1.
Introduction
The syndrome of ICH is a single pathophysiological entity of diverse origin.
Usually,
it is characterized by an orthostatic headache,
that is,
one that occurs or worsens with upright posture,
although patients with chronic headaches or even no headache have been described.
In addition to headache,
patients may experience nausea,
vomiting,
anorexia,
neck pain,
dizziness,
horizontal diplopia,
changes in hearing,
galactorrhea,
facial numbness or weakness,
or radicular symptoms involving the upper limb,
all of which are orthostatic in nature.
Making a diagnosis of SIH follows excluding causes of secondary syndrome: however spinal CSF leaks,
spontaneous or following even minimal trauma.
2.Pathogenesis:
The syndrome of spontaneous intracranial hypotension is caused by a reduced cerebrospinal fluid (CSF) volume leading to decreased CSF pressure.
This reduction in CSF pressure is thought to be caused due to a rupture of the arachnoid membrane resulting in the leakage of CSF into the subdural or epidural space.
The primary cause of SIH is an occult spontaneous CSF leak from the spinal canal.
According to the Monroe-Kellie hypothesis,
the sum of the volumes of cerebral tissue,
intracranial blood and CSF is constant in an intact cranium.
Hence,
any CSF leak must be compensated by venous engorgement (not arterial as this is tightly auto regulated) ,
increase in the subdural space and finally sagging and downward displacement of cerebellar tonsils.
Traction on these structures is responsible for some of the other clinical symptoms in SIH.
Reduction in CSF volume causes a reduction in the buoyant force allowing the brain to sag downwards which results in headache which is exaggerated by an upright posture.
This explains the orthostatic nature of the headache in SIH.
3.Epidemiology of SIH:
The incidence has been estimated at 5 per 100.000 per year.
Synonyms for SIH include intracranial hypotension,
CSF leak,
low pressure headache and CSF hypovolemia.
Women are affected more commonly (nearly 2:1) and the peak incidence is around the age of 40 years,
with associations including connective tissue disease,
trivial traumatic event (one third of patients) and acquired degenerative disk disease.
Connective tissue disorders (Marfan,
Ehlers-Danlos syndrome s) that may be associated.
4.Brain MRI findings:
The MRI findings represent the sum of loss of CSF volume and compensatory changes in response to the leakage.
4.1. Thin,
bilateral,
subdural fluid accumulation over the cerebral and cerebellar convexities is commonly seen in about 50% of patients.
They typically do not cause mass effect and represent small hygromas.
Occasionally,
subdural haemorrhage can be seen.
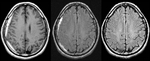
Case report:
A 42 year old previously healthy men awoke with diffuse postural headache associated with nausea,
vomiting and vertigo after make weight exercise.
RMI shows a bilateral subdural collections (Fig. 1)
SIH was diagnosed,
and the patient was treated with lumbar epidural blood patch at L2-L3,
resulting in complete and sustained resolution of symptoms.
4.2 Pachymeningeal (dural) enhancement: is bilateral,
diffuse,
involves both supratentorial and infratentorial compartments and spares the leptomeninges.
This common (in 80% of cases) and striking appearance has been likened to a “felt tip pen” outlining the thickened,
enhancing dura in a diffuse and non-nodular pattern.
It is thought to be caused by engorgement of the small,
thin-walled dilated blood vessels in the subdural zone.
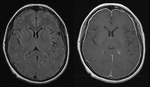
Case report:
A 65 year old women underwent lumbar decompression surgery.
On fourth postoperative day she developed severe postural headache which could berelieved only in head low position.
Magnetic resonance showed diffuse pachymeningeal enhancement (Fig. 2 ).
Over the next few months,
after the discontinuation of steroid treatment,
the patient's symptoms improved to almost complete resolution.
4.3. Dural venous sinus engorgement and Pituitary hyperaemia or enlargement are also due to compensatory increase in the venous blood component to balance the loss in cranial volume and pressure,
but are less constant and less striking signs of SIH.
These are often only appreciated on comparison with post-treatment,
normalized venous structures.
