Classification
Recently,
reversible lesions with transiently reduced DWI have also been reported with lateral extension from the splenium into the frontoparietal subcortical white matter,
and with anterior extension to involve the entire corpus callosum.
Then,
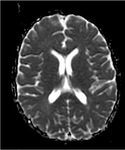
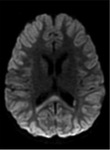
MERS is classified into types 1 which exhibits only splenial corpus callosum lesions,
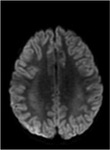
and type 2 that shows white matter lesions in addition to lesions of the entire corpus callosum; however,
the splenial lesion is always the last to disappear.
In general,
patients with MERS type 2 lesions have also good prognosis with complete resolution within two weeks.
MERS type 1 lesions are detected more frequently in patients with encephalitis/ encephalopathy than type 2 lesions.
Lesions on MRI corresponding to the so-called MERS type 2 lesions are not always given this name in the literature. (Fig.
3-7,
9-10)
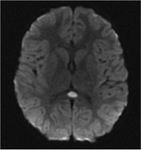
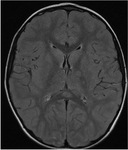
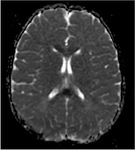
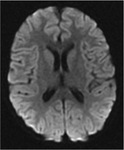
The splenium involvement appears hyperintense on T2WI and FLAIR image and iso- or hypointense on T1WI.
The changes in DWI appear earlier than the changes in T2WI and FLAIR.
Involvement of the splenium,
based on signal changes,
can be divided into two types according to its shape and extent: Oval,
circumscribed,
with well-defined borders usually located in the middle; or wider,
with less regular borders and involving the entire splenium ("Boomerang sign").
(Fig 8).
While MRI detected abnormality only in the splenium,
SPECT indicated hypoperfusion in areas with normal MRI findings,
some of which overlap with lesions involving MERS type 2.
It is possible that such hypoperfusion generally occurs in other MERS cases.
Magnetic resonance spectroscopy (MRS) revealed normal NAA/Cr and Cho/Cr ratios,
reflecting that there isn´t neuroaxonal damage and demyelination,
respectively.
Diffusion tensor MRI shows normal FA values reflecting indemnity of the fibrous structures.
[9]
Differential diagnosis
Among the differential diagnoses include posterior reversible encephalopathy síndrome (PRES),
diffuse axonal injury,
multiple sclerosis,
lymphoma and pontine myelinolysis.
In any encephalitis/encephalopathy patient with lesions in the white matter,
acute disseminated encephalomyelitis (ADEM) should be considered in the differential diagnosis.
However,
in ADEM,
recovery occurs within weeks,
and in our case the symptoms recovered within 7 days without specific treatment.
MRI in ADEM usually shows multiple foci of T1 and T2 prolongation in the subcortical white matter that typically is bilateral and asymmetric.
The lesions usually evolve over weeks to months and disappear only after several months.
After contrast-agent infusion,
ADEM lesions will show variable enhancement depending on their acuity.