This poster was previously presented in Spanish at the 2012 Congreso Nacional SERAM (Granada)
Keywords:
Lung, Oncology, Interventional non-vascular, CT, Percutaneous, Biopsy, Neoplasia
Authors:
J. A. Gallego Sánchez, N. Riera Bevia, B. Pomares Rey, Z. Sánchez Acevedo, E. Ramos Gavila, E. Alsina Seguí; Elche/ES
DOI:
10.1594/ecr2013/C-2018
Methods and Materials
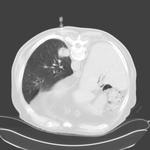
49 biopsies of thoracic lesions were performed under CT-guided coaxial technique with a 19G introducer needle.
Access to the lesions was as perpendicular as possible to the pleura and chose the shortest approach that crossed the least amount of lung parenchyma and avoided vessels,
bronchia,
bullae and fissures.
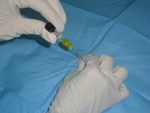
The skin entry was sterilised with povidone-iodine solution and infiltrated with lidocaine.
The introducer needle (19G) was placed in the proximal edge of the lesion with patient’s breathing suspended. Fig. 1
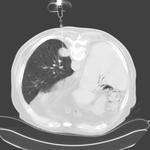
The inner stylet was removed and the 20G semiautomatic cutting needle (SCN) pushed to the end of the guiding cannula with a throw length of 10 mm or 20 mm according to the lesion size and structures behind the lesion. Fig. 2
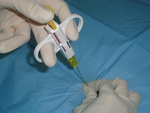
The SCN was rotated 90 ° after each pass and an average of 3.5 core specimens for histology were obtained.
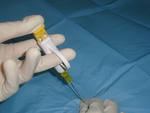
Fig. 3 Fig. 4
The 20G SCN was then exchanged for a FNA (22G) through the coaxial system Fig. 5 performing two passes and sending the samples in smears and within syringes with ethanol for cytological analysis.
After each pass the inner stylet was placed inside the introducer needle to prevent air embolism.
The punctures were performed without an on-site cytopathologist.
If the patient experienced hemoptysis during procedure,
biopsy was discontinued.
Lung CT scan was performed after biopsy and an erect chest radiograph was performed 3 hours after to rule out complications.
The results were correlated with surgical specimens if available or follow-up of the lesions.
Those without a specific diagnosis but stable for two years were considered benign.