CLINICAL FEATURES
The clinical presentation of PRES is very broad and includes headaches,
confusion,
nausea and vomiting,
generalized seizures sometimes with status epilepticus,
cerebellar syndrome,
cortical blindness,
hemianopsia,
blurred vision,
hemiparesis,
coma and others.
These symptoms may develop over several days or may be recognized only in the acute setting.
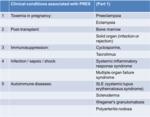
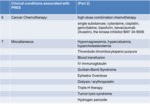
Certain clinical conditions have been established as risk factors for the development of PRES (Table 1):
-Hypertension was the first condition who was described as a factor that promotes the development of PRES (hypertensive encephalopathy).
It is present in 70 to 80% of cases.
-Eclampsia or pre-eclampsia has always been linked to PRES,
even in women with blood pressure within normal limits (20 to 30% of cases).
The development of hypertension in preeclampsia is related to systemic vasoconstriction associated with intravascular volume depletion and hemoconcentration and is more frequent in the delayed form in postpartum.
-Also has been seen in chemotherapy regimens and organ transplants that require the use of immunosuppressive drugs especially in allogeneic bone marrow transplantation.
- Severe Sepsis and multiple organ failure.
-Chronic renal failure and dialysis.
-Autoimmune diseases such as lupus erythematosus,
scleroderma,
Wegener's granulomatosis,
and others.
The syndrome has developed even in periods when the patients were not being treated with immunosuppressive drugs.
IMAGING FEATURES
PRES CT and MR images are characterised by abnormalities of the white matter and the grey matter,
predominantly affecting the posterior regions.
The parietal and occipital lobes are most commonly affected,
followed by the frontal lobes,
the inferior temporal-occipital junction,
and the cerebellum.
A bilateral and symmetrical appearance is highly typical although lesions can be asymmetrical in some cases.
On CT we can observe difusse hypodense areas that indicate the affected regions.
On MRI,
patchy confluent cortical / subcortical lesions appear iso-intense or low signal intensity on T1-weighted images and hyperintense on T2-weighted images and in FLAIR sequence,
distributed in superficial and deep border territories.
Enhancement is not usually seen after injection of a contrast agent.
There are three variants of hemispheric patterns:
1.
Holohemispheric: Vasogenic edema affecting all lobes,
separating the medial vascular regions of the anterior cerebral artery and posterior cerebral artery from the lateral vascular regions of the middle cerebral artery.
2.
Superior frontal sulcal.
3.
Primary parietal-occipital.
Partial,
asymmetric,
or mixed forms of these patterns may be encountered.
ATIPICAL IMAGING FEATURES
Some atypical findings on CT and MR have been described,
including extension of lesions to the basal ganglia and the brain stem and the deep white matter,
in particular the splenium of the corpus callosum.
In some cases the condition may be unilateral which requires a high level of suspicion.
Severe cases can cause progressive dysfunction of cerebrovascular regulatory mechanisms altering the permeability of the blood-brain barrier.
In these cases MRI with gadolinium injection shows enhancement on T1-weighted images.
We can also find diffusion restriction,
infarction,
cytotoxic edema and hemorrhage that may manifest as focal hematoma or subarachnoid hemorrhage.