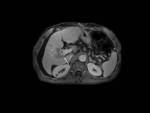
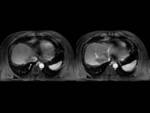
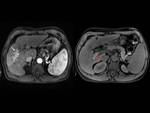
We reviewed 17 patients who had at least one hepatic DCE-MRI and who were diagnosed as diffuse HCC.
A 1.5 tesla MRI was used to perfom exams.
Standard Liver MRI protocol in our institution is detailed in Table 1.
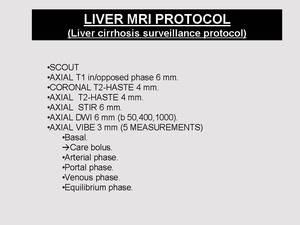
Table 1: LIVER MRI PROTOCOL IN OUR INSTITUTION
US FINDINGS
14 patients had a previous US liver study performed.
None of them were diagnosed,
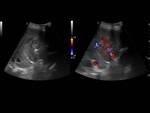
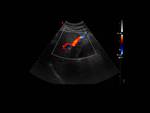
but in 2 of them diffuse hepatocellular carcinoma were suggested due to portal vein thrombosis (Fig. 1)(Fig. 2).
Metastasis or classic HCC was reported in 7 patients and no suspicious lesions were seen in the rest of them.
CT FINDINGS
13 patients also underwent an abdominal contrast-enhanced abdominal CT.
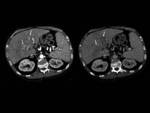
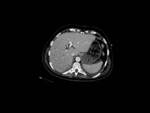
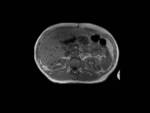
In 8 of them diffuse hepatocellular or multicentric HCC were reported (Fig. 3)(Fig. 4).
4 studies didn’t find liver lesions or indirect signs were not conclusive.
MRI FINDINGS
MR findings were consistent or at least highly suspicious of diffuse hepatocellular carcinoma and in our 17 patients the radiological final report pointed to this diagnosis.
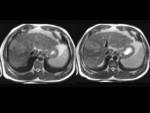
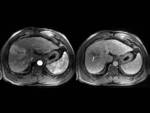
On T2- weighted images the tumours were seen mildly hyperintense in 13 patients (Fig. 5),
heterogeneously hyperintense in 3 patients and isointense-lightly hyperintense in 1 patient.
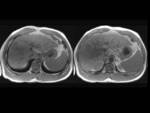
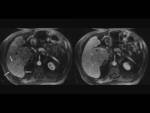
Unenhanced T1- weighted images demonstrated homogeneous hypointensity in all patients (Fig. 6) but one,
who was described as subtle heterogeneous (Fig. 7).
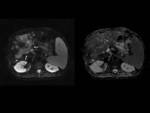
In all patients who had a DWI sequence performed (6 of them) an increased signal on diffusion-weighted images with corresponding low signal on apparent diffusion coefficient (ADC) map were manifested in both the suspected area of diffuse involvement and if some cases within the malignant portal vein thrombus (Fig. 8).
At dynamic study with gadolinium, the two main enhancement patterns already described in previous literature were found.
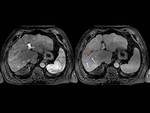
In 13 patients a geographic or patchy enhancement was found (Fig. 9),
with a more variable arterial phase that ranged from early and highly wash-in pattern to more subtle inhomogeneous enhancement and a constant heterogeneous wash-out in portal and delayed phase.
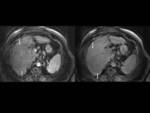
3 patients had a miliary enhancement pattern of the area involved with diffuse hepatocarcinoma (Fig. 10),
with a heterogeneous widespread of nodular arterial wash-in and more variable findings in portal and delayed phase.
One of the patients showed a lack of the expected typical wash-out (Fig. 11).
And another one of the subjects,
had a poorly focal arterial enhancement with non characteristic wash-out (Fig. 12).
Portal vein thrombosis was present in 12 patients (Fig. 13) and 1 patient had an inferior vena cava and right hepatic vein thrombosis (Fig. 14).
In most of these cases the extension of the thrombi involved right portal vein or both left and right portal veins.
The characteristics of portal vein thrombus were consistent with tumoral type in all of them,
with gross distension of the portal vein and significant neovascularization of the thrombi.
In fact,
MR findings in tumoral portal vein thrombosis were similar to those found in parenchymal mass (T2-weighted hyperintensity,
restriction on DWI and enhancement in dynamic study).
3 patients had also bland thrombi mixed with tumoral thrombi (Fig. 15).
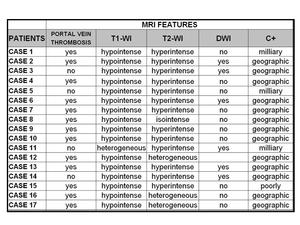
Table 2: MRI FEATURES
CLINICAL FEATURES
All our patients had already been diagnosed as cirrhotic.
8 of them were infected with hepatitis C virus (HCV) and 1 suffered from hepatitis B infection.
No co-infections of both viruses were found. 8 were negative for hepatic virus and 2 patients had no available data on their electronic medical records.
The associated alpha fetoprotein (AFP) levels in our group of patients ranged from 1.6 ng/ml to 494.613 ng/ml.
These findings are in consonance with recent literature reviews that conclude AFP levels are quite variable among patients with diffuse subtype of hepatocellular carcinoma.
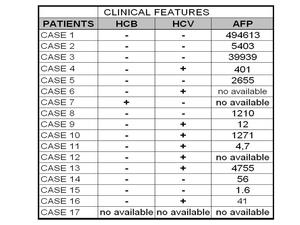
Table 3: CLINICAL FEATURES
The histopathological confirmation of all the 17 patients who were diagnosed as diffuse hepatocarcinoma was not obtained.
In some cases the diagnosis was based on the typical clinical,
radiological and laboratory findings.
Biopsy proof of tumour within the liver was available for 7 patients.
The other patient who also had a fine needle aspiration biopsy had a non conclusive anatomopahological report.