Hypointensity on FLAIR images has been described as part of some infectious diseases,
during several inflammation processes,
or in the lesions with water,
lipid or paramagnetic substances content.
Several brain tumors may demonstrate characteristic hypointense FLAIR signal,
including meduloblastoma,
rarely lymphoma,
but also some types of cortical tubers.
Inherited metabolic disorders,
like adrenoleukodistrophy,
may also present with the central zone low signal intensity within the affected white matter.
However,
it is also observed that in the pediatric patients during the normal myelination process the white matter signal is usually relative hypointense to adjacent gray matter on FLAIR images and should not be misdiagnosed as pathological finding.
This educational exhibit describes several important “dark objects” on FLAIR images.
1.
Enlarged perivascular space
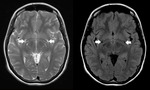
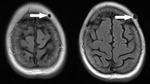
Enlarged perivascular spaces,
Virchow-Robin (VR) spaces,
even are not in direct connection with the subarachnoidal space,
they have identical MRI appearance like cerebrospinal fluid (CSF) on all pulse sequences.
However,
when signal intensities are measured,
the VR spaces prove to have significantly lower signal intensity than the CSF-containing structures within and around the brain,
a finding consistent with the fact that the VR spaces represent entrapment of interstitial fluid (2).
Fig. 1
2.
“Black hole” - Multiple sclerosis (MS)
Black holes are chronic MS lesions with T1 hypointesity.
Those lesions are focal areas of relatively sever tissue injury,
and show FLAIR hypointensity.
Fig. 2
3.
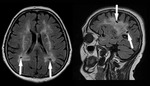
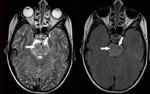
Paramagnetic substances
Various paramagnetic substances induce FLAIR hypointensity.
Some of the most often are blood products.
Fig. 3
Fig. 4
4.
Lipid content - atheroma and colloid cyst
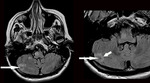
Atheromas,
a benign tumor-like lesions in subcutaneous tissue,
have typical MRI appearance because of high lipid content.
Fig. 5
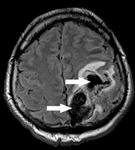
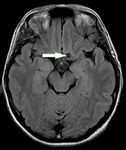
Colloid cyst is rare benign tumor usually locate in anterior part of the third ventricle.
Imaging features of colloid cysts is well known.
MR appearance of colloid cyst may change,
depending on the protein and lipid contents of the cyst and not on the presence of paramagnetic
minerals (3).
Cysts that are rich in cholesterol tend to be hypointense on T2W and FLAIR images and hyperintense on T1W images.
Fig. 6
5.
Post-operative materials
Commonly used embolization coils are either nonferromagnetic or weakly ferromagnetic.
Platinum embolization coils produce magnetic susceptibility artifact and MR image quality may be compromised in the area of interest.
Platinum coils are visible like FLAIR “dark objects” and should not be misdiagnosed.
Fig. 7
6.
Atypical infections
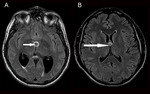
In some atypical brain infections there are lesions,
usually multiple focal lesions,
with mild T2W and FLAIR hypointensity or “intermediate” SI.
There are several reasons for this appearance.
In tuberculosis it is because of caseous material.
In fungal infections due to absence of pus,
there is increased concentration of paramagnetic ions.
Toxoplasmosis may show “eccentric target”.
Typically,
it is described like postcontrast T1W “eccentric target” sign,
highly suggestive of toxoplasmosis,
but relative insensitive,
being seen in less than 30%.
But,
there is also T2W and FLAIR “target” sign.
If it’s solitary lesion in patient with HIV/AIDS then it’s more often lymphoma than toxoplasmosis,
which also can show T2W/FLAIR hypointensity or “intermediate” SI (4).
Fig. 8
7.
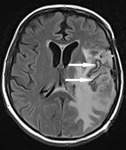
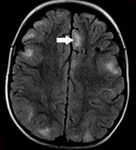
Inflammation/ demyelination
MRI has been used as the principal investigation for detection of white matter lesions in demyelinating diseases.
It helps in making difference between acute disseminated encephalomyelitis (ADEM) and multiple sclerosis.
Extensive demyelination process sometimes can show T2W and FLAIR hypointensity.
This case represents 10-year-old girl with recidivant ADEM.
Fig. 9
8.
Cortical tuber
In tuberous sclerosis complex cortical tubers is very often imaging findings.
Three types of tubers were identified based on the MRI SI of their subcortical white matter component.Tubers Type A are isointense on volumetric T1W images and subtly hyperintense on T2W and FLAIR.
Type B are hypointense on volumetric T1W images and homogeneously hyperintense on T2W and FLAIR.
Type C are hypointense on volumetric T1W images,
hyperintense on T2W,
and heterogeneous on FLAIR characterized by a hypointense central region surrounded by a hyperintense rim (5).
Fig. 10
9.
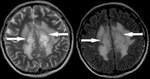
Adrenoleukodystrophy
In cerebral X-linked adrenoleukodystrophy (X-ALD),
three different pathological zones (Schaumberg’s zones) are described in affected white matter.
The central or inner zone appears moderately hypointense at T1W MR imaging and markedly hyperintense at T2W.
This zone corresponds to irreversible gliosis and scarring.
The intermediate zone represents active inflammation and breakdown in the blood-brain barrier.
At T2W MR imaging,
this zone may appear isointense or slightly hypointense and readily enhances after intravenous administration of contrast material.
The peripheral or outer zone represents the leading edge of active demyelination; it appears moderately hyperintense at T2W MR imaging and demonstrates no enhancement (6).
White matter injury in the intermediate and outer zone may be reversible and has been the prime target for therapeutic intervention.
Combination of T2W and FLAIR images may determine irreversible and potentially reversible pathological zones.
Fig. 11
10.
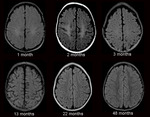
Normal myelination process
FLAIR imaging is important in differentiating pathological processes from normal myelination in routine pediatric brain MR studies.
In the deep cerebral hemispheric white matter,
FLAIR images show a triphasic sequence of signal change relative to adjacent gray matter not seen on T1- or T2W images.
White matter on FLAIR images converts from hyperintense to hypointense relative to adjacent
gray matter during the first 24 months of life.
The white matter signal change from hyperintense to hypointense relative to adjacent gray matter on FLAIR images occurs slightly later than the analogous change seen on T2W images.
This delay most likely reflects the T1 sensitivity of FLAIR imaging (7).
Fig. 12