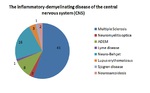
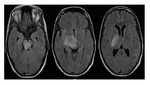
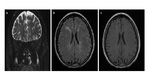
The inflammatory demyelinating diseases identified were as follows: Multiple sclerosis (n = 40) with one case of pseudotumor cerebri syndrome (n = 1); Devic's disease or neuromyelitis optica (n = 2),
acute disseminated encephalomyelitis (n = 8),
Lyme disease (n = 1); neuro-Behçet's disease (n = 16); lupus erythematosus (n = 3); Gougerot Sjogren (n = 1); neurosarcoidosis (n = 2).
(Fig 1)
1- Multiple sclerosis:
Multiple sclerosis (MS) is the most common chronic inflammatory demyelinating disease affecting the central nervous system (CNS) of young adults leading,
in most cases,
to severe and irreversible clinical disability.
Clinical presentation:
Clinical course of MS is extremely variable
Most common signs/symptoms
o Variable; initially impaired/double vision of acute optic neuritis
o Weakness,
numbness,
tingling,
gait disturbances
o Loss of sphincter control,
blindness,
paralysis,
dementia
o Cranial nerve palsy; usually multiple,
(CNs 5,
6 most common)
o Spinal cord symptoms in 80%
Clinical profile: Cerebrospinal fluid (CSF) positive for oligoclonal bands
Diagnostic Criteria for Multiple Sclerosis
* “White-matter lesions disseminated over time and space”
* Clinically definite MS:
- 2 episodes of symptoms
- evidence of 2 white-matter lesions (imaging or clinical)
* Laboratory-supported definite MS:
- 2 episodes of symptoms
- evidence of 1 white-matter lesion
- oligoclonal bands in CSF
* Probable: 2 episodes and either 1 lesion or oligoclonal bands.
Imaging Studies
- CT is not sensitive for MS plaques.
They may occasionally be seen as low attenuation areas on CT but are often not detected.
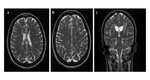
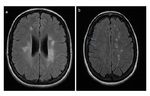
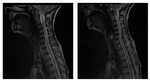
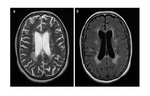
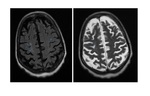
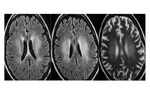
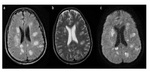
- MR imaging criteria for diagnosis of multiple sclerosis (MS) are based on the demonstration of disease dissemination in time and space on dual-echo (T1 and T2 weighted images) and contrast-enhanced T1-weighted MR images.
- In patients with established MS,
dual-echo,
fluid-attenuated inversion-recovery (FLAIR),
and contrast-enhanced T1-weighted MR images are useful for defining a more complete picture of disease burden.
(Fig 2 and Fig 3).
- The MRI lesions may not,
however correlate with clinical symptoms
Typical location of MS Plaques
* Periventricular Region
* Juxtacortical areas
* Corpus callosum
* “Dawson’s fingers”: a lymphocytic infiltration along periventricular medullary veins
* Other locations include:
- Visual Pathways
- Posterior fossa
- Cervical spine
Differential Diagnosis: Acute disseminated encephalomyelitis (ADEM)
- Autoimmune-mediated vasculitis;
- Subacute myelo-optic neuritis (SMON)
- Lyme disease
- Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL)
- Sjögren disease
- CNS lupus
- Neurosarcoidosis
- Antiphospholipid antibody syndrome
- Susac syndrome
2- Demyelinating pseudotumor:
Considered as an acute fulminant variant of multiple sclerosis.
This Inflammatory demyelinating pseudotumor (IDP) is an uncommon inflammatory lesion of the central nervous system (CNS) that clinically and radiologically mimics a neoplasm,
but dramatically responds to steroids.
The clinical form of pseudo-tumor is often acute with severe deficit.
The tumor-like form of MS is characterized by the presence of extensive demyelinating lesion greater than 2 cm in diameter simulating a tumor.
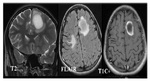
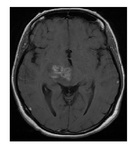
Imaging aspects (Fig.
4):
- intracranial expansive process
- hyposignal on T1-weighted image and hypersignal on T2 weighted image.
