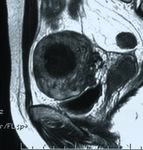
Materials and methods:
We proceeded UFE on 900 cases. The location of uterine leiomyomas in our cases is shown in table1. We inserted tip of the catheter into the bilateral uterine artery under the X-ray guidance approached from right femoral artery.
After the angiography of the uterine artery,
we injected embolizing material(gelatin sponge particle) into the uterine artery carefully.
The end point of embolization was determined by the blood flow disappearance of ascending uterine artery and retention of horizontal uterine artery. It is not all,
the majority of patients underwent MRI before and after UFE.
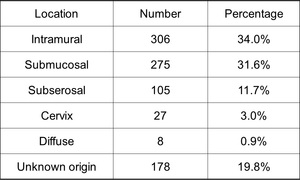
Table 1: location of the uterine leiomyomas in 900 cases
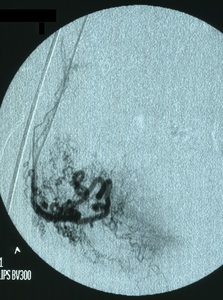
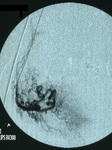
Fig. 1: Angiography of the right uterine artery
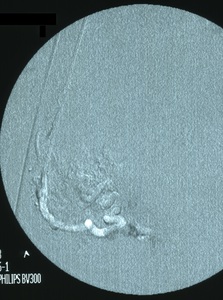
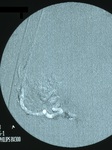
Fig. 2: Angiography of the right uterine artery
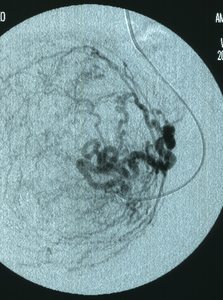
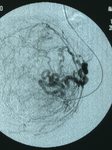
Fig. 3: Angiography of the left uterine artery
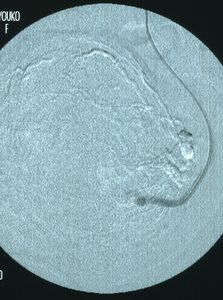
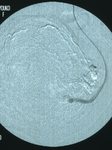
Fig. 4: Angiography of the left uterine artery
Imaging findings:
1.
Access and technique of UFE for various location,
type and size of uterine leiomyoma
Intramural or submucosal leiomyoma tends to show significant reduction after UFE compared with subserosal leiomyoma.
The terminal branch of the uterine artery is the intramural artery,
called the arcuate artery.
The arcuate arteries terminate in medial peripheral arteries and radial arteries.
Radial arteries feed the central two-third of the myometrium,
and may give greater blood flow to the central submucosal branches.
Cervical leiomyoma has a tendency to the poor reduction after UFE.
Cervix of uterus is fed mainly by the cervicovaginal artery,
known to be smaller than the size of the perifibroid arteries.
And there is anatomic variation and anastomoses in the cervix with vaginal artery and middle hemorrhoidal artery,
this may be associated with the less reduction of the cervical leiomyoma after UFE.
Uterine leiomyomas which show high intensity on T2-weighted images are more likely to show obvious reduce,
it is expected that these leiomyomas have a lot of component of smooth muscle and are hypervascular.
We could not detect the correlation between size of leiomyoma and reduction rate.
2.
Strategy of UFE for expecting mothers
479 patients hoped to have children,
it is important to reserve the fertility for such patients.
So,
we embolized their uterine arteries mildly; as blood flow of uterine artery downs,
blood flow of ovarian artery becomes dominant.
16 patients of 900 became pregnant successfully after UFE.
14 patients were pregnant spontaneously,
and 2 patients conceived by in vitro fertilization(intracytoplasmic sperm injection).
3.
Pre and post UFE MR imagings
In the whole cases performed MR before and after UFE,
reduce of the uterine fibroids was seen in 85.5%,
95.1%,
97.8%,
and 98.1%,
1month,
3months,
6months,
and 1year after UFE respectively(Table2). Patients had symptoms related uterine leiomyoma before UFE,
such as abdominal pain,
hypermenorrhea,
dysmenorrhea,
anemia,
pollakiuria,
and constipation.
