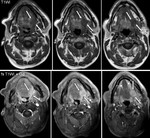
MRI is the imaging modality of choice for the study of a patient with hypoglossal nerve palsy.
It supplies superior soft-tissue contrast and allows direct visualization of the different segments of the nerve.
Multiple sequences are available to study the nerve and each has specific advantages according to the segments being studied.
For the intra-axial segment or above (nuclear or supra-nuclear lesions) a brain protocol is used with fast spin-echo (FSE) T2WI of the brain and T1WI of the skull base.
After intravenous injection of gadolinium T1WI are repeated.
High resolution T1W images pre- and post-contrast with fat suppression allow further anatomical characterization of the remaining segments.
The use of contrast is especially useful in infectious/inflammatory pathology where abnormal enhancement of the nerve may be the only presentation of the disease.
The hypoglossal nerve should be routinely studied in the axial and coronal plane.
Sometimes the sagittal plane may be useful,
e.g.
for distal lesions involving the floor of the mouth or the tongue base.
The imaging approach of a patient with hypoglossal nerve palsy consists of analyzing the different anatomical segments of the nerve and recognizing the most common differential diagnosis in each.
The most common diseases affecting each segment are discussed below and are listed in table 1.
Unilateral atrophy of the tongue musculature is the most important radiologic feature of hypoglossal nerve palsy.
Imaging changes in the tongue after damage to the hypoglossal nerve vary according to the time gone by between the initial nerve lesion and the imaging examination.
MRI is the most useful imaging modality to characterize these various muscle changes.
In the subacute phase of denervation,
the tongue is hyperintense on T2WI and hypointense on T1WI,
mainly due to edema.
Enhancement of the denervated part can be seen after intravenous gadolinium administration.
In the chronic phase,
as fatty infiltration progresses,
the tongue volume on the affected side will decrease.
On MRI the affected tongue will have high signal on both T1WI and T2WI.
Once tongue atrophy is identified at imaging,
systemic evaluation of the hypoglossal nerve should be performed.
MEDULLARY SEGMENT:
Pathology of this segment of the nerve is frequently associated with damage to other nuclei,
resulting in a complex lower cranial neuropathy.
Disease that involves both hypoglossal nerve nuclei leads to bulbar palsy with complete paralysis of the tongue.
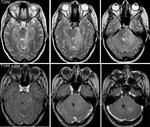
The most common pathology in this region is infarction,
due to ischemia or hemorrhage.
Neoplasms are also among the most common causes and may be primary or secondary.
Most frequent are metastases followed by gliomas.
Metastases have a variety of imaging appearances but should always be thought of.
Gliomas are heterogeneous lesions with high signal intensity on T2WI,
causing expansion of the brainstem (Fig.
5).
Other less common pathologic processes of inflammatory,
infectious or demyelinating nature may also occur,
such as multiple sclerosis,
amyotrophic lateral sclerosis or poliomyelitis.
CISTERNAL SEGMENT:
As described in the anatomical layout of the hypoglossal nerve,
there is a close relationship between the nerve and the vertebral artery.
Thus,
vertebrobasilar pathology or anatomic variants may cause compression of the rootlets resulting in paralysis.
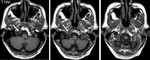
Other pathologic entities in this region include skull base bony pathology such as clival tumors,
meningioma,
osteomyelitis or pathology involving the odontoid such as rheumatoid arthritis,
trauma or Chiari malformation (Fig.
6).
Basal meningitis or subarachnoidal hemorrhage with exsudation and organization can also compromise the nerve.
Primary tumors of the hypoglossal nerve,
although uncommon,
may also affect the cisternal portion of the nerve.
SKULL BASE SEGMENT:
Tumors,
both benign and malignant,
and trauma may damage the hypoglossal nerve along its course through the skull base.
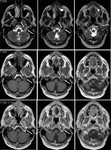
Tumors of the skull base may affect the hypoglossal canal by expansion or destruction.
The most common malignant tumors are metastasis from breast,
lung and prostate cancer and direct extension of nasopharyngeal carcinoma through the skull base.
Benign tumors include peripheral nerve sheath tumors (such as schwannoma),
glomus tumors,
and meningiomas (Fig.
7).
Primary bony tumors such as giant cell tumors or osteogenic sarcomas may also involve the hypoglossal canal.
Infection of the skull base (pseudomonas infection,
tuberculous osteomyelitis) is even much rarer,
but should also be included in the differential diagnosis,
especially in the diabetic or immunocompromised patient.
EXTRACRANIAL SEGMENT:
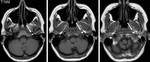
In the carotid space the hypoglossal nerve lies in close contact with the internal carotid artery and internal jugular vein.
As a result,
ectasia and aneurysm of the carotid artery,
as well as arterial dissection and jugular thrombosis can compress the nerve and lead to palsy (Fig.
8).
However,
the most common cause of hypoglossal nerve palsy in the carotid space are malignant tumors,
both primary and secondary pathologies,
including squamous cell carcinoma,
lymphoma,
salivary gland tumors and metastatic disease.
Benign tumors such as paragangliomas and lipomas should also be in the differential diagnosis.
Iatrogenic lesions (endarterectomy,
vascular punction) or trauma (stab,
gunshot wounds or infection spreading from other neck spaces) may also cause dysfunction of the twelfth cranial nerve.
The most common cause of dysfunction in this segment is nerve damage due to squamous cell carcinoma of the base or lateral regions of the tongue (Fig.
9).
Odontogenic lesions such as abscesses or iatrogenic damage after tooth extraction are other causes to be considered.