- incomplete ring-enhancing lesion with discrete perilesional edema
- with insignificant mass effect
- usually associated with intraparenchymal inflammatory demyelinating lesions of the CNS.
3 pathological forms have been identified:
► Marburg:
- Younger patients,
febrile prodrome,
clinically fulminant
- One or more large lesions,
- Inconsistently and partially enhanced by the Gadollinium.
► Schilder (diffuse sclerosis).
- Rather affects children;
- One or more roughly symmetrical lesions located in centrum semiovale and measuring at least 2 to 3 cm;
- Histopathology: similar to that present in the MS.
► Balo's (concentric sclerosis):
- Lesion composed by an alternation concentric bands of normal myelin "bulb onion" shape
- Signs in favor of extensive demyelinating lesions:
• The clinical context;
• The association with other demyelinating lesions ;
• Small mass effect relative to size of the lesion.
• An incomplete ring enhancement ==> horseshoe open to the gray matter +++.
Diagnosis is made upon biopsy,
which shows alternating bands of myelinating and demyelinating nerve fibers in the white matter of the central nervous system.
Imaging tests are used to rule out space-occupying lesions such as tumors.
Differential Diagnosis:
- Glioma low or high grade;
- Lymphoma;
- Metastatic neoplasm;
- Brain abscess
- Ischemic stroke.
3- Neuromyelitis optica (also known as Devic’s disease):
Neuromyelitis optica is an idiopathic,
uncommon,
severe,
demyelinating disease of the central nervous system that preferentially affects the optic nerve and spinal cord.
Diagnostic Criteria for Neuromyelitis Optica (NMO)
► Required criteria:
- Transverse myelitis
- Optic neuritis
► Supportive criteria (at least two of the following three elements):
1) MRI brain nondiagnostic for MS
2) MRI spinal cord lesion extending over ≥3 vertebral segments
3) NMO-IgG seropositivity
Clinical features alone are insufficient to diagnose Devic’s neuromyelitis.
The cornerstone clinical syndromes of NMO are optic neuritis and acute transverse myelitis.
Occasionally,
these events will occur simultaneously but usually they evolve months to years apart.
CSF analysis and MR imaging are usually required to confidently exclude other disorders.
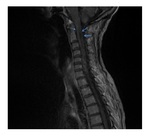
Spinal cord MR imaging shows extensive cervical or thoracic tumefactive myelitis,
involving more than three vertebral segments on sagittal and much of the crosssection on axial T2-weighted images (Fig.
5),
which sometimes enhance with gadolinium for several months.
These spinal cord lesions can progress to atrophy and necrosis,
leading to syrinx-like cavities on T1-weighted images (Fig.
6).
Differential Diagnosis:
- Multiple sclerosis
- Acute disseminated encephalomyelitis
- Adrenomyeloneuropathy
- Sjögren disease
- Systemic lupus erythematosus
- Antiphospholipid syndrome
- CNS vasculitis
4- Acute disseminated encephalomyelitis (ADEM):
Acute disseminated encephalomyelitis (ADEM) is an acute,
monophasic inflammatory demyelinating disease affecting the central nervous system,
which usually follows an infection or vaccination.
The disease is characterised by multifocal white matter lesions on neuroimaging.
Clinical manifestations:
- ADEM is usually a disease of children and young adults that typically occurs 1 to 4 weeks after a febrile illness or a vaccination.
- The neurologic symptoms may begin from 10 days before to 6 weeks after the infection.
They generally begin soon after the exanthem clears and the initial fever subsides.
- ADEM manifests with low-grade fever,
headache,
meningismus,
generalized seizures,
drowsiness,
and encephalopathy
- Multifocal neurologic signs and symptoms may develop,
with visual loss,
hemiparesis,
paraparesis,
ataxia,
sphincter disturbances,
sensory level,
choreoathetosis,
and myoclonus.
- In fulminant cases,
increased intracranial pressure with tentorial herniation,
resulting in death within few days.
Imaging features: Neuroimaging is extremely valuable in establishing the diagnosis of ADEM.
- CT Scan is generally normal at onset and usually becomes abnormal 5–14 days later.
The typical computed tomographic appearance is that of low attenuation,
multifocal lesions in the subcortical white matter.
- Demyelinating lesions of ADEM are better visualised by MRI,
which usually exhibit no mass effect and can be seen scattered throughout the white matter of the posterior fossa and cerebral hemispheres.
