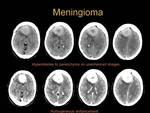
Meningiomas are slowly growing,
well–circumscribed lesions.
Due to their indolent course,
they are often large at the time of presentation.
Meningiomas are extra-axial lesions.
It does it means that it is outside the brain because the lesion derives from the lining of the brain or surrounding structures.
There are some signs that indicate that the lesion is an extra-axial tumor.
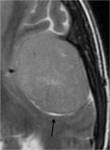
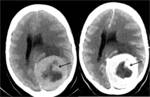
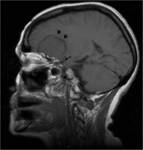
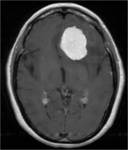
- CSF cleft : a cleft has been regarded as representing a thin rim of CSF (as seen around the posterior edge of the lesion).
High T2WI signal.
(Figure 1)
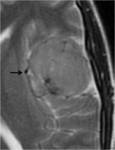
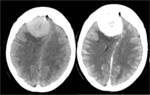
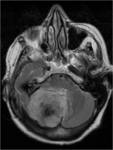
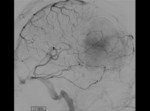
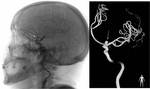
- Displace subarachnoid vessels: the vessels that run on the surface of the brain are displaced by the lesion (Figure 2)
- There is gray matter between the lesion and the white matter
- The subarachnoid space is widened because growth of an extra-axial lesion tends to push away the brain.
- Broad dural base or a dural tail of enhancement
- Bony changes
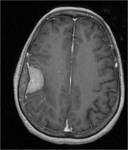
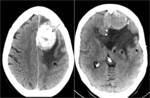
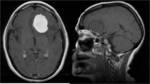
A characteristic imaging feature of meningiomas is the "dural tail." The dural tail represents the dural extension of the lesion which is seen to enhance homogeneously upon the administration of intravenous contrast.
It is not specific for meningiomas as it may be seen with other lesions.
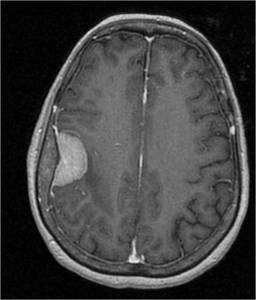
Fig. 3: Axial enhanced T1WI. Meningioma with dural tail, hyperostosis and enhancement of adjacent bone. Typical signs of an extra-axial tumor.
References: Department of Radiology, Hospital Clinico Lozano Blesa. Zaragoza/Spain 2012
TECHNIQUES AND IMAGING FINDINGS
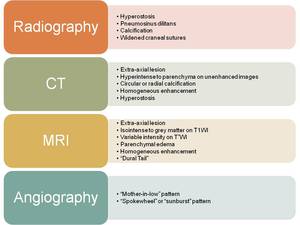

Fig. 4: Imaging Findings
References: Department of Radiology, Hospital Clinico Lozano Blesa. Zaragoza/Spain 2012
Conventional radiographs have a very limited role in the current evaluation.
Osseous changes as hyperostosis are seen with meningiomas.
Other findings in plain films are calcifications,
pneumosinus dilatans or widened cranial sutures.
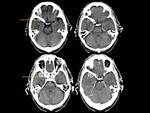
CT scan is often the first modality employed to investigate neurological signs or symptoms.
It is the principal technique used by radiologists in the emergency service.
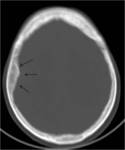
CT scan demostrates the bone hyperostosis,
which may be difficult to appreciate on MRI.
(Figure 5)
Non-enhanced CT scan demonstrates an extra–axial mass which is most frequently hyperdense to underlying parenchyma,
but it may be also iso or hypodense.
Calcification may be seen within the mass in either a circular or radial pattern.
In some cases,
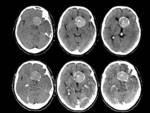
we can find a central area of high attenuation due to an acute intralesion hemorrhage or a central area of low attenuation due to necrosis (Figure 6).
Parenchimal edema sourrounding the lesion can also be identified (Figure 8).
Contrast enhanced CT scan demonstrates a brightly and homogeneously enhancing lesion.
Heterogenous enhancement is possible,
but very unusual.
