All patients who underwent to cardiovascular procedures beetwen august 2007 and may 2012 were elegible for this retrospective,
IRB study.
Inclusion criteria were cardiovascular procedures; 2) age > 18 years; 3) brain CT and/or MRI because of postoperative neurologic symptoms.
Exclusiom criteria was interval time between onset of symptoms and brain CT/MR of 60 days or more.
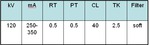
CT were performed on a 64 detector–row CT scanner (VCT 64; GE). CT protocol is showed in table1. MR were performed on a 1.5 T scanner (Signa HDXT,
GE).
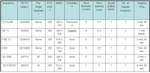
MR protocol is showed in table 2. Images were independently evaluated by two experienced radiologists on PACS.
CT and MR scans were classified as 1) no acute abnormalities; 2) ischemic stroke; 3) hemorrhagic stroke
Ischemic strokes were classified as:1) one small stroke (less than 5 mm in diameter); 2) multiple small strokes; 3) one not small stroke; 4) multiple not small strokes; 5) coexisting small and not small strokes.
Not small strokes were further classified as one-third of arterial territory affected and less than one-third of arterial territory affected.
Stroke side and number were recorded.
A control group was selected in order to identify predictors of neurological complications.
Control group included 115 cardiac surgery patients without neurological complications.
Patients were selected according to age,
sex and type of intervention.
For each patient,
epidemiological,
anamnestic and surgical risk factors were evaluated.
Epidemiological risk factors included hypertension (defined as systolic pressure > 140 mm Hg and diastolic pressure >90 mm Hg); diabetes; lipid profile (total cholesterol,
high density lipoprotein,
triglycerides); smoking status (nonsmoker,
current smoker or former smoker).
Anamnnestic risk factors inclueded previous cerebrovascular accident and internal carotid artery (ICA) stenosis.
Degree of stenosis was classified into the following categories: 1) absent (PSV less than 125 cm/sec and no visible plaque or intimal thickening); 2) <50% stenosis (PSV less than 125 cm/sec and visible plaque or intimal thickening); 3) 50%–69% stenosis (PSV equal to 125–230 cm/sec and visible plaque); 4) 70% stenosis to near occlusion (PSV greater than 230 cm/sec and visible plaque and luminal narrowing); 5) near occlusion (demonstration of a markedly narrowed lumen at color Doppler US and not applicable velocity parameters); 6) total occlusion (no sonographically detectable patent lumen and no flow at color Doppler US) (Society of Radiologists in Ultrasound Consensus Conference criteria).
Surgical risks factors included use cardio-pulmonary by- pass (cardio-pulmonary bypass time,
aortic clamp time,
beating heart,
hypothermic circulatory arrest,
intraoperative hemofiltration); cardioplegia (route and type); rhythm (defibrillation required at weaning and cardiac rhythm at sternal closure); surgery time excluding CPB time; intra-aortic balloon pump requirement; number of by-pass; complicated weaning CPB; 8) Vasoactive drugs requirement; 9) severe hypotension during surgery; transfusion (erythrocytes,
plasma,
platelets).
Risk factors were compared among study group and control group.
Quantitative data were compared using t test.
Categorical variables were compared using the Fisher exact test.
Non parametric data were compared using Mann-Whitney test.
A stepwise multiple logistic regression was used to identify stroke risk factors. A p value of less than 0.05 was considered significant.
Statistical analysis was performed with software (SPSS; version 12.0,IMB,
Italy).