Involvement of the cerebellum and brainstem is more common in children.
- Characteristic lesions seen on MRI appear as patchy areas of increased signal intensity on conventional T2-weighted images and on fluid attenuated inversion recovery sequence (FLAIR) (Fig.
7).
Few MRI lesions may enhance after gadolinium administration.
Extensive perifocal oedema may be seen.
MR Spectroscopy: N-acetyl Aspartate (NAA) low within regions of prolonged T2
Differential Diagnosis:
- Multiple sclerosis
- Autoimmune-mediated vasculitis
- Aging brain with hyperintense WM lesions
- Neuro- Behçet
- Fabry disease
5- Lyme disease:
Lyme disease is a multisystemic disease caused by the spirochete Borrelia burgdorferi.
It is transmitted by ixodid ticks.
Lyme disease may affect many systems,
such as the skin,
joints,
heart,
eye,
and nervous system.
Clinical presentation:
- Most common signs/symptoms
o Early localized: Fever,
myalgias,
headaches,
petechial rash (palm,
soles)
o Early disseminated: Erythema migrans,
arthralgias,
myalgias,
fever,
adenopathy
o Late: Arthritis,
carditis,
scleroderma-like lesions,
CNS lesions,
increased intracranial pressure.
- Clinical profile: Confirmation of diagnosis: ELISA,
PCR
Radiologically,
central nervous system involvement in Lyme disease has generally been described as consisting of nonspecific foci in the white matter in the brain.
Lyme disease MRI scans showing hyperintensive signal areas in the white matter and/or the brain stem,
on T2-weighted images,
especially in periventricular white matter,
spinal cord (Fig.
8).
On T1 C+: Enhancement of CN 7 (including root entry zones).
Differential Diagnosis:
- Multiple sclerosis
- Vasculitis
- Neuro Sarcoidosis
- Lacunar Infarct
6- Neuro-Behçet's disease:
Behçet’s disease is a multisystemic inflammatory disease characterized by recurrent oral aphthae,
uveitis,
and genital ulcers.
This disease may involve vessels (especially veins and pulmonary arteries),
joints,
gastrointestinal system and central nervous system besides the initially defined triad.
Although liver,
kidneys,
heart and peripheral nerves are relatively less affected in Behçet’s disease course.
Two patterns of CNS involvement have been described,
including direct parenchymal involvement and cerebrovascular involvement.
Neurological involvement in Behçet’s disease manifests about five years after the onset of systemic findings,
is seen 3-4 times more commonly in males compared to females and usually presents with central nervous system (CNS) involvement with extremely rare peripheral nerve and muscle involvement.
Clinical manifestations:
- Behçet’s disease manifests with headache and fever.
- Neurological examination often reveals ataxia,
dysarthria,
hemiparesis and bilateral pyramidal findings.
- Usually sphincter dysfunction and behavioral changes or cognitive impairment precedes or accompanies neurological involvement.
Imaging features on MRI:
- Scattered,
asymmetric,
subcortical white matter lesions without cortical involvement (Fig.
9).
o Nodular enhancement in acute phase (Fig.
10)
o Predilection for midbrain
- Increased ADC,
similar to ADEM
- Venous sinus thrombosis can be seen as non-parenchymal Neuro-Behçet’s disease.
Differential Diagnosis:
- Multiple sclerosis
- Meningoencephalitis
- Brain tumor
7- Lupus erythematosus:
Systemic lupus erythematosus (SLE) is a multisystem autoimmune connective tissue disorder with various clinical presentations.
SLE affects many organ systems,
including the central and peripheral nervous systems and muscles.
Central nervous system (CNS) lupus is a serious but potentially treatable illness,
which still presents very difficult diagnostic challenges.
The clinical manifestations of neurolupus: The American College of Rheumatology (ACR) has proposed specific criteria for the diagnosis of neurolupus
- Headaches are common (including migraine and idiopathic intracranial hypertension)
- Aseptic meningitis
- Cerebrovascular disease
- Demyelinating syndrome
- Movement disorder (chorea)
- Myelopathy
- Seizure disorder Acute confusional state
- Anxiety disorder
- Cognitive dysfunction
- Mood disorder
- Psychosis
Imaging studies:
- T2 weighted images
o Four patterns of involvement
• Focal infarcts
• Multiple T2Weighted Image hyperintensities(microinfarctions) (Fig.11).
