Type:
Educational Exhibit
Keywords:
Thorax, CT-Angiography, Diagnostic procedure, Haemorrhage
Authors:
C. Spinu, E. Castañer González, M. Andreu, X. Gallardo, J. M. Mata Duaso, J. C. Tortajada Bustelo, M. Cufi; Sabadell (Barcelona)/ES
DOI:
10.1594/ecr2013/C-1432
Background
- Hemoptysis is defined as the expectoration of blood originating from the tracheobronchial tree or pulmonary parenchyma.
- The quantification of blood is difficult from the clinical point of view,
so the term more useful is life-threatening hemoptysis (LTH),
to define a situation where there is an immediate risk to the life of the patient,
which is the airway compromise; the clinical significance of an episode of hemoptysis should take into account not only the volume of expectorated blood,
but also the effects on the patient’s respiratory and cardiovascular reserves.
- Life-threatening hemoptysis is rare; conservative management carries a mortality rate of 50–100%.
- Urgent surgery in patients with active bleeding is associated with high morbidity and mortality,
from this bronchial artery embolization (BAE) is currently the treatment of choice in most cases.
- The initial evaluation of patients with hemoptysis is directed to identify the origin and underlying cause of the bleeding.
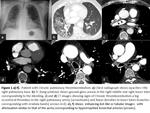
- First exploration of a patient with LTH is a conventional radiography (which often is useful in localizing the bleeding area (fig.
1.
a-f), followed by a CT angiography of the chest.
Currently in our hospital are not made urgent bronchoscopy studies at these patients.
- Pretreatment realization of MDCT angiography allows a detailed evaluation of the mediastinum and pulmonary parenchyma,
resulting in angiographic studies of the thoracic vasculature (systemic and pulmonary) and upper abdomen,
which are useful for planning the embolization,
or surgery in certain cases.
Pathophysiologic features and Causes of hemoptysis
-
The lungs are supplied by a dual arterial vascular system:
(1) pulmonary arteries,
which account for 99% of the arterial blood supply to the lungs and take part in gas exchange; and
(2) bronchial arteries,
which are responsible for providing nourishment to the supporting structures of the airways,
but do not normally take part in gas exchange.
-
Histologically,
the two systems are connected by anastomoses between the systemic and pulmonary capillaries.
-
Conditions causing decrease of pulmonary circulation and maintained ischemia (eg,
chronic thromboembolism),
the bronchial circulation responds with a focal vascular hypertrophy and proliferation through the anastomotic channels,
to replace the pulmonary circulation.
-
The neoplastic disease and chronic inflammation (eg,
bronchiectasis and chronic infections),
by angiogenic growth factors,
produce neovascularization and increased systemic circulation.
-
These neoformed and hypertrophied systemic vessels are usually very fragile and are exposed to systemic pressure,
so they tend to break at its distal portion (capillary) into the bronchial lumen or alveoli,
causing hemoptysis.
-
The bronchial circulation is the most frequent source of hemoptysis (90% of cases),
but nonbronchial systemic arteries,
as well as pulmonary arteries,
on rare occasions,
may also contribute.
- The underlying causes of hemoptysis vary depending on the geographic location of the study,
the prevalence of tuberculosis and the use of CT studies.
In our area the most common causes of LTH are bronchiectasis,
tuberculosis and its sequelae and lung cancer.
Table 1 shows the main causes of LTH.