Except 2 patients,
improvement of symptoms was seen in almost patients in spite of volume increase of some leiomyomas after UFE.
We could not find out the relationship between the degree of the reduction of the uterine leiomyomas and improvement in the patients' symptoms.
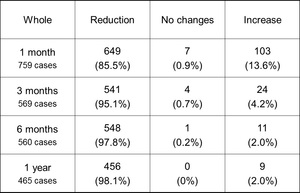
Table 2: Volume changes of the uterine leiomyomas after UFE
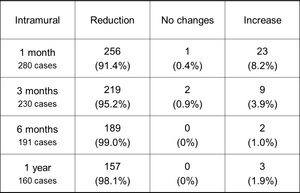
Table 3: Volume changes of the intramural uterine leiomyomas after UFE
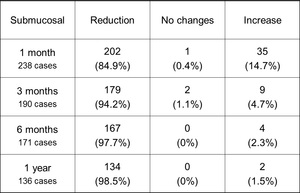
Table 4: Volume changes of the submucosal uterine leiomyomas after UFE
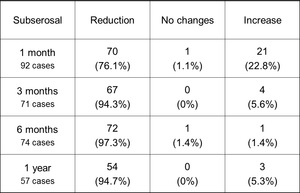
Table 5: Volume changes of the subserosal uterine leiomyomas after UFE
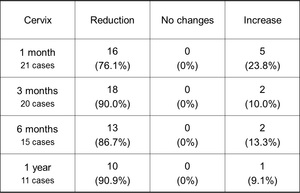
Table 6: Volume changes of the cervix uterine leiomyomas after UFE
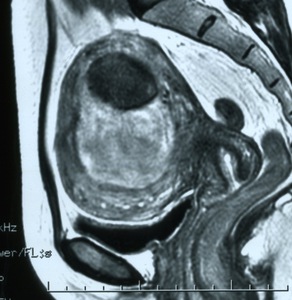
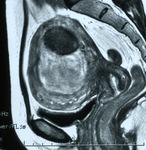
Fig. 5: MR T2-weighted image of the uterine leiomyoma before UFE
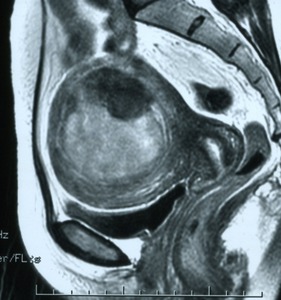
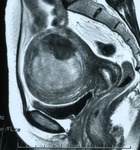
Fig. 6: MR T2-weighted image of the uterine leiomyoma after UAE 1 month
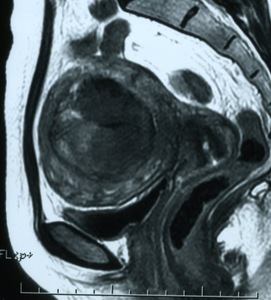
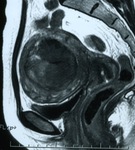
Fig. 7: MR T2-weighted image of the uterine leiomyoma after UAE 3 months
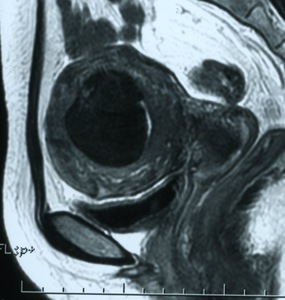
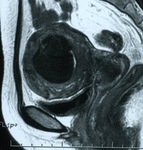
Fig. 8: MR T2-weighted image of the uterine leiomyoma after UAE 6 months
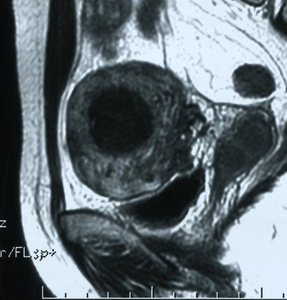
Fig. 9: MR T2-weighted image of the uterine leiomyoma after UAE 1 year
4.
Rare complications of UFE
Complications of UFE are rare,
including bleeding,
infection,
disorder of menoxenia,
etc.
We experienced infection after UFE in 18 cases(2%) and amenorrhea in 6 cases(0.07%).