• Focal areas of increased intensity,
primarily in grey matter
• Diffuse steroid-responsive subcortical lesions
o Acute lesions on T2 weighted image suggesting active Neuropsychiatric Systemic lupus erythematosus (NPSLE): New infarct,
discrete gray matter lesions,
diffuse gray matter hyperintensities,
and cerebral edema
- FLAIR: Multifocal white matter hyperintensities
- T1 C+: Acute/active CNS lesions may enhance
- MR Angiography (MRA): Can confirm thrombotic lesions of extracranial/intracranial vessels
- Positron emission tomography (PET) scanning and MR spectroscopy (MRS) promise greater sensitivity for cerebritis.
Differential Diagnosis:
- Multiple sclerosis
- Antiphospholipid antibodies (non-SLE)
- Lyme encephalopathy
- Small vessel cerebrovascular disease
- Susac syndrome
- Other vasculitides (such polyarteritis nodosa (PAN),
Wegener,
Behçet disease,
syphilis,
Sjogren disease)
8- Gougerot Sjögren syndrome:
Sjögren syndrome (SS) is a chronic,
inflammatory,
autoimmune disease,
characterised by lymphocytic infiltration and destruction of the exocrine glands,
leading to dry mouth and dry eyes.
Peripheral nervous system disease,
manifesting commonly as peripheral sensory neuropathy or,
rarely,
as mononeuritis multiplex.
About 20% of patients with primary SS have central nervous system manifestations,
including focal brain lesions,
diffuse brain lesions and spinal cord lesions.
Diagnostic of neurological involvement in Sjögren syndrome (SS):
- MRI abnormalities are common in SS and usually consist in hyperintense areas in the subcortical and periventricular white matter on T2- weighted and fluid-attenuated inversion recovery (FLAIR) sequences (Fig.12).
These lesions are less pronounced than in patients with multiple sclerosis and rarely touch the basal ganglia or the cerebral cortex.
- Cerebrospinal Fluid (CSF) may be useful to classify some manifestations and is also necessary to the differential diagnosis.
CSF is abnormal with a higher number of lymphocytes,
increased level of proteins,
and intrathecal synthesis of gamma globulins in aseptic meningoencephalitis.
- Skin or Neuromuscular Biopsy may be helpful in some cases.
Differential Diagnosis:
- Neurosarcoidosis
- Lipoproteinemia (types-II,
-IV and -V),
- Chronic graft-versus-host disease,
- Lymphoma,
- Amyloidosis,
- Infection by hepatite C virus (HCV) or human immunodeficiency virus (HIV).
9- Neurosarcoidosis:
Sarcoidosis is an inflammatory granulomatous disorder affecting virtually all organs,
particularly the lungs and lymph nodes.
The nervous system,
both central and peripheral,
is involved in 10% of patients.
Clinical presentation:
Neurosarcoidosis can present with various clinical forms,
depending on its localisation and speed of progression.
It can present with involvement of the cranial,
or peripheral,
nerves,
meningitis,
diffuse brain or spinal lesions responsible for seizures,
psychiatric symptoms or various forms of paralysis.
Diagnostic of neurological involvement in neurosarcoidosis:
- Analysis of cerebrospinal fluid in patients with central nervous system involvement indicates nonspecific lymphocytic inflammation.
- The diagnostic value of measuring angiotensin-converting-enzyme (ACE) levels in cerebrospinal fluid is controversial.
- Imaging Findings: Sarcoidosis can involve any part of the nervous system and its coverings.
* Leptomeningeal involvement is perhaps the most typical form of neurosarcoidosis.
This is generally seen as thickening and enhancement of the leptomeninges on contrast-enhanced T1- weighted images and the enhancement may be nodular or diffuse.
* Hypothalamus and pituitary involvement may be seen with basilar leptomeningeal involvement or as an isolated finding.
* Intraparenchymal lesions can be reported as multiple nonenhancing periventricular white matter lesions with high signal intensity on T2-weighted images (Fig.
13) or as an enhancing parenchymal mass lesions on T1-weighted contrast enhanced image.
* Cranial nerve involvement may occur along with leptomeningeal involvement or as an isolated finding.
* CT imaging is unnecessary for most patients with sarcoidosis.
CT is indicated when the chest radiograph is atypical for sarcoidosis.
Differential Diagnosis:
- Meningitis
- Metastases
- Meningioma
- Infundibular histiocytosis