Osteochondroma
Osteochondroma is the most common benign tumor of the bone.
It is a lesion composed of cortical and medullary bone with an overlying hyaline cartilage cap.
The continuity of the lesion with the underlying native bone cortex and medullary canal is pathognomonic.
The lesions may be solitary or multiple.
Solitary osteochondroma
Solitary osteochondroma is a frequent lesion (20 – 50% of benign bone tumors and 10 – 15% of all bone tumors).
Most solitary osteochondromas are asymptomatic and are found incidentally.
The most common clinical manifestation is a nontender,
painless cosmetic deformity related to the slowly growing enlarging exophytic mass.
Additional complications include osseous deformity,
fracture,
vascular compromise,
neurologic sequelae,
overlying bursa formation and malignant transformation.
Osteochondroma may arise in any bone that develops from preformed cartilage (enchondral ossification).
The most affected bones are,
in decreasing order of frequency,
the femur (30% of cases,
with distal involvement being more common than proximal involvement),
the tibia (15 – 20% of cases,
mostly in a proximal location) and the humerus (10 – 20% of cases).
Long bone lesions frequently affect the metaphysis,
with the diaphysis being a rare location.
Imaging findings
Conventional radiography
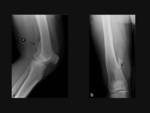
The lesion is composed of cortical and medullary bone protruding from and continuous with the underlying bone.
The areas of osseous continuity between parent bone and osteochondroma may be broad,
involving a large portion of the bone circumference (sessile osteochondroma) (Fig. 1a),
or narrow,
with a bulbous tip (pedunculated osteochondroma) (Fig. 1b).
The appearance of hyaline cartilage cap is quite variable on radiographs.
Frequently the chondroid nature of this region is suggested by the identification of arcs and rings or flocculent calcification.
The thickness of the cartilage cap is usually not well evaluated unless there is extensive mineralization.
Computed tomography
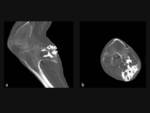
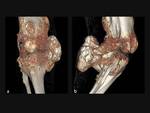
The three-dimensional imaging capability of CT often allows optimal depiction of the pathognomonic cortical and marrow continuity of the lesion and parent bone (Fig. 2 and Fig. 3).
If the cartilage cap is mineralized it is possible to measure it accurately with CT.
However,
it is very difficult to measure the thickness of an entirely nonmineralized cartilage cap because it cannot be easily differentiated from surrounding muscle or edema.
Magnetic resonance
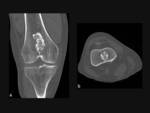
MR imaging also demonstrates cortical and medullary continuity between the lesion and parent bone (Fig. 4).
Cortical bone appears with low signal intensity in all pulse sequences,
whereas the medullary component has an appearance of yellow marrow.
MR is the best imaging modality for visualizing the effect of the lesion on surrounding structures and evaluating the hyaline cartilage cap,
allowing an accurate measurement of its thickness.
The high water content in nonmineralized portions of the cartilage cap has intermediate to low signal intensity on T1-weighted images and very high signal intensity on T2-weighted images (Fig. 5).
Osteochondromatosis
Osteochondromatosis (hereditary multiple exostosis) is an uncommon autossomal dominant disease,
characterized by the presence of multiple osteochondromas.
The estimated prevalence of disease is 1:50000 to 1:100000.
The multiplicity of lesions and associated deformity lead to early radiologic evaluation and diagnosis.
Almost every bone,
with the exception of the calvaria,
has been described as being involved in hereditary multiple exostosis.
Imaging of individual osteochondroma in osteochondromatosis is identical to that of solitary lesions.
Although some of the osteochondromas are cauliflower-like,
most are broad-base sessile lesions (Fig. 6).
Malignant transformation
Malignant transformation is the most feared complication of osteochondroma.
The prevalence of this complication is higher with multiple lesions,
occurring in 5-25% of the cases.
In solitary osteochondroma,
it occurs in 1% of the cases.
Chondrosarcoma arising in an osteochondroma accounts for 8% of all chondrosarcomas and is usually solitary,
with a low histologic grade.
Centrally located osteochondromas about the pelvis,
hips and shoulders are particularly more prone to undergo malignant transformation.
Hyaline cartilage cap thickness is an extremely important criterion in determining malignant transformation – values exceeding 2 cm in a skeletally mature patient should be viewed with great suspicion of harboring malignant transformation.
