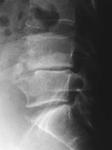
Radiographic manifestations usually appear 3 weeks to 5 weeks after the onset of clinical symptoms.
The lower lumbar spine is the preferential location.
The focal erosions of the superior or inferior vertebral body angle (brucellar epiphysitis) are characteristic of brucellosis.
(Fig.
1).
Focal anterior or diffuse disc collapse is very frequent but late and moderate.
A vacuum phenomenon may be observed,
especially in the anterior part of the disc,
possibly secondary to ischaemic changes in the disc,
with subsequent necrosis (Fig.
1) [4].
Bone destruction is less severe than in tuberculous spondylitis.
Vertebral body destruction is mild whereas condensation is early and marked.
Peri-lesional bone formation with osteophytosis and osteophyte formation at the anterior vertebral endplate (parrot’s beak) are typical (Fig.
2).
Productive bone changes occur earlier than in tuberculous spondylitis.
Because bony remodelling can progress slowly,
radiographic changes might not be easy to differentiate from those of degenerative disease.
Evidence of infective spondylodiscitis is best documented by bone scintigraphy,
CT or MR imaging [5].
Bone scintigraphy enables early and highly sensitive detection of all osteoarticular sites of the disease.
Several scintigraphic patterns can be observed.
An increased uptake limited to the anterior vertebral body angle is highly suggestive of brucellosis [4].
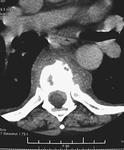
CT may be positive early in the course of the disease.
The affected disc appears hypodense.
Disc flattening and vertebral endplate destruction may be detected when plain radiographs are still negative.
(Fig.
3).
Disc gas can be detected in 25–30% of the cases [5] (Fig.
4a and b),
and is generally peripheral and of small amount.
CT after administration of contrast agent can define extension of inflammatory process and can easily diagnose paravertebral abscess with psoas involvement.
The intraspinal extent of epidural abscesses causing posterior displacement of the dural sac can be shown on post-contrast CT,
but these changes are better defined by MRI.
Extensive bone destruction is uncommun in brucellar spondylitis; however,
important bone destruction or large or calcified paraspinal soft tissue collections may be observed,
and they constitute the so called brucellar pseudo-Pott’s disease.
(Figs.
5 and 6).
MRI is the method of choice for the diagnosis,
the assessment of the disease local extension and follow-up of brucellar spondylitis.
MRI shows high accuracy for detecting the disease in the early stages and provides excellent definition of paravertebral and epidural extension.
It also allows the detection of other spinal foci [3].
In acute brucellar infections,
MRI shows low to intermediate signal intensity on T1-weighted images of the intervertebral disc and low signal intensity in the adjacent vertebral bodies.
The signals in these areas become hyperintense on T2-weighted MRI sequences,
with either a homogeneous or heterogeneous pattern.
The intravenous administration of gadolinium allows better definition of the spinal inflammatory lesions and a more complete assessment of soft tissue involvement and epidural extent (Figs.
7 and 8).
These features are best shown when fat-suppression techniques are applied to the contrast enhanced images.
Paravertebral abscesses are observed in approximately 30% of cases and are typically characterised by well-defined margins [1].
In the chronic stages,
the MRI pattern of the discs and vertebral bodies may vary.
However,
vertebral bodies usually show heterogeneous signal intensity [1–3].