Retrospective study (January - August 2012) of patients who underwent lower extremity CTA and DSA at our institution.
CTA protocol
CT angiography was performed with a 64–detector row unit (Lightspeed VCT; GE Medical Systems,
Milwaukee,
Wis),
from 2 cm above the origin of the celiac trunk to the foot (105-130m),
by using the following parameters: collimation,
0.625 X 64 mm; gantry rotation,
0.6-0.8 second; pitch,
1; noise índex,
32; scan duration,20–35 seconds.
Contrast enhancement was achieved with intravenous injection of 125 mL of nonionic iodinated contrast medium (iomeprol,
320 mg of iodine per milliliter [Iomeron; Bracco,
Milan,
Italy])after an injection of 30 mL of saline solution at a flow rate of 3,5-4 mL/sec.
Scan delay was individually determined by using bolus-tracking software (Smart-Prep,
GE Medical Systems).
The scanning began 8 seconds after a threshold attenuation of 150 HU was reached in the abdominal aorta superior to the level of the renal arteries.
CT angiographic data sets were transferred to a dedicated GE workstation for post processing.
Reconstructed three-dimensional images included maximum intensity projections (MIP),
volume-rendered images,
and curved multiplanar reformations along the longitudinal axis of the artery.
DSA protocol
Conventional DSA was performed in the cases where endovascular revascularization was indicated.
The therapeutical procedures took place during the same session using one standard angiographic unit (Innova 4100,
GE Medical Systems,
Milwaukee,
Wis).
An interventional radiologist with 7 years of experience in vascular and interventional procedures performed intra arterial DSA after catheterization through a femoral artery access.
An iodinated contrast agent (iomeprol,
320 mg of iodine per millilitre Iomeron; Bracco,
Milan,
Italy]) was administered through a 4F sheath when an anterograde puncture was performed (below the knee revascularization) or trough a 4F pigtail when a retrograde puncture was performed (contra-lateral femoral-iliac revascularization).
Radiological anatomy of the lower limb arteries (Figures 1,
2,
3)
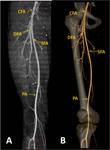
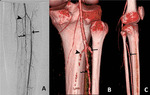
The common femoral artery (CFA) (Figure 1) begins immediately behind the inguinal ligament,
midway between the anterior superior spine of the ilium and the symphysis pubis,
and passes down the front and medial side of the thigh.
After originating the profunda femoris artery,
it is also commonly known as the superficial femoral artery.
It ends at the junction of the middle with the lower third of the thigh,
where it passes through an opening in the Adductor magnus to become the popliteal artery.
The profunda femoris artery (deep femoral artery-DFA) (Figure 1) is a large vessel arising from the lateral and back part of the femoral artery, from 2 to 5 cm.
below the inguinal ligament.
At first it lies lateral to the femoral artery; it then runs behind it and the femoral vein to the medial side of the femur,
and,
passing downward behind the Adductor longus,
ends at the lower third of the thigh in a small branch,
which pierces the Adductor magnus,
and is distributed on the back of the thigh to the hamstring muscles.
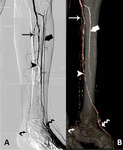
The popliteal artery (PA) (Figures 1,2) is the continuation of the femoral,
and courses through the popliteal fossa.
It extends from the opening in the Adductor magnus,
at the junction of the middle and lower thirds of the thigh,
downward and lateralward to the intercondyloid fossa of the femur,
and then vertically downward to the lower border of the Popliteus,
where it divides into anterior tibial artery and tibio-peroneal trunk.
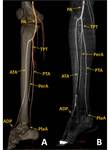
The anterior tibial artery (ATA) (Figure 2)  commences at the bifurcation of the popliteal,
at the lower border of the Popliteus,
passes forward between the two heads of the Tibialis posterior,
and through the aperture above the upper border of the interosseous membrane,
to the deep part of the front of the leg: it here lies close to the medial side of the neck of the fibula.
It then descends on the anterior surface of the interosseous membrane,
gradually approaching the tibia; at the lower part of the leg it lies on this bone,
and then on the front of the ankle-joint,
where it is more superficial,
and becomes the dorsalis pedis.
commences at the bifurcation of the popliteal,
at the lower border of the Popliteus,
passes forward between the two heads of the Tibialis posterior,
and through the aperture above the upper border of the interosseous membrane,
to the deep part of the front of the leg: it here lies close to the medial side of the neck of the fibula.
It then descends on the anterior surface of the interosseous membrane,
gradually approaching the tibia; at the lower part of the leg it lies on this bone,
and then on the front of the ankle-joint,
where it is more superficial,
and becomes the dorsalis pedis.
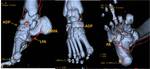
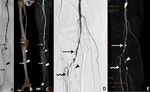
The arteria dorsalis pedis (ADP) (Fig.