Other radiographic features that suggest malignancy include growth of a previously unchanged osteochondroma in a skeletally mature patient; irregular or indistinct lesion surface; erosion or destruction of the adjacent bone and the presence of a soft-tissue mass (Fig. 7; Fig. 8; Fig. 9).
Enchondroma
Enchondroma is the second most common benign tumor of the bone,
constituting approximately 10% of all benign bone tumors.
Although age distribution includes a wide range,
they are usually seen in patients in their second to fourth decades.
They are most frequently discovered incidentally because they are usually asymptomatic.
Otherwise pathologic fracture is the second most common manifestation.
Enchondroma are especially common in the tubular bones of the hands or feet (up to 50% occur in one of these locations).
They are also frequent in long tubular bones such as humerus,
femur and tibia.
Axial skeleton is rarely involved.
In the short tubular bones enchondromas are usually located metaphyseal or metadiaphyseal.
In long tubular bones they are mostly located centrally in the metaphyseal region but can extend into the diaphysis.
Imaging findings
Conventional radiography
In the short tubular bones enchondromas typically appear as lytic lesions with a thin sclerotic rim and a varying degree of chondrogenic calcification (“arcs and rings” calcifications) (Fig. 10).
In long tubular bones they may show as dense chondrogenic calcifications completely obscuring the underlying destruction and with no sclerotic rim,
or as sharply demarcated lytic lesions with a thin rim of sclerosis and a varying degree of chondrogenic or amorphous calcification (Fig. 11).
Computed tomography
CT allows a better assessment of cortical integrity and matrix calcifications (Fig. 12).
Magnetic resonance
Enchondroma appears as a lobulated lesion,
with high signal intensity on T2-weighted sequences,
and low to intermediate signal intensity on T1-weighted sequences.
If the amount of calcification is severe,
the MR images show low signal intensity on both T1- and T2-weighted sequences (Fig. 13).
After intravenous administration of gadolinium there is a rings-and-arcs pattern of enhancement,
showing the fibrovascular septae between the cartilage lobules.
Differential diagnosis
In the hands or feet,
if the lesion shows no matrix calcification,
the differential diagnosis includes giant cell tumor,
epidermoid inclusion cyst,
aneurismal bone cyst and fibrous dysplasia.
In these locations chondrosarcoma is rare.
In sites other than the hands or feet,
enchondroma may be confused with bone infarct (although the serpiginous pattern usually seen in a bone infarct allows differentiation) but major diagnostic consideration is low-grade chondrosarcoma.
Enchondroma versus low-grade chondrosarcoma
There is considerable histologic and radiographic overlap between enchondroma and low grade chondrosarcoma.
Chondrosarcoma can develop de novo or occur as a malignant transformation within an enchondroma or other cartilaginous tumor.
The probability of malignant transformation is greater in the case of multiple lesions (enchondromatosis).
Features that do not belong to the typical presentation of an enchondroma and should initiate further workup include:
- deep endosteal scalloping (greater than two thirds of cortical thickness) (Fig. 14);
- penetration of the cortex;
- periosteal reaction or cortical remodelling,
except for a thin neocortex;
- large size lesion (larger than 5 cm);
- enlarging lesion in skeletally mature patients;
- soft tissue mass component;
- lesion-related pain.
Enchondromatosis
Ollier disease is a rare condition in which multiple enchondromas are present,
frequently with a preference for a certain limb or for one side of the body.
The disease appears in early childhood and doesn’t have an inheritance pattern.
Radiographic morphology of single lesions of enchondromatosis is identical to that of solitary enchondromas but the frequency of lesions can lead to significant deformity (Fig. 15).
The risk of malignant transformation ranges from 10 to 25%.
Maffucci’s disease is characterized by the presence of multiple enchondromas and soft tissue hemangiomas.
Phleboliths may be present which,
in addition to the features of enchondromatosis,
help to make the radiographic diagnosis.
Secondary development of chondrosarcoma is even more frequent than in Ollier disease.
Chondroblastoma
Chondroblastoma is a benign chondrogenic tumor with a strong predilection for the epiphysis of long tubular bones and for the adolescent age group.
It accounts for less than 1% of all bone tumors.
About 75% of chondroblastomas are located in the epiphyses or apophyses of long tubular bones,
most commonly in the proximal tibia,
the proximal humerus,
the distal femur and the apophysis of the greater trochanter.
