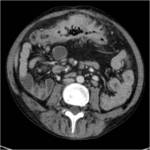
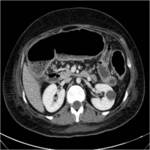
Ischemic Colitis:
Ischemic colitis results when blood flow to the colon is compromised.
Clinical situation associated with nonocclusive ischemic colitis include hemorragic or septic shock,
heart failure with low cardiac out put and use of pressor drugs such as digitalis.
Colonis ischemia can also result from occlusion of the mesenteric vasculatura by a thrombus,
embolus,
or invasive tumor.
Both arterial and venous occlusion can result in colonic ischemia.
Another variety is stercoral colitis.
In this case,
ischemia is mainly localized in the rectum due to fecal impaction evolving to chronic overinflation of the lumen and eventualy leading to necrosis.
Ischemic colitis can be diffuse or segmental.
Watershed areas of the colon (the splenic flexure and rectosigmoid) are particularly suceptible to ischemia due to hipovolemia.
The left colon ischemia is typical of elderly patients with hypoperfusion,
while the right colon is more characteristic of young people as a complication of hemorrhagic shock after penetrating trauma.
CT is one of the preferred techniques for the diagnosis of ischemic colitis.
Among the findings,
we can include circumferential wall thickening of the colon and submucosal edema,
the "target sign",
which consists of the mucosal enhancement with submucosal edema.
The inflammatory changes in the pericolic fat may also be present,
and in case involving occlusive ischemia,
CT can often demostrate thrombus whitin the splanchnic vessels or invasion of vessels by tumors such as pancreatic cancer.
Another finding of ischemic colitis or pneumatosis is bleeding in the intestinal wall,
although this is not pathognomonic of ischemic colitis.
We can also find air in the mesenteric vessels and portal vein,
this being a finding that confers a poor prognosis.
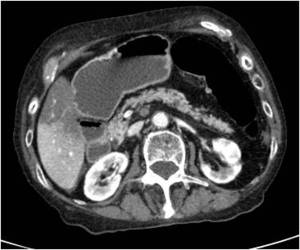
Fig. 1: CT scan obtained with intravenous contrast shows a thrombus in superior mesenteric artery, which is producind ischemic colitis.
Crohn disease:
Crohn disease is an inflammatory entity that can affect the entire gastrointestinal tract,
from the mouth to the anus.
Characterized by transmural bowel involvement and alternating with regions affected regions respected,
includng the terminal ileum in the majority of cases.
Inflammatory lesions cause mural thickening and ulcerations that create available typical cobblestone pattern described in barium studies.
In CT-can we can read the "target sign",
which consists of the mucosal enhancement with submucosal edema,
and the "sign of the comb",
which is caused by the engorgement of the mesenteric vessels.
The most common complications that can occur are fistulas,
strictures and abscesses.
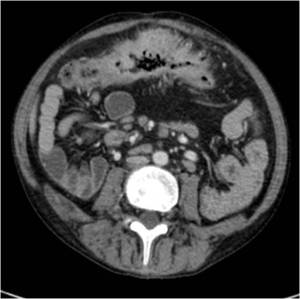
Fig. 2: Crohn disease in a young man. CT scan obtained with intravenous contrast shows the important wall tickening with narrowing of the bowel lumen and the "sign of the comb" of the mesenteric vessels.
Ulcerative Colitis:
Ulcerative colitis is an inflammatory process affecting surface colonic mucosa.
The rectum is affected in 95% of cases,
with a variable degree of affectation and circumferentially along the proximal intestine.
This is usually a pancolitis,
and in a minority of patients may also be involvement of the terminal ileum (edema without ulceration,
which differentiates it from Crohn's disease).
Colonoscopy is the primary diagnostic tool,
so it is rarely diagnosed with barium enema,
but in these cases a pattern with small granular mucosal ulcerations that capture barium can be seen.
In CT,
the wall thickness is less marked than in Crohn disease,
since inflammation is transmural.
The "halo sign",
a low-attenuation ring in the bowel wall due to deposition of sibmucosal fat, is more common in ulcerative colitis than Crohn's disease.
We can also find the presence of inflammatory pseudopolyp made of the confluence of healthy mucosa between ulcers.
Colorectal carcinoma occurs most frequently in patients with ulcerative colitis than in Crohn's disease.
Toxic megacolon is among its most serious complications.
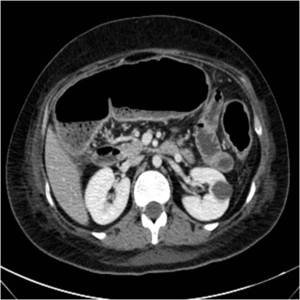
Fig. 3: Young woman with abdominal pain and diarrhea. CT scan obtained with intravenous contrast shows mucosal enhancement and colon distention. Ulcerative Colitis was diagnosed in a second time by colonoscopy.
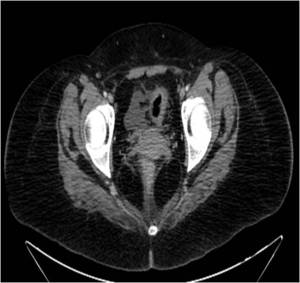
Fig. 4: CT scan obtained with intravenous contrast in the same patient shows the "halo sing" and a small pericolic fluid collection in the same patient. Notice the diffuse involvement of the colon.
