Keywords:
Acute, Contrast agent-intravenous, MR, Echocardiography, CT, Emergency, Contrast agents, Cardiac
Authors:
S. K. Ternovoy, T. N. Veselova, I. Merculova, M. Y. Ruda; Moscow/RU
DOI:
10.1594/ecr2013/C-1569
Methods and Materials
In study were included 117 patients with first AMI (111 male,
6 female,
age 55,4±10,1 years).
Two-phase contrast-enhanced ECG-gated MDCT was performed using a 64-slice MDCT scanner (Aquilion 64; Toshiba Medical Systems Corporation,
Otawara,
Japan),
which is a
640.5 mm collimation scanner with a gantry rotation speed of
400 ms/rotation.
Scanning was performed at 120 kV and 400 mAs,
and the table feed was 6.4 mm/gantry rotation with a beam pitch of
0.2 The acquisition protocol included both early (arterial) and delay phases acquisition.
In arterial phase MDCT were evaluation myocardial perfusion defect (sm3),
end-systolic,
end-diastolic volume (ESV,
EDV) and ejection fraction (EF) of LV.
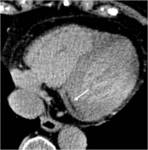
Delay phase acquisition was performed 7 minutes after this first-pass acquisition for analysis of the delayed enhancement patterns. In delay phase we detected 3 types of contrast enhancement of infarct zone:
type I — subendocardial residual defect (RD)(fig.1);
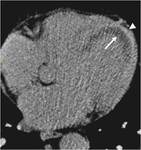
type II — myocardial contrast delayed hyperenhancement (DHE) with RD (fig.
2);
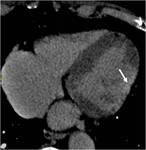
type III — transmural DHE (fig.3).
The absence of hyperenhancement in delay phase MDCT has been related to viable myocardium (1-3).
Patients were divided in 3 groups: Group 1 — with subendocardial RD (n=63); Group 2 — with DHE+RD (n=28); Group 3 — with transmural HDE (n=26).
LV remodelling was defined as an increase in LVEDV of ≥20% at 12 months after infarction compared with that based on measurements in individual patients (4).
64-MDCT with contrast enhancement was performed in all patients within 3-5 days (two-phase) and at 12 month after AMI (only early-phase).