Within other localizations described,
the temporal bone,
the talus and the calcaneous are more frequent.
A few cases of malignant behavior of chondroblastoma,
with distant metastases,
have been reported.
Imaging findings
Conventional radiography
Chondroblastoma appears as a round or oval lytic lesion with sclerotic margins (Fig. 16).
About 50% of the lesions show some amount of chondroid matrix which tends to be more of an amorphous pattern instead of punctate or rings-and-arcs pattern.
It tends to be eccentrically located within the epiphysis.
Computed tomography
CT can help in detection of matrix mineralization and in assessment of the sclerotic rim (Fig. 17).
Magnetic resonance
MR is useful in the exclusion of a soft tissue component or intraarticular extension.
On T1-weighted images chondroblastoma is isointense with muscle.
On T2-weighted images the lesion shows heterogeneous intermediate to high signal intensity,
often with a lobulated pattern.
MRI also may show bone marrow and adjacent soft tissue edema (Fig. 18).
The differential diagnosis includes giant cell tumor,
abscess,
metastasis and clear cell chondrosarcoma.
Chondromyxoid fibroma
Chondromyxoid fibroma is a very rare benign cartilaginous lesion,
most frequently seen in the second and third decades of life.
Predilection sites are the metadiaphyses of long tubular bones,
mainly about the knee joint,
where about two thirds of lesion occur.
An eccentric location within the medullary canal is typical.
Imaging findings
Conventional radiography
The typical chondromixoid fibroma is a round or oval,
well-defined,
sharply marginated lytic lesion,
surrounded by a sclerotic rim.
Although this is a cartilaginous lesion,
it is rare to find calcified tumor matrix within it.
Occasionally,
matrix calcifications can be seen in a punctuate,
occulent or rings-and-arcs pattern.
Computed tomography
Computed tomography can add some information on matrix calcification and the presence of a sclerotic rim.
Magnetic resonance
The MRI appearance is nonspecific,
with low signal intensity on T1- and heterogeneous high signal intensity on T2-weighted images.
Synovial chondromatosis
Primary synovial chondromatosis is an uncommon benign neoplastic process characterized by the presence of hyaline cartilage nodules in the subsynovial tissue of a joint,
tendon sheath or bursa.
It typically affects patients in the third to fifth decades of life.
Clinical manifestations include pain,
swelling and restriction of range of motion.
The knee is the most commonly affected articulation (more than 50-65% of cases occur in that location).
Other commonly involved joints are the hip,
elbow,
shoulder and ankle.
Secondary synovial chondromatosis is associated with joint abnormalities,
such as mechanical or arthritic conditions,
that cause intraarticular chondral bodies.
Imaging findings
Conventional radiography
Radiographs reveal multiple intraarticular calcifications in 70-95% of cases of primary synovial chondromatosis (Fig. 19).
A typical chondroid ring-and-arc pattern of mineralization is common.
Fragments may also progress to further maturation and enchondral ossification,
with a peripheral rim of cortex and inner trabecular bone.
Evidence suggesting joint effusion may be seen.
The joint space is typically maintained.
Computed tomography
CT is the optimal imaging modality to detect and characterize calcifications and is particularly helpful in cases for which radiographic findings are normal or equivocal due to complex osseous anatomy.
Nonmineralized regions of synovial thickening appear as low attenuation areas (Fig. 20).
Peripheral and septal enhancement may be seen following intravenous administration of contrast material.
Magnetic resonance
On T1-weighted images synovial chondromatosis has homogeneous,
intermediate,
intraarticular signal intensity,
similar to that of muscle.
On T2-weighted images it appears with high signal intensity.
Calcifications appear as focal areas of low signal intensity with all pulse sequences (Fig. 21).
Chondrosarcoma
Chondrosarcoma is a malignant tumor that produces cartilage matrix.
The lesions that arise de novo are called primary chondrosarcomas.
Lesions arising on preexisting benign cartilaginous neoplasms such as enchondromas or osteochondromas are secondary chondrosarcomas.
Primary chondrosarcoma is one of the most common primary malignant tumor of the bone,
constituting 3,5% of all primary tumors.
The most frequent histological type,
accounting for more than 90% of chondrosarcomas,
is conventional chondrosarcoma (also called medullary or central chondrosarcoma).
Rare histological varieties include clear cell chondrosarcoma,
mesenchymal chondrosarcoma and dedifferentiated chondrosarcoma.
