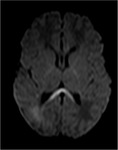
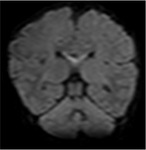
MERS is a clinical-radiological entity,
characterized by mild encephalitis or encephalopathy associated with reversible lesion of the corpus callosum,
which commonly involves the splenium.
Epidemiology
Affects mainly young patients and children,
being reported mostly in oriental population,
with more tan 50 published cases.
Its precise frequency is unknown,
but it is likely underreported,
since magnetic resonance imaging examination is not routinely performed in the responsible disorders.
[1]
Clinical presentation
Clinically its present with nonspecific prodromal symptoms including cough,
rhinorrhea,
vomiting,
headache,
and sore throat.
Later symptoms are consistent with encephalopathy as speech difficulties,
drowsiness,
decreased consciousness,
delirium,
seizures,
irritability,
agitation,
and disorientation.
[2] A multi-center study performed in Japan showed that the most common neurological symptom is delirium behavior representing 54%.[3]
All reports refer present a mild clinical course,
with complete resolution of symptoms in a short period of time generally does not exceed 30 days from the onset of symptoms.
Causes
The first description of this entity was by Chason et al.
in 1996.
Lately it has been described in patients with encephalitis/encephalopathy of varied etiology,
including infections,
high altitude cerebral edema,
metabolic disturbances like hyponatremia and hypoglycemia,
and antiepileptic drug therapy.
It also occurs in nonepileptic patients who are on antiepileptic drugs for other reasons.
During the last years several studies have been reported related to other causes such as measles,
rotavirus,
hemorragic fever,
neuroleptospirosis.
Also associated to hemolytic uremic síndrome,
malnutrition during chemotherapy,
anorexia nervosa and use of corticosteroids.
There are few reports of reversible splenium lesion in neonates.
(Fig 1-2).
Some authors postulated that the timing of the MRI or the severity of brain damage influenced the results.
Barkovich described differences in the pattern of injury in neonates cases during the first two weeks after the clinical onset.[4]
Pathophysiology
Reversible brain lesions have been attributed to the transient development of intramyelinic edema due to the separation of myelin layers,
which is a possible mechanism for the transiently decreased diffusion of the splenium lesion.[5] It has to be remembered that during the neonatal period myelination of the corpus callosum is not completed and then,
the hypothesis of intramyelinic edema cant be the cause of the diffusion weighted imagingsignal.
The reduced diffusivity might be the result of interstitial edema in the extracellular space between tightly packed axons.
Reversible diffusion changes in the corpus callosum are also observed in patients with epilepsy receiving antiepileptic drugs,
in which the involvement of focal cytotoxic edema occurring at the glial level is speculated by the absence of fiber interruption on diffusion tensor imaging.[6] Kim et al.
attributed it to possible anti-epileptic drug (AED) toxicity induced reversible demyelination.
Others postulated that sudden cessation of AED could lead to alteration of the arginine-vasopressin (AVP) system,
resulting into hydric imbalance.
[7]
Another possible explanation is the development of an inflammatory infiltrate.
The influx of inflammatory cells and molecules,
possibly combined with related cytotoxic edema,
might have decreased the ADC.
Some authors have examined oxidative stress markers in cerebralspinal fluid (CSF) in MERS patients demonstrating that the values of tau protein in the CSF were not increased,
indicating less possible involvement of axonal injury.
This is in good accordance with the absence of fiber interruption on diffusion tensor imaging in the aforementioned epileptic patients with a similar SCC lesion.
The symmetry and absence of contrast enhancement makes an inflammatory etiology less likely.
Others authors suggests that the difference in arterial vascularization and/or water content in the corpus callosum may lead to the frequent occurrence of SCC lesion.
The reversibility of the lesion of the splenium of the corpus callosum within a brief period also suggests that this entity is distinct from the cytotoxic edema seen in cellular energy failure,
such as an acute infarction,
which is nearly always irreversible.
Some genetic factors might predispose to reversible lesion in the splenium.
Familial cases of clinically mild encephalitis/encephalopathy with transient splenial lesions have been reported,
and an autosomal recessive model of inheritance,
if any,
was suspected.
[8]