The Vascular Interventional Radiology Unit of Reina Sofia Hospital,
in Murcia,
Spain,
is one of the principal unit for hemodialysis vascular access in our region.
It covers three secondary hospitals,
with their corresponding hemodialysis units,
and 7 peripheral dialysis centers.
We performed a retrospective study from January 2005 to December 2012.
We analyzed all cases with femoro-femoral PTFE prosthetic implants.
Of all patients analyzed,
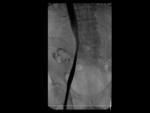
only 8 femoro-femoral PTFE prosthetic implants were found,
(3 in the right lower limb and 5 in the left lower limb) in 7 patients.
One patient had 2 PTFE. (Fig. 1 )
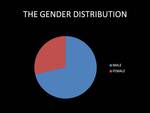
The gender distribution was 5 men (71.40%) and 2 women (28.60%),
with an average age of 63 (R= 45 - 79).
(Fig. 2 )
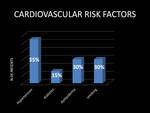
All patients had cardiovascular risk factors; the main cardiovascular risk was arterial hypertension (55% of cases),
also diabetes (15%),
dyslipidemia (30%) and smoking (30%),
among others.
(Fig. 3 )
The patients analyzed were heterogeneous,
they came from five different hemodialysis units.
In general,
patients have multiple diseases at the same time,
with a long history of hemodialysis.
The average time was 93 months (R: 22-183).
All patients had exhausted all vascular access sites in both upper extremities and suffered central venous injuries that made it impossible to place a central venous catheter.
For diagnostic and therapeutic reasons,
we had 61 assists for the Vascular Interventional Radiology Unit,
with an average of 8.7 assists per person.
The average age of the vascular access was 27.4 months (r: 3-109).
(Table 1 )
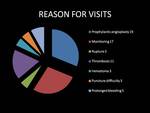
The reasons for the consultation were very different.
The most frequent reason for visits was prophylactic angioplasty which ocurred in 19 cases.
Other reasons for which patients attended were: radiological controls and multiple complications of the PTFE,
including thrombosis,
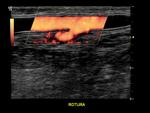
rupture (Fig. 15),
hematoma,
prolonged bleeding,
puncture difficulty,
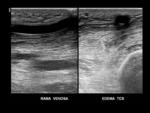
edema,
among others.
(Fig. 4 )
Of the total visits,
ultrasound guidance was performed on one hand in 9 instances without intervention,
on the other hand,
the 52 remaining visits needed some type of vascular intervention.
Hematoma was the most common injury monitored with ultrasound and without other radiological technique (37.5% of all lesions detected by ultrasound).
Other injuries have been found,
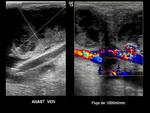
rupture (#4) (Fig. 5 ),
subcutaneous edema and pseudoaneurysm (#13).
(Fig. 6 - Fig. 7 ).
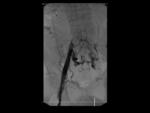
On 11 occasions we objectively evaluated graft thrombosis,
for an average time of fistula thrombosis of 4.7 days.
(R: 1-14).
(Fig. 8 - Fig. 16 )
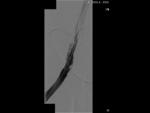
In total we performed 27 angioplasties,
(Fig. 17 - Fig. 18 ) (14 angioplasties performed on the same patient).
The dilatation balloons used were: CONQUEST 7 x 40,
10 x 40,
12 x 40,
14 x 40,
8 x 80; ATLAS 14 x 40,
16 x 40; BLUE MAX 6 x 40,
7 x 40,
8 x 40.
The most commonly used was ATLAS 14 x 40 (24%),
the second CONQUEST 10 X 40 (21%).
In most cases,
we used more than one balloon in the same intervention,
starting with the smaller caliber ones and ending with the highest caliber.(Fig. 9 Fig. 10 Fig. 11 Fig. 12 )
We performed five thrombectomies,
4 of them were only with manual aspiration maneuvers and in only one we needed a Fogarty.
We have implanted 11 stents (Fig. 19) (5 VIABHAN,
5 FLUENCY and 1 EVERFLEX) in 4 patients.
The main cause of stent implantation was the pseudoaneurysm (36% of the stent),
other causes were: Iliac vein stenosis,
stenosis elastic with a tendency to shrink,
loop,
Elastic Recoil,
mural thrombus attached and in one case,
a rupture of a previous stent.
(Fig. 13 )