From a total of 411 neurosurgical cranial procedures,
90/411 (22%) presented one or more postoperative complications (Table 1).
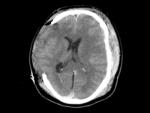
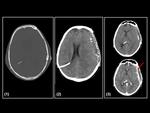
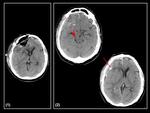
We found 18/90 (20%) extracranial herniations,
wich is a typical complication of the craniectomy (Figure 2).
The brain and vessels extrud through skull defect,
and if the defect is too small,
this can result in compression of cortical veins and lead to venous infarction and contusion of the brain at the craniectomy margins.
In our 46 patients who underwent decompressive craniectomy,
extracranial herniation occurred in 18 (39%).
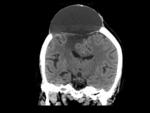
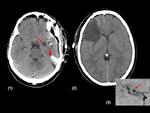
There were 16/90 (18%) hygromas: subdural or subgaleal fluid collections that usually appear within days of surgery and resorb over period of week to months.
They generally behave in a benign fashion; only 2/16 (12%) of them caused a brain tamponade wich is a rare but potentially life-threatening complication caused by a pressurized subgaleal fluid collection.
The diagnosis include the imaging findings in a context of neurologic deterioration of the patient and neurologic improvement after drainage of the fluid collection (Figure 3).
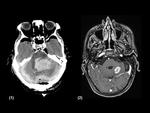
15/90 (17%) complications were some type of hemorrhage (Table 2): 5/15 (33%) subdural hematoma,
4/15 (27%) subgaleal hematoma,
4/15 (27%) intraparenquimatous hemorrhage (Figure 4 y 5) and 2/15 (13%) others hemorrhages (intraventricular hemorrhage).
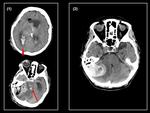
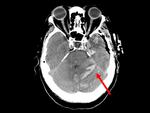
One of the intraparenchymal hemorrhage is actually a remote cerebellar hemorrhage (Figure 6),
it is thought that this complication results from cerebro-spinal fluid (CSF) volume depletion leading to sagging of the cerebellum,
with consequent occlusion of the superior bridging veins of the posterior fossa and hemorragic infarction.
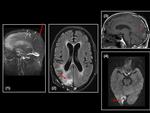
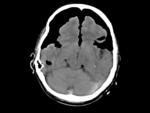
There were 14 (16%) infarctions (12 arterial (Figure 7) and 2 venous (Figure 8)).
The 2 venous infarctions were due to venous thrombosis in surgery for metastasis and meningioma resection.
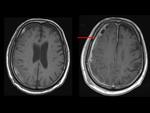
The rate of infection was 12/90 of the 411 procedures (13%) (Table 3): 4/12 (34%) were subdural empyemas (Figure 9),
fluid collections overlying the cerebral convexity or alongside the falx cerebri,
with attenuation slightly higher than that of CSF.
They often produce mass effect,
edema in the underlying brain and diffuse enhancement of the adyacent cortex.
There were 3/12 (25%) soft tissue or subgaleal infections,
which usually begin at the line of the skin closure,
so the role of imaging is to identify deep extension.
3/12 (25%) were CSF infections,
with ventriculitis or meningitis.
1/12 (8%) were intraparenchymal abscesses,
fluid collections wich whose margins appear thickened and enhanced after contrast administration.
Finally,
there was 1/12 (8%) bone flap infection in the context of a cranioplasty (Figure 10),
with abnormal texture and multiple lytic areas in the bone flap.
Finally,
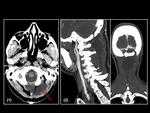
there were 10/90 (11%) hidrocephalus and 4/90 (4%) tension neumocephalus,
1 of them in the context of a posterior fossa surgery (Figure 11) and the other 3 after a supratentorial procedure,
all of them in tumor resections.
The tension pneumocephalus is a rare but potentially life-threatening complication that occurs when subdural air collections compress the brain.
Axial CT shows low attenuation collections with mass effect,
and sometimes we can see the "Mount Fuji" sign,
in which which bilateral tension pneumocephalus cause compression and separation of the frontal lobes from the falx cerebri.
Similar findings may be seen at imaging in asymptomatic patients,
so the diagnosis should be made only if clinical deterioration accompanies these imaging findings.
Special cases were classified as others:
- 2 cases of pseudomeningocele (Figure 12),
it is an abnormal collection of CSF that communicates with the CSF space around the brain.
In contrast to meningocele,
in which the fluid is surrounded and confined by dura mater,
in a pseudomeningocele,
the fluid has no surrounding membrane,
but it is contained in a cavity within the soft tissues.
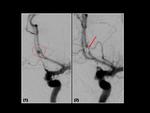
- 2 pseudoaneurysms (or false aneurysms): This is a hematoma that forms as the result of a leaking hole in an artery,
contained by the surrounding tissues.
We found one of them in transsphenoidal resection of pituitary macroadenoma (Figure 13).
- 2 venous thrombosis,
associed to the 2 venous infarcts before mentioned.
- 1 one-month-delayed-intraparenchymal-hemorrhage in a metastasis resection (Figure 14).
The rate of complications attending to the surgery indication was 38/203 (18%) in patients who had a tumor,
20/55 (36%) in patients who suffered a trauma and 22/90 (24%) in patients with vascular disease.
The other group is formed by 63 patients most of which were cranioplasties to repair a surgical skull defect,
from which we found 10 complications (16%) (Table 4).
Only the trauma sample presented a stadistically significant difference in the Chi square test (p < 0,05).
133 interventions were urgent,
most of them trauma emergencies,
and 43/133 presented postoperative complicacions while only 47/278 (17%) programmed interventions presented complications,
being these differences statistically significant in the Chi square test (p < 0,001) (Table 4).