3),
the continuation of the anterior tibial,
passes forward from the ankle-joint along the tibial side of the dorsum of the foot to the proximal part of the first intermetatarsal space,
where it divides into two branches,
the first dorsal metatarsal and the deep plantar.
The posterior tibial artery (PTA) (Figure 2)  arises from the tibio-peroneal trunk,
begining at the lower border of the Popliteus,
opposite the interval between the tibia and fibula; it extends obliquely downward,
and,
as it descends,
it approaches the tibial side of the leg,
lying behind the tibia,
and in the lower part of its course is situated midway between the medial malleolus and the medial process of the calcaneal tuberosity.
Here it divides beneath the origin of the Adductor hallucis into the medial and lateral plantar arteries.
arises from the tibio-peroneal trunk,
begining at the lower border of the Popliteus,
opposite the interval between the tibia and fibula; it extends obliquely downward,
and,
as it descends,
it approaches the tibial side of the leg,
lying behind the tibia,
and in the lower part of its course is situated midway between the medial malleolus and the medial process of the calcaneal tuberosity.
Here it divides beneath the origin of the Adductor hallucis into the medial and lateral plantar arteries.
The peroneal artery (PerA) (Figure 2) is deeply seated on the back of the fibular side of the leg.
It arises from the tibio-peroneal trunk,
about 2.5 cm,
below the lower border of the Popliteus,
passes obliquely toward the fibula,
and then descends along the medial side of that bone.
It divides into lateral calcaneal branches which ramify on the lateral and posterior surfaces of the calcaneus.
The lateral plantar artery (a.
plantaris lateralis; external plantar artery) (LPA) (Fig.
3),
much larger than the medial,
passes obliquely lateralward and forward to the base of the fifth metatarsal bone.
It then turns medialward to the interval between the bases of the first and second metatarsal bones,
where it unites with the deep plantar branch of the dorsalis pedis artery,
thus completing the plantar arch.
The medial plantar artery (a.
plantaris medialis; internal plantar artery) (MPA) (Figure3),
much smaller than the lateral,
passes forward along the medial side of the foot.
Imaging findings
Atherosclerosis is the predominant cause of lower extremity ischemia,
although in younger patients or in patients with atypical histories or physical findings,
non atherosclerotic diseases should be considered.
Atherosclerotic plaques commonly calcify and produce focal,
patchy,
irregular calcifications in the intima of the arterial wall.
These calcifications are easily seen on CT examinations of the extremities.
Plaques may have a wide variety of angiographic appearances,
ranging from diffuse,
relatively smooth narrowing of long arterial segments to very focal web-like lesions.
The distribution of atherosclerotic lesions in lower extremity arteries is surprisingly symmetrical in most patients.
A fairly strong correlation exists between the extent of disease and clinical presentation,
although clinical symptoms may not be a good measure of angiographic progression of disease.
Patients with claudication usually have flow-limiting vascular lesions at one level—pelvis,
thighs,
or calves—compared to patients with limb-threatening ischemia in which multiple proximal and distal arteries are involved.
Certain diseases associated with atherosclerosis have atypical and characteristic angiographic patterns of arterial involvement.
Patients with diabetes have an increased frequency and severity of symptoms related to peripheral vascular disease.
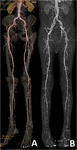
Accelerated atherosclerosis largely confined to the infrapopliteal arteries in the calf demonstrated has been demonstrated in these patients (Figure 4).
The severity of disease correlates well with the duration of diabetes,
independent of patient age.
Interestingly,
the proximal lower extremity arteries seem to be relatively spared and,
in fact,
seem to have less involvement than typical nondiabetic patients who have peripheral vascular disease,
producing the classic angiographic findings of normal proximal vessels with severe disease in the tibial and peroneal arteries.
Premature atherosclerosis is usually defined as symptomatic arterial obstruction in patients younger than 50 years of age.
It is often associated with a positive family history and may be associated with hyperlipidemia and hipercoaguable states.
As opposed to diabetic vascular disease,
premature atherosclerosis usually occurs in the proximal arteries,
mainly the distal aorta,
iliac and femoral arteries (Fig 5).
Traditionally,
pre-treatment assessment of PAD has been performed with conventional catheter angiography.
However,
conventional angiography is an invasive procedure that can have a complication rate (puncture site complication and catheter-related complications) as high as 10%.
The advent of alternative minimally invasive procedures,
such as multidetector CTA has markedly reduced the need for diagnostic catheter angiography,
effectively limiting its use to patients undergoing interventional treatment.
From our experience,
we find an excellent agreement between the CTA and DSA findings (Figures 6,7,8 and 9).
Therefore,
we confidently use CTA for diagnosis,
therapeutical decision and procedure planning.