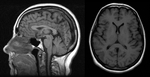
Case report:
A previously healthy 65-year-old woman presented with severe positional headaches,
aggravated by sitting or standing and relieved by lying down.
The MR showed dural venous sinus engorgement and ventricular volume decrease ( Fig. 3)
The patient was diagnosed with spontaneous intracranial hypotension and underwent an epidural blood patch.
After treatment,
the patient reported almost immediate relief from headaches.
4.4 Sagging and downward displacement of the cerebellar tonsils or effacement of prepontine cistern with flattening of the pons against the clivus may mimic a Chiari type 1 malformation or it can be misdiagnosed as increased intracranial pressure from sinister cause such as space-occupying lesions.
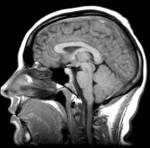
Case report:
Women of 33-year-old.
Headache and neck pain after childbirth triggered by orthostasis.
Accompanied by tinnitus and blurred vision in his right eye.
MR showed minimal displacement of the cerebellar tonsils. (Fig. 4).
5.
Spine MR findings:
Although spinal imaging is not a necessity for the diagnosis of SIH,
these examinations may be ordered because of spinal symptoms caused by the fluid collection or by clinicians unfamiliar with the syndrome who want to exclude a spinal block after an unsuccessful
spinal tap.
MR showed spinal extradural fluid collections. These spinal fluid collections tend to be isointense with CSF on T1- and T2-weighted MR images.
Sometines spinal extradural collections are hyperintense.
The possible cause of the increased signal intensity of the spinal collection may be increased protein content within the collection as compared with CSF.
The origin of the enhancement is uncertain,
but it may represent delayed leakage of contrast material into the collection.
Mild enhancement of the fluid collection or the adjacent dura may occur.
Spinal fluid collections may or may not be symptomatic,
depending on their size and relative mass effect upon the spinal cord or nerve roots.
While the intracranial subdural fluid collections in SIH are believed to be due to CSF hydrostatic changes,
the spinal fluid collections are likely caused by extradural CSF leakage and accumulation.
Case report:
A 25-year-old presented with a 2 week history of positional headaches associated with horizontal diplopia.
A subsequent lumbar puncture revealed a depressed opening CSF pressure of 40 mm H2O,
but extensive studies of the CSF disclosed no other abnormalities.
Serologic studies for collagen-vascular diseases and other systemic conditions were unrevealing.
Brain MRI show a normal structures.
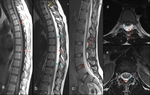
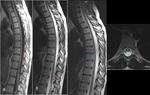
Spinal MR revealed a ventral extradural fliud collection at the cervicothoracic juntion to lumbar columne. (Fig. 5)
We reported a table of patients diagnosed with intracranial hypotension syndrome in the last five years and the MRI findings. (Fig. 6).
6.
Manegement of SHI:
Most cases of SIH resolve with conservative treatment including bed rest,
oral hydration,
and caffeine.
Other strategies used to treat SIH involve the fluid restoration to increase CSF or eliminating the leakage site.
Strategies to increase CSF volume include intravenous or oral hydration,
increased salt intake,
carbon dioxide inhalation and steroid therapy.
However,
the persistence of postural headache or occurrence of neurological disorders,
calls for definitive therapy.
If conservative management fails,
epidural blood patches are considered to be the safest and most efficacious in treating leakage sites causing SIH. It involves injection of autologous blood into the epidural space. (Fig. 7)
Surgical repair is the last treatment option in patients who do not respond to conservative management and blood patches.
7.
Differential diagnosis:
The differencial diagnosis of the brain MRI findings in SIH is important to consider:
Pachymeningeal enhancement may be seen in:
- metastatic malignant tumor deposits: but these tend to be multifocal and nodular rather than diffuse
- Infectious meningitis: typically affects the leptomeninges rather than pachymeninges.
The differencial diagnosis of spine MRI findings is:
Extramedullary cystic lesions includes:
- epidural hematoma: its not isointensity with CSF on T1-weighted images.
- abscess: usually show thick peripheral enhancement
- arachnoid cyst: are typically intradural extramedullary lesions.
- neurenteric cyst: are also intradural extramedullary and may or may not have associated vertebral body anomalies.