All the patients had persistent orthostatic headache,
which did not improved with conventional analgesic treatment,
with nausea and vomiting,
without any other symptoms or neurological signs on physical examination.
Two patients didn´t have any pathologies in their medical history.
One patient suffered a severe head injury in childhood,
that required surgery by multiple brain hematomas,
another patient had undergone lumbar puncture in last two weeks,
but his headache had started before to the puncture and the last patient had a history of the epidural anesthesia three weeks before.
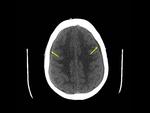
Two of the five patients had normal cranial CT and the other three had frontal and parietooccipital subdural collections left (Fig. 1 ).
In two of the three showed the presence of effacement of the basal cisterns,
as a sign of downward transtentorial herniation (Fig. 2 ).
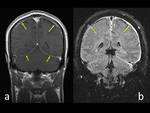
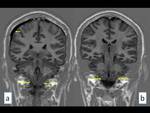
The main findings of MRI were: diffuse dural thickening in both convexities,
tentorium and falx,
which showed enhancement with intravenous contrast medium administration,
without involvement of the leptomeninges (Fig. 3 ).
In two patients this thickening extended into the spinal canal.
In one of the patients was identified discrete posterior parietal dural hyperintensity on T1 suggesting minimal hemorrhagic transformation subdural collection.
Dural venous engorgement was visualized in one patient (Fig. 4 ) and 2 had effacement of the cisterns of protuberance and descent of the cerebellar tonsils (Fig. 5 ).
Ballooning was identified only in the pituitary gland in one case.
In the three patients,
spine MRI showed dural thickening and epidural CSF collections in the lumbar,
dorsal and cervical level.
(Fig. 6 ).
One patient had paraspinal and retroperitoneal collections and another had bilateral pleural effusion,
in both cases thev presence of CSF leakage through the dural fistula was viewed (Fig. 7 ).
We didn´t identify meningeal diverticula or syringomyelia in any case.
CT myelography was performed in 3 patients,
finding extravasation of contrast medium subdural and epidural space as indirect sign of fistula (Fig. 8 ) and the fistula was identified in two of them,
one in dorsal region (Fig. 9 ) and lumbar another location.
Myelo-CT wasn't performed in two patients because the headache was associated to lumbar puncture and they improved with conservative treatment.
Three of five patients received conservative treatment with good response.
The other two patients who did not respond to initial treatment,
were underwent lumbar epidural patch of autologous blood at levels L2-L3 and L3-L4 with 5-10 cc,
showing improvement of symptoms within 24 hours of treatment,
without no complications (Fig. 10 ).
All patients fulfilled the diagnostic criteria and had a good response to treatment,
except one who was readmitted a month later by headache and epidural patch was necessary by persistent symptoms and positive findings in MRI as dural thickening,
epidural collections spinal and pleural effusion unchanged.
MRI control were performed to 3 patients after 1 and 3 months (Fig. 11 ,Fig. 12 ) with persistent subdural collections to a lesser extent (Fig. 13) and evidence of improvement or resolution of dural thickening .