Keywords:
Neuroradiology brain, Cardiac, MR, CT, Surgery, Ischaemia / Infarction, Transplantation
Authors:
F. Agnello, S. Caruso, V. Carollo, F. Crinò, G. Marrone, G. Mamone, G. Floridia, A. Luca; Palermo/IT
DOI:
10.1594/ecr2013/C-1922
Results
2121 patients underwent to cardiac surgery at our institution.
115/2121 (5.4%) patients (86 males; 52 females; mean age,
60.3 years; range,
6-86) underwent CT or MR because of postoperative neurologic symptoms.
Mean interval between CT/MR and surgery was 10.4 days (range 0-60).
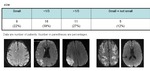
43/115 (39%) patients had abnormal CT/MR findings.
43/45 (95%) had ischemic strokes.
2/48 (5%) had hemorrhagic strokes.
70/115 (63%) patients had no acute abnormalities.
Details are showed in tables 3-5. No statistically significant difference in epidemiological risk factors between groups.
There was no statistically difference in incidence of previous cerebrovascular accidents between groups.
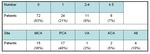
Incidence of ICA stenosis was significantly higher in study group than in control group (table 6). Incidence of bilateral ICA stenosis was higher in study group than in control group (p<0.01)(table 7). There was a statistically significant difference in complicated weaning CPB and cardiac rhythm at sternal closure between groups (p<0.01) (table 8).
Other surgical risk factors were not statistically significant different between groups. Multivariate analysis showed that bilateral ICA occlusion of any grade was the only predictive factor of neurological complications in cardiac surgery patients increasing 24.6 times the risk (odd ratio,
24.66; 95% confidence interval,10.96-55.48,
p<0.01).