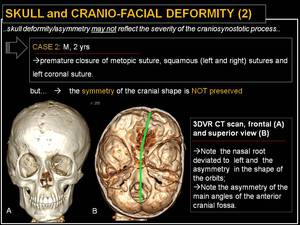
Fig. 14: Skull and cranio-facial deformity (2): symmetry not preserved.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
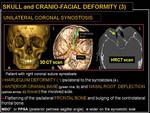
Most of the craniofacial deformities are associated with premature closure of the coronal arch sutures .
The coronal arch can be divided into two hemirings; synostosis anywhere along the coronal hemiring can restrict growth at other sutures.
The dismorphology of the pathologic sutural fusion along the coronal ring (commonly referred to as anterior plagiocephaly) is specific to which component suture(s) is (are) fused.
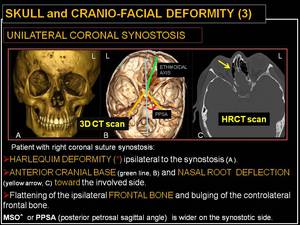
Fig. 15: Skull and cranio-facial deformity (3): unilateral coronal synostosis.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
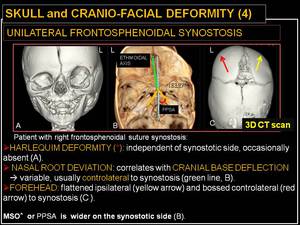
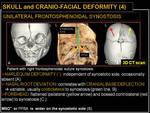
Fig. 16: Skull and cranio-facial deformity (4): unilateral frontosphenoidal synostosis.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
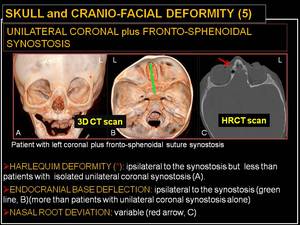
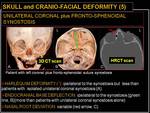
Fig. 17: Skull and cranio-facial deformity (5): unilateral coronal and frontosphenoidal synostosis.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
-CLINICAL PRESENTATION
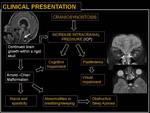
The premature fusion of multiple sutures prevents cranial growth in response to normal brain growth.
As a result of continued brain growth within the confines of a fixed skull,
the Monro–Kellie Doctrine predicts that intracranial pressure will rise.
The incidence of elevated intracranial pressure is significantly higher in cases of multiple suture fusion than in cases of single suture synostosis; as such,
the symptoms of elevated intracranial pressure are more commonly seen in cases of pansynostosis.
The sequelae of prolonged intracranial hypertension may include cognitive impairment,
visual and sleeping impairment,
ataxia and spasticity.
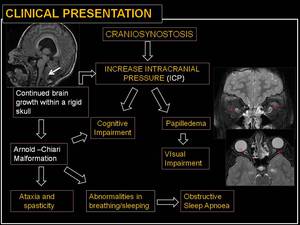
Fig. 18: Clinical presentation.
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
-SURGICAL TREATMENT
Therapeutic intervention for synostosis involves surgical intervention as the mainstay.
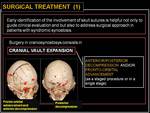
Surgical treatment depends on the type of craniosynostosis and on the patient’s age; ideally,
the child should be operated on between the third and twelfth month of life.
Surgery consists of cranial vault expansion: anterior/posterior decompression and/or fronto-orbital advancement (as a staged procedure or in a single stage).
After surgery,
ICP decreases because the constricted brain has the opportunity to expand into the newly formed cavity.
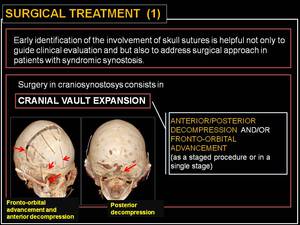
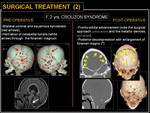
Fig. 19: Surgical treatment (1).
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT
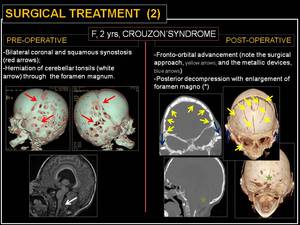
Fig. 20: Surgical treatment (2).
References: Department of Bio-imaging and Radiological Sciences, Catholic University of Rome - Rome/IT