Keywords:
Head and neck, Interventional vascular, Neuroradiology brain, Catheter arteriography, CT-Angiography, Embolisation, Fistula
Authors:
T. J. Popiela, P. Brzegowy, A. Urbanik; Krakow/PL
DOI:
10.1594/ecr2013/C-1447
Methods and Materials
The analysis was conducted in 13 patients with carotid-cavernous fistula (mean age 46 years) treated with intravascular embolization between 2005 – 2011.
In all patients the diagnosis was established based on the typical clinical symptoms,
including exophthalmia, conjunctival congestion,
progressive ophthalmoplegia,
pulsatile tinnitus,
and imaging examination findings.
All patients had been assessed by both,
a neurologist and neurosurgeon, and some of them by an ophthalmologist.
Nine patients underwent CT angiography,
and four MR angiography.
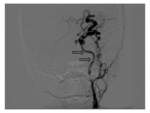
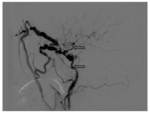
Each time intravascular procedure was preceded by bilateral selective angiography (DSA) of both internal and external carotid arteries to confirm final diagnosis.
The embolization was performed from the femoral artery approach.
In 12 patients we used microspirals,
in 2 cases flow-diverting stents,
and in 1 patient liquid adhesive cyanoacrylate (LAC) was used.
Nine patients underwent single embolization procedure,
and in 3 cases the reembolization was necessary.
One patient with bilateral fistula underwent 4 embolizations.
The result of embolization was selective occlusion of carotid-cavernous fistula in 12 patients,
who underwent 18 procedures altogether.
In one case the decision was made to occlude the main trunk of internal carotid artery with embolization coils due to the size of fistula (impossible localisation of the fistula entry),
no blood flow in the distal part of internal carotid artery (ICA) and clinical signs of ischemic stroke in this part of brain.