Depending on the patient’s condition either a chest x-ray or a CT will be performed.
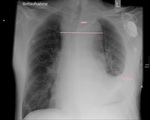
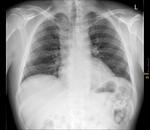
Chest x-ray is taken in upright p.a.
and left lateral position or in supine position if not otherwise possible.
The radiograph is evaluated specifically for signs of mediastinal hematoma such as:
- widening of the mediastinal shadow
- altered configuration of the aorta
- deviation of the trachea or a nasogastric tube to the right of the spinous process of T4.
- loss of the aorticopulmonary window.
- presence of pleural effusion,
typically on the left.
- left apical cap.
- depression of the left main-stem bronchus > 40° below the horizontal.
- aortic wall thickness indicated by the aortic shadow beyond the intimal calcification
- displacement of the calcification in the aortic knob.
the best positive predictive value of mediastinal hematoma is the combination of 3 signs:
loss of aortic contour,
tracheal deviation and mediastinal widening.
Unfortunately the accuracy in predicting thoracic aortic injury in chest radiographs is very poor with a specificity ranging from 1-60%.
Plain films can be sufficient if the aortic arch is clearly and normally visualized in an p.a.
view.
Exception seen in Fig.
9.
MDCT contrariwise exceeds a sensitivity of 98% for blunt traumatic aortic injury.
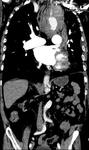
Direct and indirect signs for BAT in thoracic CT.
Indirect signs:
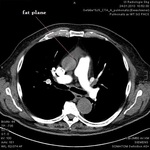
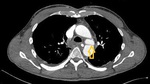
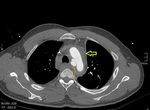
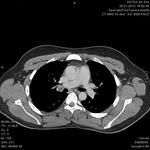
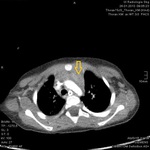
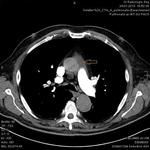
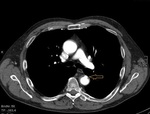
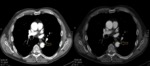
Mediastinal hematoma appears as soft tissue attenuation surrounding the mediastinal structures.
The location of hematomediastinum has diagnostic significance e.g.
surrounding the aorta or retrosternal.
periaortic hemorrhage in direct communication with the aorta (missing fat plane) is highly suspicious for aortic injury
if fat plane is visible or retrosternal location – the hematoma can be caused by a fracture of sternum or vertebral body,
by venous mediastinal bleeding,
or bleeding from side branches of the aorta.
Hematoma can track down to the level of the diaphragm or retrocrural.
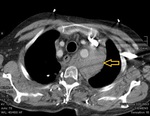
Direct signs:
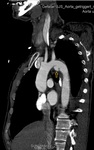
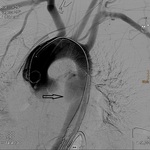
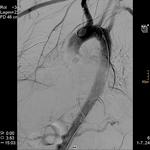
aortic pseudoaneurysm
aortic contour / diameter variation
intimal flap
intramural thrombus
contrast extravasation – rare.
Common Pitfalls:
Breathing / pulsation / motion artefacts
Thymus,
pericardial recesses
ductus diverticulum
aortic diverticulum
penetrating atherosclerotic ulcer (PAU)
atherosclerotic aortic plaque
Treatment:
For the decision of further treatment it is important to classify 3 groups of patients.
|
Risk factor
|
Hemodynamic
|
Findings
|
Treatment
|
|
low
|
stable
|
minor lesions (local dissection without signs of perforation,
intimal flaps,
mural hematoma)
|
conservative
repeated CT-scans,
hypotensive therapy
|
|
mid
|
stable
|
major lesions (extended dissections,
contained rupture
|
endovascular intervention
Stentgraft
|
|
high
|
unstable
|
free aortic rupture
|
open surgery
|