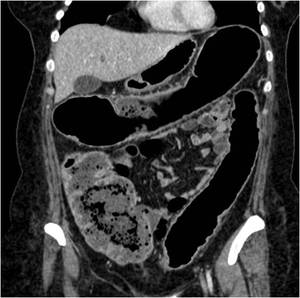
Fig. 5: Coronal reconstructions shows the disaperance of the colon normal morphology in Ulcerative colitis.
Pseudomembranous colitis:
Pseudomembranous colitis is produced by Clostridium difficile enterotoxin in patients following antibiotic treatment,
often clindamycin,
although it has been described in association with ampicillin,
amoxicillin,
cephalosporins and imipenem,
and occasionally to cytostatics.
Its distribution is usually pancolonic,
although it may affect the left or right colon.
One of the most striking findings is the large mural thickening of this entity,
the greatest of all the types of colitis,
in contrast to the low pericolonic inflammation.
The CT scan shows large mucosal enhancement with fibrinous plaques and detritus,
its polypoid-like aspect confers it a distinctive look and large submucosal edema.
In studies with oral contrast,
we observedthe so-called "accordion sign" it is the entrapment of some amount of barium between the folds of the colon thickened,
giving an appearance similar to an accordion.
The most common complications of this entity are toxic megacolon and perforation.
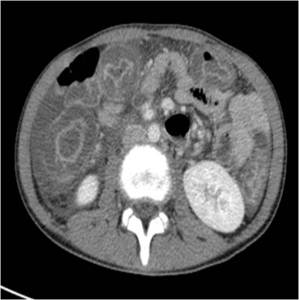
Fig. 6: CT scan obtained with intravenous contrast in a patient with chemotherapy tratment shows large mucosal enhancement with polypoid-like aspect and large submucosal edema.
GVHD:
GVHD is a process that occurs after the transplantation of a non-identical donor bone marrow because the transplanted immune cells recognize the host tissues as foreign,
so that an immune response occurs.
This reaction of the recipient to the donor's cells is classified into two types:
- Acute: When occurs during the first 100 days.
- Chronic: When it happens after 100 days.
The clinical manifestations are diverse,
affecting skin,
where it produces a maculopapular rash; liver,
studying with increased conjugated bilirubin and alkaline phosphatase; the gastrointestinal tract,
causing watery diarrhea or blood type and abdominal pain; the hematopoietic system,
producing anemia or thrombocytopenia; or kidney,
where it produces a nephrotic syndrome.
In the CT study we will see a moderate thickening of the colon wall,
mucosal and dilated bowel loops (which may be greater than 3 cm in small bowel and greater than 8 cm in colon).
In addition,
there is plenty of liquid content in the intestinal lumen.
But we must not forget that in this case,
the key fact that leads to the diagnosis is the antecedent of TPH.
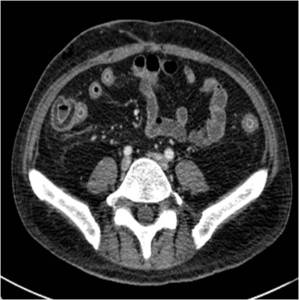
Fig. 7: CT scan obtained with intravenous contrast in a patient wiht antecedent of TPH shows moderate thickening of the right and left colon wall and mucosal enhancement.
Diverticulitis:
Acute diverticulitis occurs When the neck of diverticulum is swollen or occluded by food particules,
resulting in a microperforation.
Usually,
it sits on sigmoidal area but it may take place at any other location of the colon.
For the diagnosis of diverticulitis,
the CT-scan is the method of choice,
since we can evaluate-the wall of the colon as well as the surrounding pericolic fat.
In CT-scan,
diverticulitis appears as segmental wall thikening and hyperemia with inflammatory changes in the poericolic fat and adjacent liquid or intramural abscess.
The most frequent complications are fistulae,
abscesses,
peritonitis,
intestinal obstruction and portal vein thrombophlebitis.
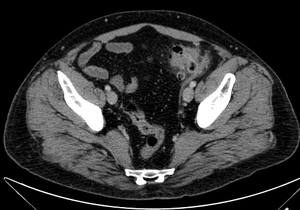
Fig. 8: CT scan obtained with intravenous contrast shows segmental wall thikening with inflammatory changes in the poericolic fat in a uncomplicated diverticulitis.
Infectious Colitis:
There are many causes of infectious colitis because there are a lot of bacteria,
fungi and virus that affect the colon.
Normally,
the infectious colitis are typically diagnosed clinically but,
sometimes,
CT is required to rule out other causes.
Usually,
in patients with infectious colitis,
CT shows wall thickening which demonstrates homogeneous enhancement.
Ascites or inflammation of the pericolic fat may also be present.
In addition,
the portion of colon affected may suggest a specific organism.
Shigella and Salmonella normally are limited to the right colon,
cytomegalovirus and E coli can produce diffuse involvement,
gonorrhea,
herpesvirus,
and C trachomatis typically involve the rectosigmoid and schistosomiasis is usually confined to the descending and sigmoid.
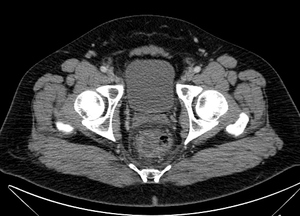
Fig. 9: CT scan obtained with intravenous contrast shows wall thickening and mucosal enhancement confined to the rectum and inflammation of the pericolic fat in the context of infectious colitis.