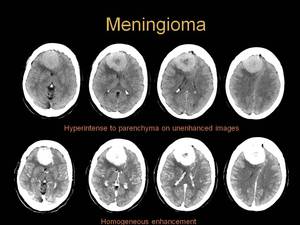
Fig. 9: CT characteristics of meningioma
References: Department of Radiology, Hospital Clinico Lozano Blesa. Zaragoza/Spain 2012
When appearances and locations are typical,
diagnosis can be made with a very high degree of certainty.
In many instances however the appearances are atypical.
Meningiomas typically appear as extra-axial masses with a broad dural base.
They are usually homogeneous and well circumscribed,
although many variants are encountered.
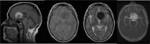
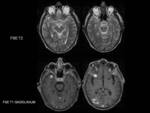
They are isointense relative to grey matter on T1 weighted images (Figure 10),
have variable intensity on T2 weighted images (ranging from iso to hyperintense) (Figure 11) and we identify the parenchimal edema with inversion recovery sequences (Figure 13).
It can be also hypointense on T2 due to a fibrocollageneous matrix or calcifications.
Cortical buckling is one of the most valuable imaging feature for identifying meningiomas on unenhanced images.
With the administration of gadolinium (Figure 14),
MR enhanced images demonstrate markedly homogeneous enhancement of the mass.
MRI shows the “dural tail”,
thickening of the dura mater that resembles a tail extending from a mass and which enhance homogeneously upon the administration of intravenous contrast.
As it has already explained,
this sign is not specific of meningiomas,
and it has been reported in various nonmenigioma tumors or tumefactive processes (chloroma,
primary central nervous system lymphoma,
sarcoidosis,
vestibular schwannoma,
metastatic tumor,
syphilitic gumma,
and an aggressive papillary middle ear tumor)
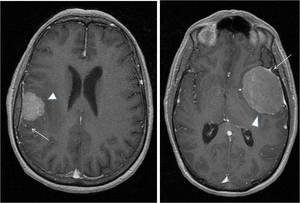
Fig. 15: Axial T1-weighted spin-echo MR image of the brain with intravenous gadolinium enhancement shows dural tail (arrow) attached to a typical
meningioma (arrowhead).
References: Department of Radiology, Hospital Clinico Lozano Blesa. Zaragoza/Spain 2012
The most characteristic vascular finding of a meningioma is a contribution to the blood supply of the neoplasm by branches of the external carotid system.
Whenever it is possible to show that the external carotid artery shares in the blood supply of an intracranial tumor,
it is most likely to be a meningioma.
There are three signs that all radiologists should know:
- Mother in law sign: it is a lesion that enhance early during the arterial phase and remain opacified well after the venous phase.
The joke is that a mother in law comes early and stays late.
(Figure 16)
- Spokewheel or sunburst pattern: this is due to a radial distribution of the small arterial branches which seem to spring from a central point.
This point probably represents the original site from which the blood supply was drawn at the beginning of the growth of the tumor.
- The venous blush: Usually the vessels that supply meningiomas can be seen in the angiogram,
but sometimes they cannot,
and only a large area of abnormal density can be identified.
DIAGNOSTIC PITFALLS
Sometimes it is not easy to diagnose a meningioma tumor with the imaging findings.
- In our institution,
the principal difficulty to diagnose meningioma tumors is to do differential diagnosis with trombosed aneurysm.
(Case 1 and 2)
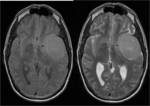
Thrombosed aneurysms are of high attenuation,
sometimes with peripheral calcification.
Diagnosis is confirmed when there is dense central enhancement after contrast administration.
The clearly demarcated slightly increased attenuation and marked total enhancement of a patent aneurysm,
is also generally appreciated but sometimes it is not easy.
Radiologists should analize the imaging appearance of the lesion and if it is not clear,
they should lead on to angiography.
It is important to recognice an aneurysm because failure to appreciate it pre-operatively is potentially dangerous.
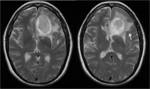
- Another difficulty was to differenciate extra-axial versus intra-axial lesions.
(Case 3)
The differentiation between intra-axial versus extra-axial is usually straight forward,
but sometimes it can be very difficult and imaging in multiple planes may be necessary.
(Case 4)