Conventional chondrosarcoma
Conventional chondrosarcoma frequently affects patients in their fourth to fifth decades of life.
Clinical manifestations include pain,
a palpable soft tissue mass and pathologic fracture.
Conventional chondrosarcoma has a strong predilection for the pelvis,
the femur,
proximal humerus and ribs.
Within long tubular bones it is usually located in the metaphysis or metadiaphysis.
Imaging findings
Conventional radiography
Radiographic appearance differs with histological grade,
reflecting the different aggressiveness.
The spectrum of imaging findings starts with osteolytic lesions difficult to differentiate from enchondromas and ends with the radiographic pattern of high-grade malignant tumors,
with moth-eaten destruction and aggressive periosteal reaction.
Many chondrosarcomas,
mainly those with higher grade of differentiation,
show chondrogenic calcifications.
Continued growth leads to lobulated endosteal scalloping that eventually produces cortical penetration and a soft tissue component (Fig. 22).
Computed tomography
CT allows detection and characterization of matrix mineralization,
particularly when it is in a complex anatomic area.
Evaluation of cortical response (including cortical thickening and periosteal reaction),
endosteal scalloping and soft tissue extension are also well evaluated by CT (Fig. 23).
Magnetic resonance
MR provides the best method for depicting the extent of marrow involvement.
On T1-weighted images,
marrow replacement appears as low to intermediate signal intensity.
The nonmineralized component of chondrosarcoma has high signal intensity on T2-weighted images.
Areas of matrix mineralization have low signal intensity with all pulse sequences.
The lobular architecture typical of all hyaline cartilage neoplasms is commonly seen best at the lesion margin.
The contrast enhancement is typically mild in degree,
with a peripheral and septal pattern (Fig. 24).
Both the depth and extent of endosteal scalloping are well depicted by MR imaging.
Endosteal scalloping causing cortical destruction is commonly seen.
MR is the best radiologic modality to identify soft-tissue extension (which is seen in about 76% of the cases).
The intrinsic characteristics of the soft tissue extension are identical to those of the intraosseous component (Fig. 25).
Clear cell chondrosarcoma
Clear cell chondrosarcoma is a low-grade variant of chondrosarcoma,
accounting for 1 – 2% of all chondrosarcomas.
It is most frequent in the third and fourth decades of life.
Its most frequent location is the epiphyseal region of long bones,
especially of the femur and humerus.
The radiographic appearance is that of a well-defined lytic lesion,
that can have a thin sclerotic rim.
Chondrogenic calcifications occur in approximately one third of cases.
The main differential diagnosis is with chondroblastoma (patient age is an important discriminator between both entities)
Mesenchymal chondrosarcoma
Mesenchymal chondrosarcoma is a rare form of chondrosarcoma characterized by a dimorphic histological pattern with highly undifferentiated small round cells and islands of well-differentiated cartilage.
It is more frequently found in the second and third decades of life.
Mesenchymal chondrosarcoma can originate in bone (approximately in two thirds of cases) and in soft tissue (in one third of cases).
In those cases originating from the bone,
distribution is widespread,
with a preference for the craniofacial bones,
ribs,
iliac bone and vertebrae.
The radiographic manifestations of mesenchymal chondrosarcoma have been described as being similar to conventional chondrosarcomas.
About 75% of mesenchymal chondrosarcomas originating from bone contain chondrogenic calcifications (Fig. 26).
In soft tissue lesions,
granules of chondrogenic calcifications are frequent and can lead to the specific diagnosis.
MR imaging typically shows a well-demarcated mass composed of calcified and non-calcified areas (Fig. 27).
Dedifferentiated chondrosarcoma
Dedifferentiated chondrosarcoma is an entity that consists of two different components: a well-differentiated chondrogenic component,
and a high-grade,
non-cartilaginous component,
frequently malignant fibrous histiocytoma,
fibrosarcoma or osteosarcoma.
They account for 10% of chondrosarcomas and are most frequent in the fifth to ninth decades of life.
Prognosis is poor,
with a 5-year survival rate of only 20%.
Metastases to the lung are common.
Most common sites include pelvis,
femur and humerus.
The typical imaging appearance reflects the presence of the two components: one component shows the characteristics of a well-differentiated chondrogenic tumor,
including chondrogenic calcifications in about 50% of cases; the other component has a highly aggressive pattern,
with penetration of the cortex,
ill-defined margins and a large soft tissue component (Fig. 28).